Patients with cancer account for 20% of venous thromboembolism (VTE) cases in the United States, and these patients are at a 4- to 7-fold increased risk for VTE compared with people without cancer.1 Since the 2003 publication of the landmark CLOT (Randomized Comparison of Low-Molecular-Weight Heparin versus Oral Anticoagulant Therapy for the Prevention of Recurrent Venous Thromboembolism in Patients with Cancer) clinical trial, which compared low-molecular-weight heparins (LMWHs) with a coumarin therapy,2 the treatment of choice for cancer-associated thromboembolism has been LMWHs. Patients often struggle with adherence to these therapies, however, because of cost and the inconvenience of daily or twice-daily injections.3,4
Direct oral anticoagulants (DOACs) may serve as an alternative means of anticoagulation in this patient population.3 These agents are available as once- or twice-daily oral medications, and for the treatment of cancer-associated thromboembolism, the rate of patient adherence is greater using DOACs than LMWHs.3,5 Several studies have investigated the use of rivaroxaban for cancer-associated thromboembolism, ranging from case reports to a randomized controlled trial.4,6-10 In general, studies show that patients using rivaroxaban for cancer-associated thromboembolism have reduced risk for VTE recurrence but increased risk for bleeding compared with LMWHs.4,7-10 Fewer data exist for the use of apixaban and edoxaban for cancer-associated thromboembolism.11-13
The National Comprehensive Cancer Network (NCCN) recently updated its Guidelines for Cancer-Associated Venous Thromboembolic Disease, recommending DOACs as the preferred agents for the treatment of cancer-associated thromboembolism in patients without gastric or gastroesophageal lesions, and maintaining LMWHs as the preferred agents in patients with gastric or gastroesophageal lesions.5
Despite a growing body of literature supporting the efficacy of DOACs for cancer-associated thromboembolism, guidelines for the treatment of VTE in patients with cancer from the European Society of Cardiology14,15 and the American College of Chest Physicians16 still recommend LMWHs as the preferred agents for the treatment of cancer-associated thromboembolism, and the American Society of Clinical Oncology guidelines for VTE prophylaxis and treatment in patients with cancer now recommend rivaroxaban, edoxaban, or LMWHs for the treatment of VTE.17
No consensus has been reached among national guidelines regarding the role of DOACs for the treatment of cancer-associated thromboembolism.5,14-17 In addition, studies have raised concerns about increased bleeding risk with DOAC use in certain types of cancer, including gastrointestinal (GI) cancer.10,11 With emerging evidence to support the use of DOACs for cancer-associated thromboembolism,4,6-13 clinicians are increasingly prescribing these medications for VTE treatment in patients with cancer.
Because patients with cancer pose unique challenges, including variable renal and hepatic functions, baseline hypercoagulability, and increased risk for medication interactions, real-world data are needed to assess the appropriateness of DOACs for cancer-associated thromboembolism. This study adds to the body of knowledge to evaluate the efficacy and safety of DOACs, including apixaban, edoxaban, and rivaroxaban, in the treatment of cancer-associated thromboembolism.
Our study aimed to address important real-world clinical variables—such as obesity, complications of dosing DOACs in patients with variable renal and hepatic function; the impact of concurrent, interacting medications; and the role of cancer type—that may influence the selection of anticoagulation therapy for patients with cancer-associated thromboembolism within the Cleveland Clinic health system.
The primary objective of this study was to assess the incidence of treatment failure caused by VTE recurrence or major bleeding in patients receiving DOACs for cancer-associated thromboembolism. The secondary objectives included assessment of the incidence of DOAC discontinuation or switching to a non-DOAC anticoagulant and the average time to treatment failure.
Methods
This retrospective chart review included patients who were diagnosed with cancer and cancer-associated thromboembolism and received treatment with apixaban, edoxaban, or rivaroxaban between October 1, 2017, and August 31, 2018.
The 4 largest Ohio hospitals within the Cleveland Clinic health system were selected as study sites because of the presence of oncology clinics at these sites. This study was approved by the Institutional Research Review Board.
We identified patients via a query of the electronic medical record (EMR) for patients seen at 1 of the 4 oncology clinics with a diagnosis code for cancer and deep-vein thrombosis (DVT) or cancer and pulmonary embolism (PE) who had a prescription for apixaban, edoxaban, or rivaroxaban during the study period. For study inclusion, patients had to be aged ≥18 years; have had a diagnosis of cancer and received treatment at 1 of 4 oncology clinics; have had a diagnosis of DVT, PE, or both; and have had a prescription for apixaban, edoxaban, or rivaroxaban after the index VTE.
