Chemotherapy-induced nausea and vomiting (CINV) is one of the most feared and detrimental adverse events for patients resulting from chemotherapy that can decrease the patient’s quality of life.1,2 CINV is common in patients who receive highly emetogenic chemotherapy (HEC).3 Several studies have estimated that 30% to 60% of patients who are prescribed HEC will have CINV despite routine prophylaxis, which raises concern.4,5 Many antiemetic regimens are available, but differences exist in prescribing patterns, and variable success rates have been reported.6 In addition, with the exception of serotonin antagonists, inconsistencies among national practice guidelines, especially in terms of delayed CINV, highlight a lack of a standardized approach in the use of antiemetic regimens in clinical practice.3,7,8
A pharmacist-run CINV protocol may improve adherence to national guideline recommendations for the use of antiemetic drugs: the availability of multiple guidelines and guideline-consistent CINV prophylaxis may ultimately have positive effects on patient outcomes.9 One study described the implementation of a pharmacist-run CINV protocol that resulted in no difference in outcomes in CINV rates compared with standard of care (managed by physicians), but demonstrated the advantage of standardization of inpatient management of CINV by a pharmacist.10
Conversely, outpatient management of CINV is further complicated by operational limitations, such as cost, prior authorizations, and patient adherence. The objective of this current study was to achieve 90% complete response rates to antiemetic regimens through a pharmacist-run protocol in the outpatient setting over a 6-month period.
Methods
This study was conducted in the outpatient hematology oncology clinic at Boston Medical Center. This is an urban academic medical center and the largest safety-net hospital in the New England area, with 57% of patients being from underserved populations and 32% of patients whose primary language is other than English.11 More than 60 patient infusions are administered daily at the center’s outpatient oncology clinic. Patients are managed using a multidisciplinary approach, in collaboration with medical oncologists and hematologists, surgical oncologists, and radiation oncologists. Weekly tumor board meetings are held to discuss complicated patient cases.
Oncology pharmacists are well-integrated into these teams and are actively sought out for their expertise in pharmacotherapy. The healthcare system at Boston Medical Center uses Epic as its electronic health record (EHR) system. The EHR system incorporates treatment plans for all patients who receive chemotherapy, including the chemotherapy itself, nursing communication, supportive care, and infusion reaction sets.
In early August 2017, a Work Group consisting of 4 oncology-trained pharmacists, 1 attending medical oncologist, and 1 attending hematologist developed a structured pharmacist-run CINV protocol (see Appendix Figure) that was adherent to the national clinical practice guidelines.3,7,8
The Work Group applied the Institute for Healthcare Improvement Model for Improvement framework to guide the efforts to reduce the rates of CINV throughout the study period.12 Our study was exempt from Institutional Review Board review, because it qualified as a quality improvement study. Adults who were receiving a new HEC regimen, as recommended by the National Comprehensive Cancer Network (NCCN) guidelines for antiemesis,3 were eligible for management using this protocol and were included in this study.
All patients receiving a new HEC regimen, regardless of the intent of chemotherapy and their organ function, were included in the study during the 6-month period, to account for real-world variability in the ambulatory setting. Patients were only excluded from the study if they were receiving a chemotherapy regimen that was not considered to be HEC. The pharmacist-run management began in the outpatient oncology clinic at Boston Medical Center on November 1, 2017, and completed on April 30, 2018. Although data collection ended after a 6-month period, the pharmacist-run protocol remains active at the institution.
Before the implementation of this improvement protocol, antiemetic medication prescribing was handled solely by attending physicians. Providers often consulted the pharmacists on complex cases or when there was a problem in obtaining medications. Antiemetic drugs were often prescribed and sent to outside pharmacies, which would create a gap in communication if a prior authorization was needed. Patients would frequently leave the clinic after their chemotherapy, without picking up their medications, because of various barriers, such as lack of transportation or a lack of understanding the importance of taking antiemetic drugs.
