Neutrophils are critical in providing defense against bacterial and fungal infections.1 Patients diagnosed with cancer are especially at risk for infection when their absolute neutrophil count (ANC) decreases dramatically after receiving cytotoxic chemotherapy. A fever may be the only signal of a potentially life-threatening infection, which requires immediate empiric broad-spectrum antimicrobial therapy.1 Expert guidelines provide succinct antimicrobial schemes for patients with cancer who have neutropenia or sepsis; however, the guidelines’ guidance is limited in the setting of suspected multidrug-resistant (MDR) pathogens.1-4
The aim of this review is to support decision-making for appropriate antimicrobial selection and the course of treatment for neutropenia, with concern for potential MDR organisms. MDR organisms are defined by the Centers for Disease Control and Prevention (CDC) as “microorganisms, predominately bacteria, that are resistant to one or more classes of antimicrobial agents.”5
Neutropenia is defined by the National Comprehensive Cancer Network as an ANC of <500 neutrophils/mcL, or an ANC of <1000 neutrophils/mcL with a predicted decrease to ≤500 neutrophils/mcL over the next 48 hours.3 The expert panel of the treatment guidelines from the American Society of Clinical Oncology and the Infectious Diseases Society of America defined neutropenia as an ANC of <1000 neutrophils/mcL.1 Fever in patients with neutropenia is defined by all expert panels as a single oral temperature of ≥101°F (38.3°C), or a temperature of ≥100.4°F (38°C) for at least an hour.1-3
The risk for infection can worsen with a longer duration of neutropenia. Prolonged neutropenia is defined as an expected duration of >7 days.2 Profound neutropenia is a dramatic decrease in cell counts, in which the ANC is ≤100 neutrophils/mcL after receiving cytotoxic chemotherapy.2 Functional neutropenia “refers to patients whose hematologic malignancy results in qualitative defects (impaired phagocytosis and killing of pathogens) of circulating neutrophils.”2 Despite having a normal neutrophil count, patients with functional neutropenia should be considered to have an increased risk for infection.2
Febrile neutropenia is a medical emergency associated with significant morbidity and mortality that has a large financial burden on patients and on institutions.6 In patients with neutropenia who have a fever, approximately 40% to 50% have an infectious etiology and 10% to 30% have bacteremia.7
The risk for a bacterial infection is related to the severity and duration of neutropenia, and most episodes of bacteremia occur during prolonged or profound neutropenia.1 The mortality rate of critically ill patients with cancer who have neutropenia is up to 11%, and can be as high as 50% in patients with severe sepsis or septic shock.1,8
In patients with solid-tumor malignancies, 10% to 50% will have neutropenic fever in the course of their treatment compared with more than 80% of patients with hematologic malignancies.2
The incidence of MDR organisms as the causative pathogens for bacterial infections has been increasingly reported in patients with cancer.9 In a 5-year epidemiologic retrospective meta-analysis, 73 patients with cancer were infected with MDR organisms, including MDR Klebsiella pneumoniae (37%), oxacillin (or methicillin)-resistant Staphylococcus aureus (MRSA; 24%), MDR Acinetobacter baumannii (21%), MDR Pseudomonas aeruginosa (5%), MDR Escherichia coli (4%), and vancomycin-resistant Enterococcus faecium (3%). In total, 6% of the patients were infected with >2 MDR pathogens.9
Fever was recorded in 51% of the study patients, and neutropenia was present in 14%. Empiric antibiotic therapy was initiated in 69% of the patients, but antibiotics were effective against the causative MDR pathogens in only 13% of the patients. A mortality rate of 32% was observed, of which 30% of the deaths were attributed to infection.9