Patients were excluded if they did not have an active malignancy; if the index VTE was diagnosed outside of the study period; if the index VTE was treated using a thrombectomy, insertion of a caval filter, or fibrinolytic agent; if the patient was receiving a DOAC for another indication at the time of the index VTE; or if there was any documentation that the patient never filled or used the DOAC prescription. Patients who were admitted for treatment of the index VTE might have been receiving another anticoagulant agent while inpatient, but patients were excluded from the study if a DOAC was not the initial outpatient therapy prescribed for the index VTE.
Patients were also excluded if they could not be followed for at least 3 months after initiation of the DOAC unless a treatment failure, discontinuation, or switch to a non-DOAC anticoagulant occurred before that time.
The primary outcome was the incidence of treatment failure because of VTE recurrence or major bleeding, and secondary outcomes included discontinuation or switching to a non-DOAC anticoagulant and the average time to treatment failure.
Baseline data collected from the EMR at the time of the initial DOAC prescription order included age; sex; race; date and type of the index VTE; history of VTE; primary tumor type and stage of disease; Eastern Cooperative Oncology Group performance status or Karnofsky Performance Status; weight and body mass index (BMI); platelet count, serum creatinine, and liver function tests; date of DOAC initiation; and name and dose of DOAC prescribed.
We recorded the presence or absence of a recurrent VTE or major bleeding leading to a change in anticoagulation, or discontinuation of DOAC for any other reason. If a treatment failure occurred, the time to treatment failure; type of recurrent VTE or site of major bleed; therapy selected after treatment failure; and most recent patient information at the time of treatment failure, including weight, BMI, platelet count, serum creatinine and liver function tests were also collected. The Cockcroft-Gault method and patient actual body weight were used to calculate creatinine clearance (CrCl).
A diagnosis of cancer was defined using an inpatient or outpatient International Classification of Diseases, Tenth Revision (ICD-10) code of C00.x-D44.x (excluding C44.x nonmelanoma skin cancer). We defined DVT using an inpatient or outpatient ICD-10 code of I82.210, I82.220, I82.290, I82.3, I82.4x, I82.6x, I82.A1x, I82.B1x, or I82.C1x, and PE was defined using an inpatient or outpatient ICD-10 code of I26.x. Treatment failure was defined as any VTE recurrence or major bleeding leading to a change in anticoagulation therapy. VTE recurrence was defined as an ultrasound report, ventilation or perfusion scan, or computed tomography of the chest showing new or acute PE or DVT, or documentation by any clinician of a new VTE.
Major bleeding was defined using the International Society of Thrombosis and Haemostasis criteria of a bleeding event that is associated with death, occurred at a critical site (intracranial, intraspinal, intraocular, retroperitoneal, intraarticular or pericardial area, or intramuscular with compartment syndrome), resulted in a need for transfusion of at least 2 units of blood, or led to a drop in hemoglobin of at least 2.0 g per deciliter.18
Clinically significant interacting medications investigated in this study were based on a list developed by the pharmacy department of Memorial Sloan Kettering Cancer Center after a review of available literature.9 The prescribing information recommendations for apixaban, edoxaban, and rivaroxaban guided the evaluation of dosing for patients’ renal function.19-21
Statistical Analysis
We performed descriptive statistics using categorical variables reported as N (%) and continuous variables as mean with standard deviation or median with interquartile range. Categorical variables were analyzed by chi-square or Fisher’s exact test, as appropriate. Continuous variables were analyzed by Student’s t-test or nonparametric equivalent based on normality of data distribution.
Normality was determined by a significant Shapiro-Wilk test (P >.05). Statistical analysis was performed using IBM SPSS statistics version 24.0, and the level of significance was set at P <.05 (2-sided).