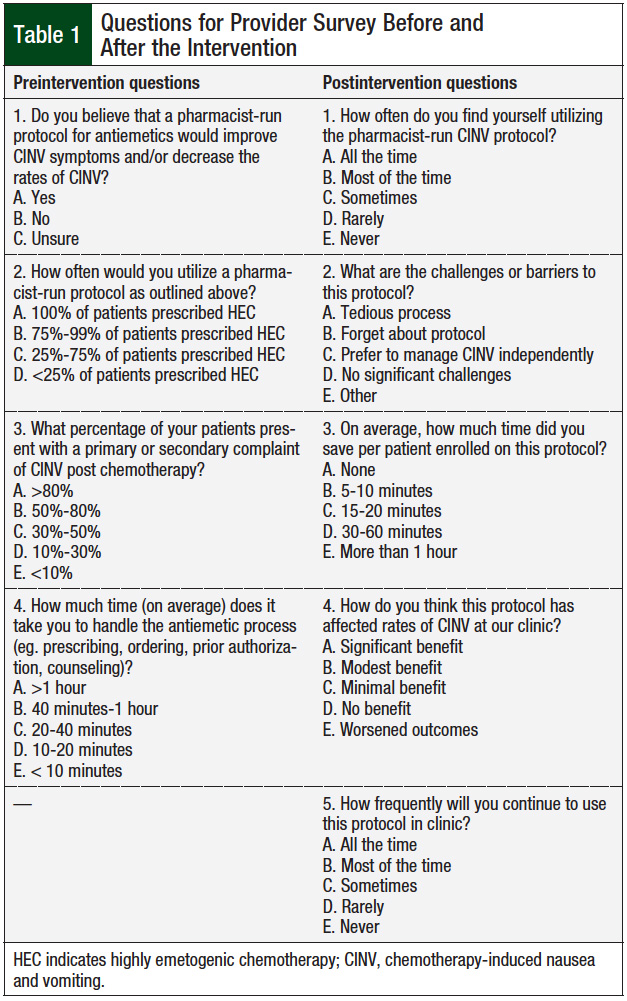
To encourage the need for an intervention to improve patient outcomes by reducing CINV rates, providers at Boston Medical Center were surveyed before and after the intervention implementation to assess the current incidence of CINV at the institution (Table 1). We completed a retrospective chart review of patients who received a new HEC regimen 3 weeks before the study intervention (from August 10, 2017, through August 31, 2017) to confirm the data that were solicited from the providers. The rates of complete response to antiemetic drugs (defined as no CINV at days 3 and 5 after starting the new HEC regimen) served as the baseline data for this study.
The Intervention Protocol
The providers formally referred patients who were starting an HEC regimen to pharmacists by messaging within the EHR of Boston Medical Center. The pharmacists who were responsible for referrals were full-time clinical pharmacy specialists and oncology clinical pharmacists who were overseeing our satellite oncology pharmacy. For the patients who were not referred by the day (<24 hours before) of starting the HEC regimen, the pharmacists reminded the providers of the need for a formal referral.
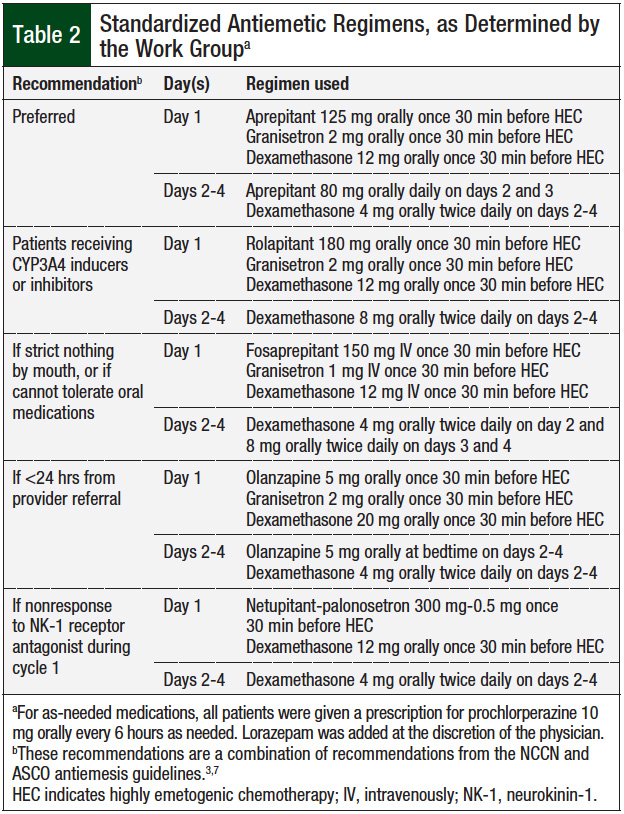
The pharmacists initiated the protocol for eligible patients by prescribing antiemetic drugs according to a standardized regimen that was determined by the Work Group (Table 2). This regimen incorporated recommendations from the NCCN3 and the American Society of Clinical Oncology.7 The pharmacists completed all prior authorizations (with assistance from pharmacy liaisons) for the antiemetic drug regimen, prescribed the antiemetic drugs, delivered medications dispensed by Boston Medical Center’s outpatient pharmacies, and performed comprehensive medication counseling, with an interpreter when appropriate. Medication counseling included reviewing the dosing, administration, and toxicity of the antiemetic agents, as well as reviewing the chemotherapy regimen itself.