The results of this study by Perdikouri and colleagues illustrate the challenges of using guideline algorithms for empiric therapy in patients for whom MDR infections may be of concern.9
Patients at Risk for Infection
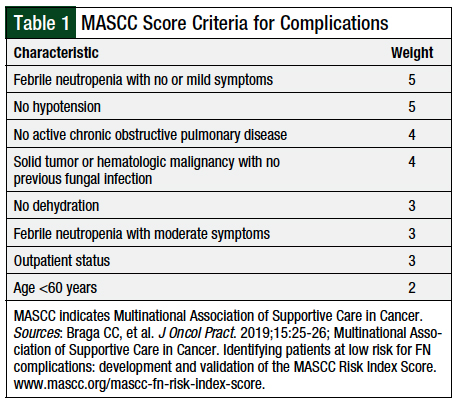
Stratifying patients based on the risk for complications related to febrile neutropenia can help guide providers in choosing whether the risk necessitates inpatient admission or if a treatment can be directed in an outpatient setting.10 Other considerations include the appropriateness of antimicrobial therapy selection, the route of administration, and the duration of therapy. The risk for adverse events can be classified using the validated Multinational Association of Supportive Care in Cancer Risk Index scoring system.10 This classification considers independent predictive factors at fever onset in adults with febrile neutropenia and cancer who are receiving chemotherapy.6,10
The weighted risk factors for adverse events in this patient population are shown in Table 1. The maximum theoretical score is 26; a score of less than 21 indicates a high risk for poor outcomes and a score of 21 or higher indicates a low risk.6,10,11
Patients at high risk for adverse events are anticipated to have prolonged and profound neutropenia; or have comorbid conditions, such as uncontrolled cancer, chronic obstructive pulmonary disease, poor functional status, or advanced age; or present as clinically unstable, with hypotension, pneumonia, new-onset abdominal pain, or neurologic changes.2 Patients who meet the high-risk criteria will likely be admitted to the hospital and receive intravenous (IV) empirical antibiotic therapy.2
Low-risk patients are categorized as having an anticipated duration of neutropenia of ≤7 days, have few or no comorbidities, and remain clinically stable with adequate hepatic and renal functions.2 Such patients are likely to be candidates for oral empirical therapy, which may be administered at an outpatient setting.2
The risk factors for resistant bacterial infections include the use of broad-spectrum antimicrobials, prolonged and/or repetitive hospitalizations, intensive care unit admissions, infections acquired during hospital admission, presence of indwelling devices such as urinary catheters, high severity of illness, and older age.12 Patients should be classified as high-risk if they have previously had colonization with an organism, have a new infection, or have concern for infection with an MDR organism.1
On presentation, certain laboratory parameters should be obtained, including a complete blood count with a differential, a basic metabolic panel to assess electrolytes, serum creatinine, blood urea nitrogen, and liver function tests to evaluate hepatic transaminases and total bilirubin.2 Two sets of blood cultures are recommended, 1 from each lumen of a central line preferred (if present), and, whenever possible, all cultures should be obtained before initiating antimicrobial therapy. Specimens from other potential sites with localizing signs or symptoms of infection should be drawn, and a chest x-ray is indicated for patients with any evidence of respiratory distress.2
During influenza seasons, testing for respiratory viruses based on clinical symptoms should be considered. Fever can be an important indicator of infection, because other prominent signs and symptoms of inflammation on a physical examination are often attenuated or absent in patients with neutropenia.2
Antimicrobial Course of Therapy
In a vulnerable immunocompromised patient population, urgent evaluation and access to appropriate diagnostic tools are imperative to prevent major adverse events from febrile neutropenia.1 Empiric therapy is initiated at the time of concern for possible infection to help prevent morbidity and mortality associated with bacterial pathogens.