Results
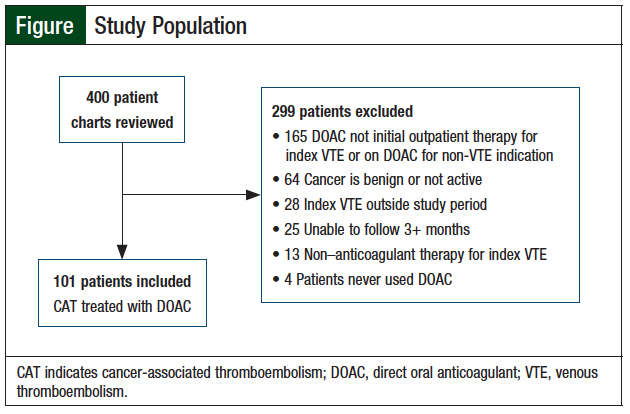
Of the 400 patients who were evaluated for inclusion in this study, 101 were included and 299 were excluded (Figure). A majority of the patients were excluded because the DOAC was not the initial outpatient therapy for the index VTE or patients were receiving DOAC therapy for a non-VTE indication at the time of the index VTE. Other reasons for exclusion included the patient’s cancer diagnosis code indicating benign cancer or cancer in remission; the index VTE occurring outside of the study period; inability to follow a patient for at least 3 months after the initiation of DOAC therapy; nonanticoagulant therapy, such as thrombolytics or caval filters, was used to treat the index VTE; or DOAC therapy was prescribed but never started by the patient.
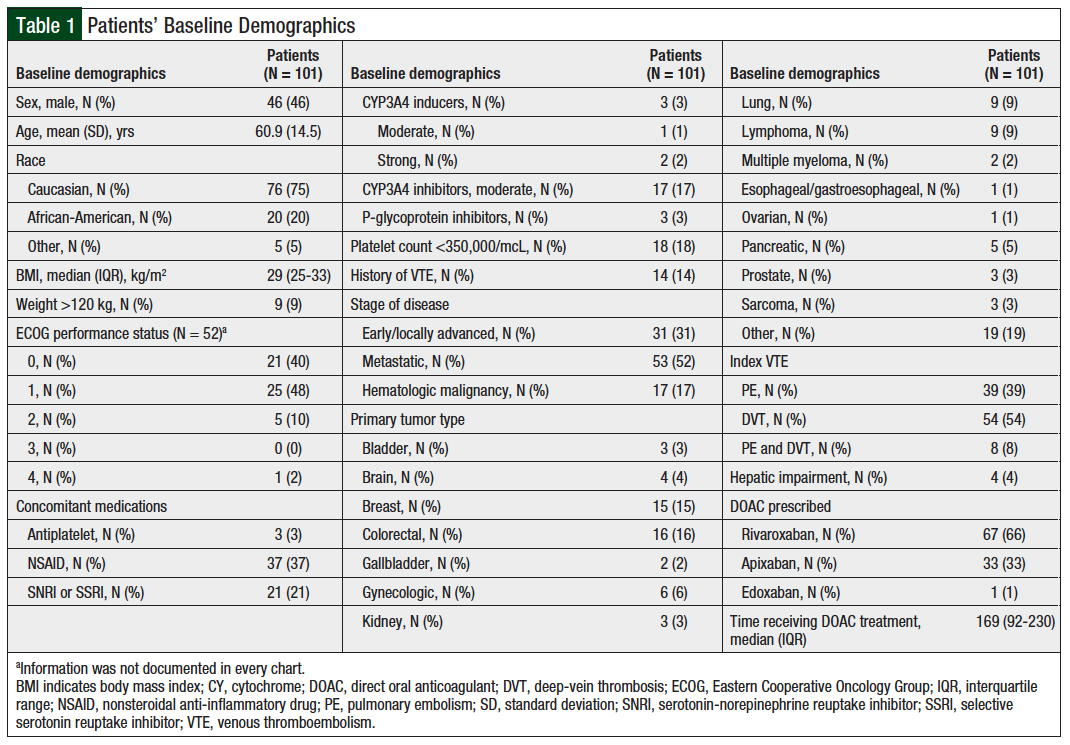
The patients’ mean age was 60.9 years and 75% were Caucasian. In this study, 31% of patients had early or locally advanced solid tumors, 52% had metastatic disease, and 17% had hematologic malignancies. The baseline demographics were similar among those who did and did not have treatment failure, with the exception of BMI, stage of disease, and duration of DOAC treatment (Table 1).
Patients without treatment failure had a higher BMI and longer duration of DOAC treatment (median, 29 vs 25; P = .036, and median, 176 days vs 10 days; P <.001, respectively). Patients were prescribed 1 of 3 DOACs, including rivaroxaban (N = 67; 66%), apixaban (N = 33; 33%), or edoxaban (N = 1; 1%). No difference existed in the type of DOAC prescribed between those who had treatment failure versus those who did not. A greater proportion of no response to treatment was observed in patients with metastatic disease compared with patients with locally advanced or hematologic malignancies; all patients with treatment failure had metastatic disease (P = .019).