On days 3 and 5 of the HEC cycle, patients were called to be assessed for CINV, in an attempt to capture CINV at the most common times of the chemotherapy cycle. All patients were asked standardized questions about the presence of symptoms, the date and time of the symptoms, the number of days the symptoms were present, the number of scheduled antiemetic agent doses missed, the need for emergency department or clinic visit, and the number of breakthrough doses used. If patients were not reached on both days, an assessment of their symptoms was done at the next patient encounter.
Any follow-up calls scheduled for the weekend were done on the following Monday, regardless of the day of the cycle. For patients who reported symptoms via a telephone call, a follow-up appointment was scheduled with the pharmacist at the next infusion. The pharmacists assessed adherence and/or toxicity, adjusted the antiemetic regimen accordingly, and counseled the patients.
Our pharmacist-run protocol incorporated 3 plan-do-study-act (PDSA) cycles. The first PDSA cycle (weeks 1-6) piloted the initial implementation of this pharmacist-run protocol. The second PDSA cycle (weeks 7-12) integrated an electronic order entry for the initiation of the protocol by providers, who would place an order for the pharmacist protocol in lieu of a formal referral. This cycle also limited enrollment if an order or a referral to a pharmacist was placed less than 24 hours from the start of chemotherapy. Before PDSA cycle 2, pharmacists could self-enroll patients in the pharmacy protocol by notifying the attending physician. The third and final PDSA cycle (weeks 13-24) involved educating specific providers to increase the utilization of the protocol.
Outcome Measures
The study’s outcome measure was complete response to antiemesis drugs (as measured by the absence of emesis). The complete response rates were calculated by dividing the number of patients who did not have CINV at day 3 and 5, by the total number of patients being treated that week. As a marker to confirm a high success rate throughout this initiative, an initial goal of 90% response (ie, lack of emesis) rate was chosen.
The percentage of patients enrolled in the pharmacist protocol and the percentage of orders placed by providers (and not pharmacists) served as the process measures. The time spent by the pharmacist to complete the protocol was recorded as a balancing metric. This included the time spent prescribing antiemetic drugs, delivering the medications, patient counseling, and follow-up phone calls with patients. These metrics were analyzed in 2-week time intervals and were plotted as run charts to display the results over time. Each 2-week assessment included the number of patients (or patient-cycles) who were treated in that 2-week time frame.
A total of 3 PDSA cycles were implemented in an attempt to improve the process continuously over time for the number of patients treated in each 2-week interval. Therefore at each 2-week interval, we assessed the state of the protocol for the total of patients at that time point (which was less than the total of 46 patients enrolled in the entire study period).
The data collection started on November 1, 2017, and was completed on April 30, 2018. The providers were surveyed preintervention and postintervention to assess the perceived impact of a pharmacist-run protocol on patient outcomes and provider time.
Results
Of 14 attending physicians, 8 completed a baseline survey before the intervention (Table 1). A total of 4 of the 8 physicians stated that 10% to 30% of their patients presented to the clinic or emergency department with a primary or secondary complaint of CINV, despite routine prophylaxis; the remaining 4 providers estimated that <10% of their patients did so. Furthermore, 4 of the 8 providers stated that it takes >20 minutes per patient for the management of CINV.
The same 8 providers who responded to the preintervention survey were later asked to complete a postintervention survey (Table 1). Of these 8 providers, 7 (88%) stated that there was significant benefit from this intervention, whereas 1 provider stated a modest benefit.
Thus, none of the providers indicated that there was no benefit or a worse outcome from the use of this intervention. Of the 8 providers, 4 (50%) estimated that 15 to 20 minutes of their time was saved per patient with the protocol, and an additional 3 (38%) providers estimated that they saved more than 30 minutes per patient.
A retrospective review of patients receiving new HEC regimens in a 3-week time frame before study implementation showed that 7 of 20 (35%) patients had CINV and 13 of 20 (65%) patients had a complete response to antiemetic drugs at baseline.