If a patient presents to the clinic or emergency department with concerns of febrile neutropenia, empiric antimicrobial therapy should be initiated within 1 hour of triage.1 Once blood culture results have been obtained, more precise antibiotic choices can be made to target the pathogens of concern. Regardless of whether the cultures remain negative, empiric antibiotics should continue to cover possible occult infections in patients with febrile neutropenia.1
Gram-positive organisms may be more frequently isolated than gram-negative organisms; however, because of the association between gram-negative organisms and increased mortality, a broad array of coverage should be initiated.2,13,14 P aeruginosa has especially high mortality rates and remains an essential target of initial empiric antibiotic therapy.2
As resistance patterns change with the use of broad-spectrum antimicrobials, site-specific antibiograms and susceptibility patterns are important to assess when determining the appropriate diagnosis and treatment plan. For example, if an institution has a high prevalence of extended-spectrum beta-lactamase–producing gram-negative bacilli and a patient is presenting with sepsis, empiric antimicrobial therapy with a carbapenem may be considered to ensure coverage for potential MDR organisms.7
Initial Antibiotics for High-Risk Patients
An antipseudomonal beta-lactam agent that also covers other serious gram-negative pathogens can be used as monotherapy for high-risk patients who require hospitalization and IV empiric therapy.2 The agents of choice include cefepime, piperacillin plus tazobactam and carbapenems, such as meropenem or imipenem plus cilastatin.2
Of importance, the coverage of aerobic gram-positive cocci with agents such as vancomycin is not recommended as the standard initial antibiotic therapy.1 Vancomycin may be added in situations where a patient is hemodynamically unstable or septic, has radiographic evidence of pneumonia, has positive blood culture for gram-positive bacteria, has known or suspected MRSA, has a catheter-related infection, has a skin or soft-tissue infection, or has severe mucositis while receiving fluoroquinolone prophylaxis.1
Considerations for the use of other antimicrobials, such as aminoglycosides or fluoroquinolones, depend on adverse-event concerns, including hypotension and pneumonia, or if there is potential for antimicrobial resistance as guided by local antibiograms. It is important to consider the intra-hospital variability that may exist in pathogen susceptibility, and to reference the most appropriate unit-specific or hospitalwide antibiogram the institution has organized.
In addition, if a patient has had previous colonization with an MDR organism, the risk for future resistant pathogens remains high.15 The most pragmatic approach would initially be to cover any previous resistant strains empirically and de-escalate treatment as appropriate if no MDR pathogens are isolated.15
Initial Antibiotics for Low-Risk Patients
For low-risk patients, the initial empiric antibiotics can be oral or IV, depending on the treatment setting, and patients may be transitioned to an outpatient regimen once they are clinically stable.1 Oral options include a combination of ciprofloxacin and amoxicillin plus clavulanate, or ciprofloxacin and clindamycin. Monotherapy options include a fluoroquinolone targeting Pseudomonas, such as ciprofloxacin or levofloxacin.1 Of note, if a patient received prophylactic treatment with a fluoroquinolone, these agents should be avoided, because of concerns about possible resistance.
If low-risk patients have any new signs or symptoms that are indicative of an infection, immediate reevaluation should be completed, which may require hospital readmission or a prolonged hospital stay to be treated as a high-risk patient.1
No single empirical therapeutic regimen is superior to others for the initial treatment of patients with febrile neutropenia. For high-risk patients, monotherapy with an antipseudomonal beta-lactam is as effective as multidrug combinations and is recommended as first-line therapy.2 However, ceftazidime may not be a reliable agent, because of its “decreasing potency against gram-negative organisms and its poor activity against many gram-positive pathogens, such as streptococci.”2 Aminoglycosides are not used as monotherapy for empiric coverage during neutropenia, because of concerns about microbial resistance.2
In patients with a noted hypersensitivity reaction to beta-lactams, treatment with aztreonam has resulted in successful clinical outcomes in a single-center, retrospective study of 106 patients with neutropenia.16 Of the 27 patients who received aztreonam as monotherapy, the survival rate was 89% on resolution of febrile neutropenia or at the completion of the treatment course.16 However, because of its narrow spectrum of coverage and inferior susceptibility patterns compared with other beta-lactams, aztreonam should be reserved as a last-line agent and should be used in combination with another antimicrobial to ensure appropriate coverage.
Modifying Antibiotics During Treatment
If a low-risk patient who is afebrile after the initial fever presents with new symptoms suggestive of an infection, the treatment plan should be adjusted to that of a high-risk patient.1 In these low-risk patients and in high-risk patients, additions to the initial regimen can be made to manage additional adverse events, such as suspected catheter-related infections, skin and soft-tissue infections, pneumonia, or hemodynamic instability, if necessitated. Clinical and microbiologic findings should ultimately guide the modifications to the standard regimen plan.