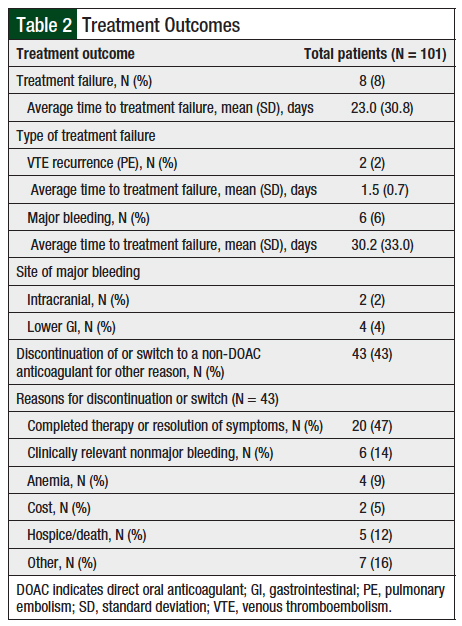
Overall, the incidence of treatment failure in this study was low, at 8%. Recurrent VTE occurred in only 2 patients, which presented as a PE in both cases. Major bleeding occurred in 6 patients, 2 of whom had intracranial bleeding and 4 had lower GI bleeding (Table 2). The average time to treatment failure was 23 days, with VTE recurring an average of 1.5 days into therapy and major bleeding occurring 30.2 days into therapy (Table 2). An additional 43 patients discontinued treatment or were switched to non-DOAC anticoagulants during the study period for reasons other than treatment failure (Table 2).
The most common reasons for therapy discontinuation or switching to a non-DOAC anticoagulant were completion of the course of therapy or resolution of symptoms (47%); clinically relevant nonmajor bleeding (14%); hospice or death (12%); and other (16%) (Table 2). Other reasons for discontinuation included embolic stroke, bleeding risk associated with surgery, or not documented. No differences in treatment failure or discontinuation rates were observed among DOACs used in this study.
The study population included obese patients with weight >120 kg and BMI >40 (N = 9) and patients with hepatic impairment based on aspartate transaminase, alanine transaminase, and/or total bilirubin >3 × upper limit of normal (N = 4). Several patients concurrently used medications that may increase bleeding risk, including antiplatelets (N = 3); nonsteroidal anti-inflammatory drugs (N = 37); selective serotonin reuptake inhibitors or serotonin-norepinephrine reuptake inhibitors (N = 21); and cytochrome (CY)P3A4 or P-glycoprotein inhibitors (N = 20), which would be expected to increase DOAC concentrations, or CYP3A4 inducers (N = 3), which would be expected to decrease DOAC concentrations (Table 1).
A total of 10 patients were prescribed multiple interacting medications; of these medications, all were expected to increase DOAC concentrations. Based on the prescribing information recommendations,19-21 2 patients received prescriptions for DOAC doses outside of those recommended for their renal function at baseline. For patients who had treatment failure, renal function was again assessed at the time of treatment failure, but we found no changes in dosing appropriateness.
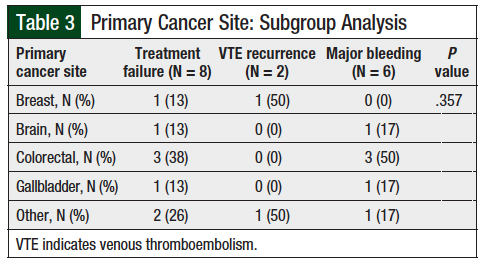
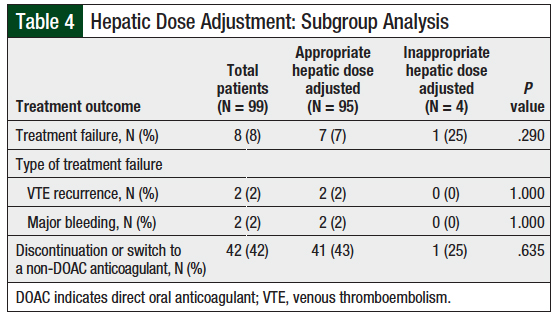
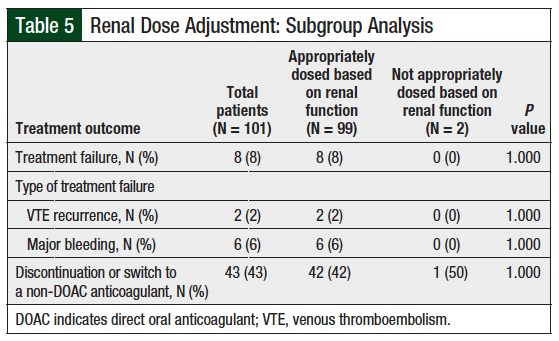
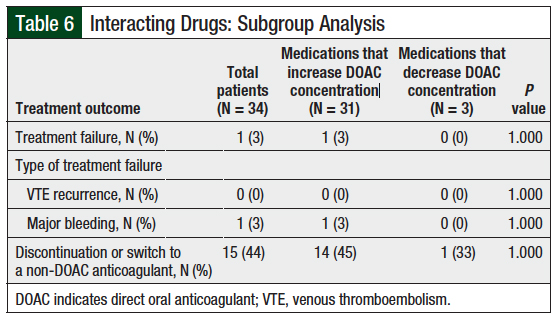
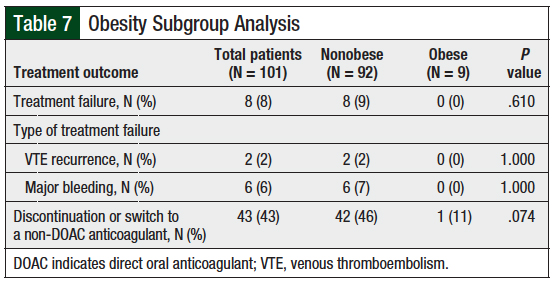
Patients with colorectal cancer were more likely than those with other cancer types to have major bleeding, although this was not statistically significant (P = .357; Table 3). No significant differences in treatment failure were found in subgroup analyses for hepatic impairment (Table 4), inappropriate renal dosage (Table 5), interacting drugs (Table 6), or obesity (Table 7).
Discussion
The principal finding of this study was a low rate of treatment failure, especially because of VTE recurrence, in real-world patients using DOACs for the treatment of cancer-associated thromboembolism. This provides additional evidence to support the use of these medications in patients with active malignancy.
An increasing number of randomized controlled trials have evaluated the use of DOACs for the treatment of cancer-associated thromboembolism.10,11,13 The Hokusai-VTE trial was the first and largest randomized controlled trial comparing a DOAC and an LMWH for the treatment of cancer-associated thromboembolism.11,22,23 In this study of 1050 patients, edoxaban was noninferior to dalteparin with respect to a composite outcome of recurrent VTE or major bleeding. This difference was driven primarily by a reduction in the VTE recurrence rate for edoxaban (7.9% vs 11.3%), but was associated with the cost of a higher major bleeding rate compared with dalteparin (6.9% vs 4%).11