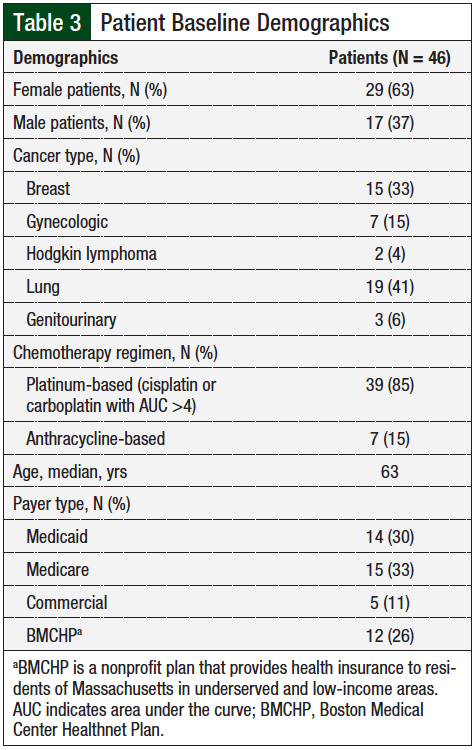
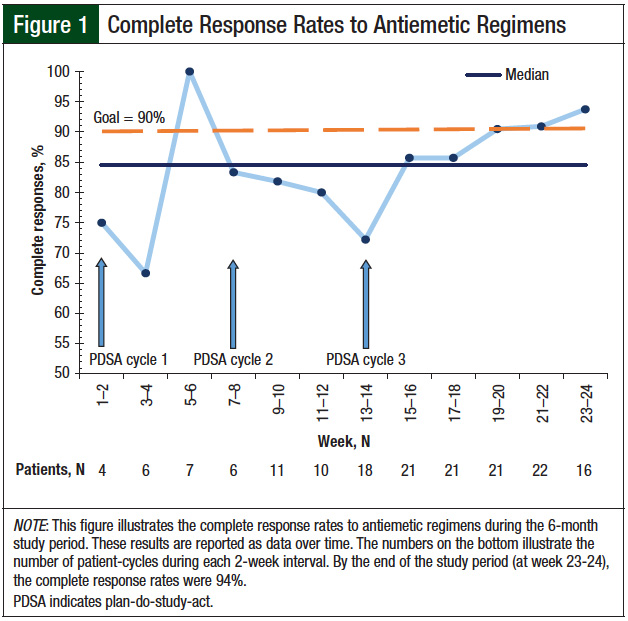
A total of 46 patients (and a total of 163 patient-cycles of HEC) were managed through the newly enacted pharmacist protocol over the 6 months of the study. The patients’ baseline demographics are shown in Table 3. During the first month of the study protocol (the first PDSA cycle), the complete response rates were stable, at 75% (3 of 4 patient-cycles) during week 1 to 2 and 67% (4 of 6 patient-cycles) during week 3 to 4 (Figure 1). By the end of the study period, the average weekly number of patients on the protocol ranged from 10 to 20.
A second PDSA cycle was implemented to increase the providers’ use of the protocol. The complete response rates for patients in each 2-week interval after the implementation of cycle 2 were 83% (5/6), 82% (9/11), 80% (8/10), and 72% (13/18). These declining complete response rates were thought to be attributed to an inadequate understanding of how to enroll patients in the pharmacy protocol. Thus, PDSA cycle 3 was designed to improve the understanding of the enrollment process and the electronic order referrals with certain providers.
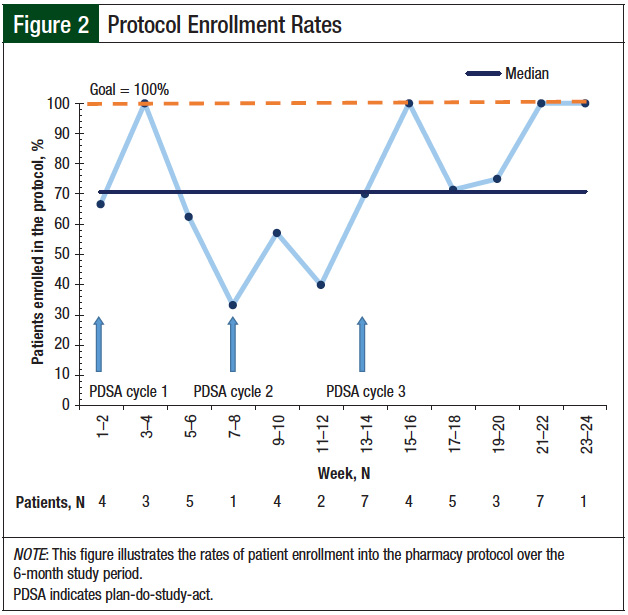
After PDSA cycle 3, the complete response rates to antiemetic regimens revealed an increasing trend to 94% (15 of 16 patient-cycles), which met the goal of >90% by the end of the study evaluation period (Figure 2).