Broadening coverage to include additional or resistant gram-negative, gram-positive, and anaerobic bacteria or fungi can be considered if patients remain hemodynamically unstable with their standard regimen.2 Typically, vancomycin or other agents that are active against aerobic gram-positive cocci are not recommended for the initial management of fever or febrile neutropenia, unless there is suspicion for other underlying infections. If initiated and there is no evidence of a gram-positive infection, these agents may be stopped after 48 hours. If all cultures are negative and a patient’s fever has resolved, it is appropriate to consider discontinuing IV antibiotics 72 hours after the patient’s last fever and to reinitiate prophylaxis, if applicable, regardless of their ANC level.2
An empiric duration of 72 hours is supported by an open-label, randomized, controlled phase 4 clinical trial that assessed the duration of empiric therapy in patients with febrile neutropenia and hematologic malignancies.17 In the experimental group (N = 78), empiric therapy was withdrawn after at least 72 hours of clinical stability and defervescence. The control group (N = 79) continued treatment until their ANC recovery was >500 neutrophils/mcL. The primary end point of days free of empiric antimicrobial therapy was 16.1 days in the experimental group (standard deviation [SD], 6.3) versus 13.6 days in the control group (SD, 7.2; absolute difference −2.4; 95% confidence interval [CI], −4.6 to −0.3; P = .026). There were fewer serious adverse events identified with the shorter course of antibiotics (18 events in the experimental group vs 38 events in the control group).17
This study illustrates that in patients with high-risk febrile neutropenia, antimicrobials can be stopped, regardless of ANC count, if a patient has negative blood cultures, remains clinically stable, and is afebrile for 72 hours.17
In addition, European guideline recommendations for empirical antibacterial therapy for patients with febrile neutropenia suggest the discontinuation of antibiotics after 72 hours, regardless of neutrophil count and the anticipated duration of neutropenia.12 This recommendation helps streamline and minimize unnecessary antimicrobial use and decreases the incidence of subsequent adverse events and the potential for treatment resistance.
Patients who are clinically stable but still have fevers after several days of broad-spectrum therapy do not necessitate broadening therapy. Without an identifiable source, fever alone is not an indication to add to or change the antimicrobial regimen.2 A physical examination and review of clinical symptoms should be completed to exclude additional reasons for persistent fevers in patients with neutropenia, with additional radiographic or infectious disease workup as indicated.
In clinical situations where blood cultures are positive but patients begin to improve clinically, their antimicrobial regimen can be simplified, such as de-escalation from IV to oral antibiotics, while maintaining appropriate antimicrobial coverage. Once a bacterial pathogen is identified and susceptibilities return, further de-escalation of antibiotics to a more targeted therapy can be considered when the patient is clinically stable.
Beta-Lactam Allergies
Most patients with noted penicillin allergies who do not have a history of an immediate-type hypersensitivity reaction can tolerate treatment with cephalosporins.2 Those with more severe reactions, such as hives or bronchospasm, should potentially avoid treatment with beta-lactams, because of the possibility for cross-reactivity. Instead, these patients could receive a combination therapy, such as ciprofloxacin plus clindamycin, or aztreonam plus vancomycin, that is guided by local antibiograms.2
Two recent systematic reviews about the risk for cross-reactivity related to cephalosporins and carbapenems in patients with confirmed immunoglobulin E–mediated or T-cell–mediated penicillin allergies showed variations based on side-chain profiles.18 Nearly 1300 patients who were allergic to penicillin were included, and their reactions to cephalosporins with side chains that were identical, intermediate similar, and low similar were 16.5%, 5.6%, and 2.1%, respectively.18
There was a much lower prevalence of carbapenem cross-reactivity, with a risk of 0.87%. Even in immunoglobulin E–mediated and severe anaphylactoid reactions to penicillin, treatment with carbapenems resulted in a very low occurrence of cross-reactivity.18 With a long history of carbapenem’s safety in the setting of penicillin allergies, carbapenems may potentially be used in patients with penicillin allergies.