In July 2018, the SELECT-D study was the first published randomized, multicenter clinical trial comparing rivaroxaban with dalteparin in patients with cancer-associated thromboembolism.10 This study reaffirmed the association of DOACs with reduced VTE recurrence rate compared with LMWH therapy (4% vs 11%) and higher comparative rate of bleeding (major bleeding, 6% vs 4%), especially clinically relevant nonmajor bleeding (13% vs 4%).10
Most recently, the multicenter, randomized, superiority ADAM-VTE trial, which aimed to investigate the safety of apixaban versus dalteparin for cancer-associated thromboembolism, was published.13 In this study of 287 patients with cancer and acute DVT, PE, or splanchnic or cerebral vein thrombosis, apixaban demonstrated a lower rate of recurrent VTE (0.7% vs 6.3%) and no significant difference in major bleeding (0% vs 1.4%) or composite bleeding (6.2% vs 6.3%) versus dalteparin.12,13 These studies excluded patients with renal impairment, hepatic impairment, and interacting medications, limiting their applicability to these populations.10-13
Few studies have examined real-world data for the use of DOACs for the treatment of cancer-associated thromboembolism. Clinicians at Memorial Sloan Kettering Cancer Center (MSKCC) implemented a clinical pathway to guide rivaroxaban use in patients with cancer-associated thromboembolism and reported a validation analysis of 200 patients.9 MSKCC listed relative contraindications to rivaroxaban therapy for patients using clinically relevant interacting medications or concomitant antiplatelet medications, including those who had clinically significant liver disease (CrCl <30 mL/min), expected malabsorption at the level of the stomach of small bowel, had active genitourinary or gastrointestinal lesions, had untreated primary central nervous system neoplasms, or who were underweight or obese.9
The validation analysis revealed invasive procedures, transient renal insufficiency, elevated liver enzymes, and thrombocytopenia as complications that affect rivaroxaban therapy in these patients, and indicated that after 6 months of therapy, the incidence of new or recurrent VTE was similar to other studies, at 4.4%, and the incidence of major bleeding was 2.2%.9
Our study is reflective of real-world practice, in which shared decision-making is emphasized and patients who may not be ideal candidates for DOAC use because of these same relative contraindications are prescribed these medications preferentially over other anticoagulants. Despite these factors, patients in our study had a 2% incidence of VTE recurrence and a 6% incidence of major bleeding, a rate of VTE recurrence similar to apixaban and rivaroxaban in these randomized controlled trials, and closely mirroring the bleeding rates seen in the SELECT-D trial using rivaroxaban.10
A retrospective cohort study by Theberge and colleagues examined the outcomes of patients using rivaroxaban for acute or extended treatment and secondary prevention of cancer-associated thromboembolism.4 In this study of 224 patients who started rivaroxaban therapy for acute or extended treatment or secondary prevention of cancer-associated thromboembolism, 4% of the patients had VTE recurrence. Of the 74 patients who started therapy within 7 days of a cancer-associated thromboembolism diagnosis, the rate of VTE recurrence was 2.7%, within a mean time of 2.5 days.4