The percentage of patients placed on the pharmacy protocol gradually increased from 67% (2/3) to 100% (7/7). The percentage of patients who were referred exclusively by providers had increased from 50% (2/4) during week 1 to 2 to 100% (7/7) by week 23 to 24. The average weekly new enrollment for the protocol was 2.16 patients.
A total of 163 patient-cycles of chemotherapy were assessed. Patient follow-up phone calls on day 3 and day 5 were successful for 76% of patient-cycles (124 of 163 patient-cycles). Patients who were not reached on day 3 and day 5 of their chemotherapy cycle (24%; 39 of 163 patient-cycles) were assessed for CINV at their next clinic follow-up. The average time the pharmacist spent per patient encounter was 45.7 minutes.
Discussion
This quality improvement project demonstrated that a pharmacist-run CINV protocol achieved high complete response rates for CINV reduction in an outpatient oncology clinic. The initial goal to reach a complete response of 90% was reached and was consistently above the providers’ projections from the preintervention survey, which highlights the clinical impact of pharmacists as extenders to providers in a healthcare system. Furthermore, after 3 PDSA cycles, the trends in the rates of complete response increased over the 6-month period, suggesting the success of the initiative.
Initially, a brief decrease in our primary outcome was seen after cycle 2 of the PDSA (ie, the implementation of the electronic order entry), which was attributed to the providers’ misunderstanding of a new function within the EHR system and of how to use the function properly. Hence, cycle 3 of the PDSA was implemented to address education regarding the use of the electronic order. The time spent by pharmacists completing this protocol translated to substantial time-savings for providers in the clinic, which was also reflected in the postintervention surveys. If extrapolated, this time-savings allows a higher volume of patients to be seen in the clinic without any additional financial burden to the hospital.
The balancing metric served to gauge the sustainability of this protocol. An increased workload for clinic pharmacists was expected without additional support; initially, the time spent by pharmacists was adequately managed. As noted earlier, by the end of the study, the average weekly number of patients in protocol ranged from 10 to 20. This included new patients as well as patients who were previously enrolled in the protocol. Therefore, to sustain this protocol in a real-world oncology setting, follow-up phone calls were removed from the protocol at the completion of this project to alleviate increased workload for pharmacists.
The follow-up phone calls served as a means to capture CINV at the most vulnerable time, and successful trends after 3 PDSA cycles suggested that eliminating phone calls would not lead to decreases in the complete response rates. However, if the patient reported CINV at the next clinic visit, the provider was encouraged to notify the pharmacist for follow-up recommendations. Future direction to expand this protocol into practice will include the incorporation of an automated pharmacy protocol order in all prebuilt treatment plans for HEC.
The pharmacist-run protocol allowed for pharmacists’ involvement in meeting all the challenges associated with prescribing of antiemetic drugs. The pharmacists were able to overcome several operational challenges within the healthcare system, including the high cost of prescription medications, prior authorizations, and language barriers. Some data suggest a lack of prescriber awareness of the costs of frequently used medications in clinical practice.13 The pharmacists used copay assistance programs to optimize antiemetic medications that were prescribed for patients to reduce the cost burden of drugs with high copayments.
Prior authorizations for antiemetic medications were required for 20 (43%) of the 46 patients who were on this protocol. Pharmacy liaisons completed the prior authorizations for protocol orders placed more than 24 hours before administering chemotherapy, for improved access. If prior authorizations could not be completed in a timely fashion, the pharmacists opted to use an olanzapine-based treatment regimen, as determined by the Work Group.
The pharmacists attempted to hand deliver all antiemetic drugs to the patients’ bedsides before leaving their chemotherapy appointments. Finally, the pharmacists used language interpreter services for 27 (59%) of the 46 patients during counseling sessions, which highlights the challenge of language barriers within healthcare.
Limitations
There are several limitations to this quality improvement initiative. The sample size used in this quality improvement project was small (N = 46). However, this quality improvement project reflects a real-world experience with a pharmacist-run protocol, which may be extrapolated to institutions with similar volume.