In our study of patients who are receiving initial outpatient VTE treatment with DOACs, the mean time to VTE recurrence was 1.5 (± 0.7) days. In both studies, the short time between the initial VTE diagnosis and VTE recurrence supports that these recurrence outcomes may represent extensions or incomplete resolution of the initial VTE rather than a recurrence.
Retrospective studies have shown low bleeding rates with rivaroxaban use in patients with cancer-associated thromboembolism, with major bleeding occurring in 5.5% of patients in a study by Pignataro and colleagues,6 and major bleeding events occurring in 4% of patients in a study by Theberge and colleagues, with GI bleeding accounting for the most major bleeding recorded.4
Streiff and colleagues showed similar bleeding rates among groups for patients with cancer-associated thromboembolism using rivaroxaban, LMWHs, or warfarin.7 However, Bott-Kitslaar and colleagues showed that patients with malignancy receiving rivaroxaban for VTE treatment had a higher major bleeding rate compared with patients without malignancy.8
Patients in our study experienced a major bleeding rate of 6%, which is slightly elevated compared with other published retrospective studies evaluating the use of DOACs for the treatment of cancer-associated thromboembolism. Patients in our study were at an increased risk for bleeding because of the inclusion of patients with interacting medications and renal or hepatic impairment, and as a result of the large proportion of patients with metastatic disease and GI cancers.
Although treatment failure occurred in only a small number of patients in our study, the presence of metastatic disease was associated with a higher incidence of treatment failure, as all patients with treatment failure had metastatic disease. In addition, compared with other types of cancer, a diagnosis of colorectal cancer was associated with an increased incidence of major bleeding.
A retrospective cohort study of a validated data set pooled from multiple US health systems demonstrated that patients with metastatic cancer were at an increased risk for bleeding versus those with nonmetastatic cancer.24 Furthermore, bleeding of the lower GI tract is a well-known presenting symptom of colorectal cancer and is frequently associated with erosion and hemorrhage of the primary tumor.25,26
In the HOKUSAI-VTE study, patients with GI cancer were more likely to have an increased risk for bleeding during treatment with a DOAC compared with an LMWH, and a majority of the bleeding associated with edoxaban in that clinical trial was GI bleeding.11 This increased risk for bleeding was noted for patients with esophageal and gastroesophageal cancers again in the SELECT-D clinical trial during the interim safety analysis, resulting in the subsequent exclusion of these patients from the study.10
Further clinical trials examining the use of DOACs for cancer-associated thromboembolism are ongoing. The CANVAS study is a randomized clinical trial in progress that will compare efficacy, safety, and patient satisfaction with therapy using 1 of 4 DOACs, including apixaban, dabigatran, edoxaban, and rivaroxaban, with LMWHs with or without a transition to warfarin.27 The recently completed but yet unpublished CASTA-DIVA study was designed to compare rivaroxaban with dalteparin for cancer-associated thromboembolism in patients with active cancer identified as high risk for recurrent VTE using the Ottawa score.28,29
Finally, the multinational, randomized CARAVAGGIO study aims to assess the noninferiority of apixaban versus dalteparin for the prevention of recurrent VTE in cancer-associated thromboembolism.30 The data from these clinical trials and additional real-world studies will provide further evidence regarding the use of DOACs for the treatment of cancer-associated thromboembolism.
Therapy for the treatment of cancer-associated thromboembolism should be selected using shared decision-making between patients and clinicians, and should weigh the benefits of DOACs, including the convenience of oral administration and lack of monitoring, against the risk for bleeding.31
Limitations
This study has several limitations. The largest limitation is the study’s retrospective nature, which limits data collection to visits captured in the EMR and is subject to the influence of confounding factors that might not have been assessed in the study, including adherence to therapy and concurrent anticancer treatment.
Furthermore, the data collection period was limited to 10 months, and additional outcomes might have occurred outside this time frame. Also, the outcomes of this study for patients receiving DOACs were not compared with a control group of patients using LMWHs.
In addition, only 1 patient with esophageal or gastroesophageal cancer was included. Previous studies have shown an increased bleeding risk associated with this cancer type, and our study may underestimate the incidence of major bleeding. However, colorectal cancer, which may have a bleeding risk similar to other GI or gastroesophageal malignancies because of the location of the primary tumor, was the most prevalent cancer included in this study.
Finally, only a small number of patients were included in this study, and future studies including more patients may provide more reliable estimates of treatment failure rates.
Conclusion
The results of this study suggest that outcomes of DOAC use for the treatment of cancer-associated thromboembolism in real-world practice are reflective of those seen in large randomized controlled trials.
Patients with colorectal cancer were more likely to have a bleeding event, and extra caution may be warranted in this patient population.
This study adds to the growing body of evidence suggesting that DOACs are an effective and safe anticoagulation option for patients with cancer-associated thromboembolism. Given the small sample size of this study, real-world data examining the appropriateness of these medications for the treatment of cancer-associated thromboembolism should continue to be assessed to validate their use in this patient population.
References
- Heit JA, Silverstein MD, Mohr DN, et al. Risk factors for deep vein thrombosis and pulmonary embolism: a population-based case-control study. Arch Intern Med. 2000;160:809-815.
- Lee AYY, Levine MN, Baker RI, et al; for the Randomized Comparison of Low-Molecular-Weight Heparin versus Oral Anticoagulant Therapy for the Prevention of Recurrent Venous Thromboembolism in Patients with Cancer (CLOT) investigators. Low-molecular-weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancer. N Engl J Med. 2003;349:146-153.
- King JB, Charlu M, Zhu S, Delate T. Adherence and persistence to direct oral anticoagulants for the treatment of cancer-associated venous thromboembolism. Circ Cardiovasc Qual Outcomes. 2019;12(suppl_1):Abstract 139.
- Theberge I, Bowdridge J, Forgie MA, et al. Rivaroxaban shows promise as effective therapy for cancer patients with venous thromboembolic disease. Thromb Res. 2017;152:4-6.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines): Cancer-Associated Venous Thromboembolic Disease. Version 1.2020. April 16, 2020. www.nccn.org/professionals/physician_gls/pdf/vte.pdf. Accessed September 4, 2020.
- Pignataro BS, Nishinari K, Cavalcante RN, et al. Oral rivaroxaban for the treatment of symptomatic venous thromboembolism in 400 patients with active cancer: a single-center experience. Clin Appl Thromb Hemost. 2017;23:883-887.
- Streiff MB, Milentijevic D, McCrae K, et al. Effectiveness and safety of anticoagulants for the treatment of venous thromboembolism in patients with cancer. Am J Hematol. 2018;93:664-671.
- Bott-Kitslaar DM, Saadiq RA, McBane RD, et al. Efficacy and safety of rivaroxaban in patients with venous thromboembolism and active malignancy: a single-center registry. Am J Med. 2016;129:615-619.
- Mantha S, Laube E, Miao Y, et al. Safe and effective use of rivaroxaban for treatment of cancer-associated venous thromboembolic disease: a prospective cohort study. J Thromb Thrombolysis. 2017;43:166-171.
- Young AM, Marshall A, Thirlwall J, et al. Comparison of an oral factor Xa inhibitor with low molecular weight heparin in patients with cancer with venous thromboembolism: results of a randomized trial (SELECT-D). J Clin Oncol. 2018;36:2017-2023.
- Raskob GE, van Es N, Verhamme P, et al; for the Hokusai VTE Cancer investigators. Edoxaban for the treatment of cancer-associated venous thromboembolism. N Engl J Med. 2018;378:615-624.