The symptoms of CINV in our baseline assessment were evaluated using a retrospective chart review. Therefore, the telephone calls at days 3 and 5 might have overestimated the rates of CINV when symptoms were captured at the patient’s most vulnerable time.6
In addition, patients referred for management through the pharmacy protocol within 24 hours before the first chemotherapy cycle might not have had prior authorizations completed and might have received alternative therapy using an olanzapine-based regimen from our standardized protocol as opposed to a neurokinin-1 antagonist.
Finally, patients who were not reached via day 3 and/or day 5 follow-up phone calls were assessed for CINV at the next chemotherapy or nadir visit, which might have underestimated the incidence of CINV in our study.
Conclusion
This pharmacist-run CINV-related protocol was successful in standardizing the management of CINV and in minimizing the rates of CINV that resulted from the use of an HEC regimen in our outpatient oncology clinic. Furthermore, the protocol demonstrated the value of having pharmacists on the forefront of healthcare for challenging patient populations, without the setbacks of operational limitations such as language barriers, prior authorizations, and high copayments. The use of this pharmacist-run initiative has now become a standard practice in our ambulatory clinic 1 year after the implementation of the intervention and could be adopted by other institutions. The continued growth of multidisciplinary approaches will remain vital, given the expansion of healthcare in the United States and the limited available economic resources.
Acknowledgment
The authors thank Adrian Zobniw, Phuong Dao, Alexamil Rodriguez, and Naomi Ko for their support of this project.
Author Disclosure Statement
Dr Hughes, Dr Vose, Mr Shah, and Dr Jhaveri have no conflicts of interest to report.
References
- Passik SD, Kirsh KL, Rosenfeld B, et al. The changeable nature of patients’ fears regarding chemotherapy: implications for palliative care. J Pain Symptom Manage. 2001;21:113-120.
- Salihah N, Mazlan N, Lua PL. Chemotherapy-induced nausea and vomiting: exploring patients’ subjective experience. J Multidiscip Healthc. 2016;9:145-151.
- Berger MJ, Ettinger DS, Aston J, et al. NCCN Guidelines Insights: Antiemesis, version 2.2017: featured updates to the NCCN Guidelines. J Natl Compr Canc Netw. 2017;15:883-893.
- Cohen L, de Moor CA, Eisenberg P, et al. Chemotherapy-induced nausea and vomiting—incidence and impact on patient quality of life at community oncology settings. Support Care Cancer. 2007;15:497-503.
- Rapoport BL. Delayed chemotherapy-induced nausea and vomiting: pathogenesis, incidence, and current management. Front Pharmacol. 2017;8:19. doi.org/10.3389/fphar.2017.00019.
- Rao KV, Faso A. Chemotherapy-induced nausea and vomiting: optimizing prevention and management. Am Health Drug Benefits. 2012;5(4):232-240.
- Hesketh PJ, Kris MG, Basch E, et al. Antiemetics: American Society of Clinical Oncology Clinical Practice Guideline update. J Clin Oncol. 2017;35:3240-3261. Erratum in: J Clin Oncol. 2018;36:1459.
- Roila F, Molassiotis A, Herrstedt J, et al; for the participants of the MASCC/ESMO Consensus Conference Copenhagen 2015. 2016 MASCC and ESMO guideline update for the prevention of chemotherapy- and radiotherapy-induced nausea and vomiting and of nausea and vomiting in advanced cancer patients. Ann Oncol. 2016;27(suppl 5):v119-v133.
- Aapro M, Molassiotis A, Dicato M, et al; for the PEER investigators. The effect of guideline-consistent antiemetic therapy on chemotherapy-induced nausea and vomiting (CINV): the Pan European Emesis Registry (PEER). Ann Oncol. 2012;23:1986-1992.
- Elshaboury R, Green K. Pharmacist-driven management of chemotherapy induced nausea and vomiting in hospitalized adult oncology patients. A retrospective comparative study. Innov Pharm. 2011;2:Article 52. doi.org/10.24926/iip.v2i3.235.
- Boston Medical Center. About us. www.bmc.org/about-us. Accessed June 13, 2018.
- Langley GJ, Moen RD, Nolan KM, et al. The Improvement Guide: A Practical Approach to Enhancing Organizational Performance. 2nd ed. San Francisco, CA: Jossey-Bass; 2009.
- Cogdill B, Nappi JM. Assessment of prescribers’ knowledge of the cost of medications. Ann Pharmacother. 2012;46:200-207.