- McBane R II, Loprinzi CL, Ashrani A, et al. Apixaban and dalteparin in active malignancy associated venous thromboembolism. The ADAM VTE trial. Thromb Haemost. 2017;117:1952-1961.
- McBane RD II, Wysokinski WE, Le-Rademacher JG, et al. Apixaban and dalteparin in active malignancy-associated venous thromboembolism: the ADAM VTE trial. J Thromb Haemost. 2020;18:411-421.
- Mazzolai L, Aboyans V, Ageno W, et al. Diagnosis and management of acute deep vein thrombosis: a joint consensus document from the European Society of Cardiology working groups of aorta and peripheral vascular diseases and pulmonary circulation and right ventricular function. Eur Heart J. 2018;39:4208-4218. Erratum in: Eur Heart J. 2018;39:1316.
- Konstantinides SV, Meyer G, Becattini C, et al. 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS): the Task Force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology (ESC). Eur Heart J. 2020;41:543-603.
- Kearon C, Akl EA, Ornelas J, et al. Antithrombotic therapy for VTE disease: CHEST guideline and expert panel report. Chest. 2016;149:315-352. Erratum in: Chest. 2016;150:988.
- Key NS, Khorana AA, Kuderer NM, et al. Venous thromboembolism prophylaxis and treatment in patients with cancer: ASCO Clinical Practice Guideline update. J Clin Oncol. 2020;38:496-520.
- Schulman S, Kearon C; for the subcommittee on control of anticoagulation of the Scientific and Standardization committee of the International Society on Thrombosis and Haemostasis. Definition of major bleeding in clinical investigations of antihemostatic medicinal products in non-surgical patients. J Thromb Haemost. 2005;3:692-694.
- Eliquis (apixaban) tablets, for oral use [prescribing information]. Princeton, NJ: Bristol-Myers Squibb Company; New York, NY: Pfizer; November 2019.
- Savaysa (edoxaban) tablets, for oral use [prescribing information]. Basking Ridge, NJ: Daiichi Sankyo; April 2020.
- Xarelto (rivaroxaban) tablets, for oral use [prescribing information]. Titusville, NJ: Janssen Pharmaceuticals; March 2020.
- Mahé I, Elalamy I, Gerotziafas GT, Girard P. Treatment of cancer-associated thrombosis: beyond HOKUSAI. TH Open. 2019;3:e309-e315.
- Ramacciotti E, Resende Aguiar VC, Castelli Júnior V, et al. Edoxaban for venous thromboembolism treatment—the new kid on the block for Latin America. A practical guide. Clin Appl Thromb Hemost. 2018;24(9 suppl):340S-349S.
- Angelini DE, Radivoyevitch T, McCrae KR, Khorana AA. Bleeding incidence and risk factors among cancer patients treated with anticoagulation. Am J Hematol. 2019;94:780-785.
- Viborg S, Søgaard KK, Farkas DK, et al. Lower gastrointestinal bleeding and risk of gastrointestinal cancer. Clin Transl Gastroenterol. 2016;7:e162.
- Shen H, Ye XY, Li XF, et al. Severe esophageal bleeding in colorectal cancer due to antitumor therapy: a case report. Oncol Lett. 2015;10:3660-3662.
- ClinicalTrials.gov. Direct oral anticoagulants (DOACs) versus LMWH +/- warfarin for VTE in cancer (CANVAS). https://clinicaltrials.gov/ct2/show/NCT02744092. Accessed October 4, 2018.
- ClinicalTrials.gov. Cancer associated thrombosis, a pilot treatment study using rivaroxaban (CASTA-DIVA). https://clinicaltrials.gov/ct2/show/NCT02746185. Accessed October 4, 2018.
- Louzada ML, Carrier M, Lazo-Langner A, et al. Development of a clinical prediction rule for risk stratification of recurrent venous thromboembolism in patients with cancer-associated venous thromboembolism. Circulation. 2012;126:448-454.
- Agnelli G, Becattini C, Meyer G, et al. Apixaban for the treatment of venous thromboembolism in patients with cancer. N Engl J Med. 2020;382:1599-1607.
- Khorana AA, Noble S, Lee AYY, et al. Role of direct oral anticoagulants in the treatment of cancer-associated venous thromboembolism: guidance from the SSC of the ISTH. J Thromb Haemost. 2018;16:1891-1894.