Resistant Organisms
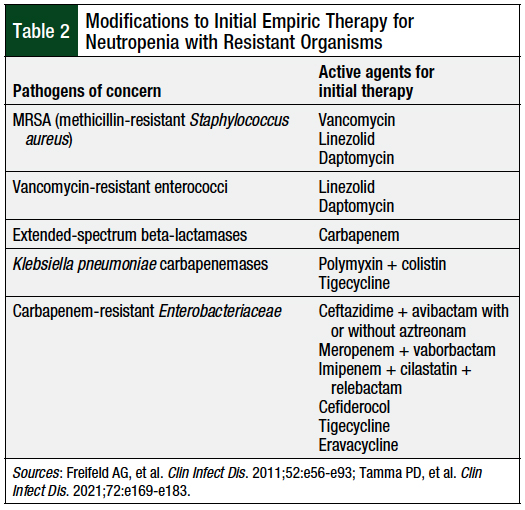
The increasing incidence of antibiotic-resistant pathogens has become a significant challenge in the treatment of patients with neutropenia. For concerns regarding resistant organisms, including MRSA, vancomycin-resistant enterococci, extended-spectrum beta-lactamase–producing gram-negative bacilli, and carbapenemase-producing organisms, including K pneumoniae carbapenemase (KPC), modifications to the initial empiric therapy can be made (Table 2).2,19
The addition of these agents should be considered if the patient is unstable, has positive blood cultures for resistant bacteria, has risk factors of a previous infection or colonization with resistant organism(s), or has received treatment in an institution with high rates of endemicity.2 The ultimate selection of an empiric regimen should be based on the risk status, localizing signs and symptoms of infection, as well as local and individual patterns of bacterial colonization and resistance.2
The rates of resistant gram-negative bacteria have been globally increasing, particularly with the detection of carbapenem-resistant Enterobacteriaceae (CRE) infections.20 Carbapenemases can be divided into the 3 molecular classes of class A carbapenemases, which include KPCs; class B metallo-beta-lactamases (MBLs), such as imipenemase, Verona Integron–encoded MBL, and New Delhi MBL; and class D enzymes, such as oxacillin carbapenemase number 48 (OXA-48).20
Classes A and D have active sites with serine atoms that are inhibited by beta-lactam inhibitors, such as clavulanic acid and tazobactam.20 Class B MBLs are zinc-dependent hydrolases that inactivate nearly all beta-lactam antibiotics and are the most clinically relevant. These emerging enzymes are of concern on an international level, because transmission-resistant clones are beginning to disseminate, but therapeutic options for the treatment of these infections are very limited.20
The morbidity and mortality associated with CRE infections also continue to rise internationally.21,22 In one nationwide retrospective survey from Italy, the epidemiologic prevalence of carbapenem-resistant K pneumoniae in autologous and allogeneic stem-cell transplant recipients increased by nearly 6-fold from 2010 to 2013.21 Colonization with carbapenem-resistant K pneumoniae resulted in 25.8% of patients who had an autologous stem-cell transplant and 39.2% of patients who had an allogeneic stem-cell transplant having an infection, with associated mortality rates of 16% and 64.4%, respectively. Of note, most patients who died had severe neutropenia and/or acute (grade II-IV) or chronic extensive graft-versus-host disease at the time of the infection.21
Another retrospective observational study of patients with hematologic cancer and febrile neutropenia evaluated the incidence of bloodstream infections with resistant pathogens.22 Carbapenem-resistant gram-negative bacteria was identified as the cause of 12% of gram-negative bacteremia and of 9% of all of the bacteremia that were assessed. The gram-negative pathogens of concern were A baumannii, P aeruginosa, and Serratia marcescens, which were associated with approximately 4.6% of the deaths from bloodstream infections.22
Interestingly, in a prospective, multicenter, cohort study, the CDC evaluated the positive clinical cultures of 1040 patients with CRE isolates.23 The identification of CRE was defined by the CDC in 3 groups: 59% carbapenemase-producing Enterobacterales, 19% non–carbapenemase-producing Enterobacterales, and 22% unconfirmed CRE that were initially reported as CRE and were later susceptible to carbapenems. The most common isolate was KPC-producing clonal group 258. The primary outcome in this study was the desirability of outcome ranking, which was not statistically significant in any group.23
This study illustrates that regardless of the mechanism of resistance, the CDC definition for CRE is broad and accounts for a diverse group of bacteremia that may not respond appropriately to therapies directed at carbapenemase-producing Enterobacterales.
New and Promising Antimicrobials
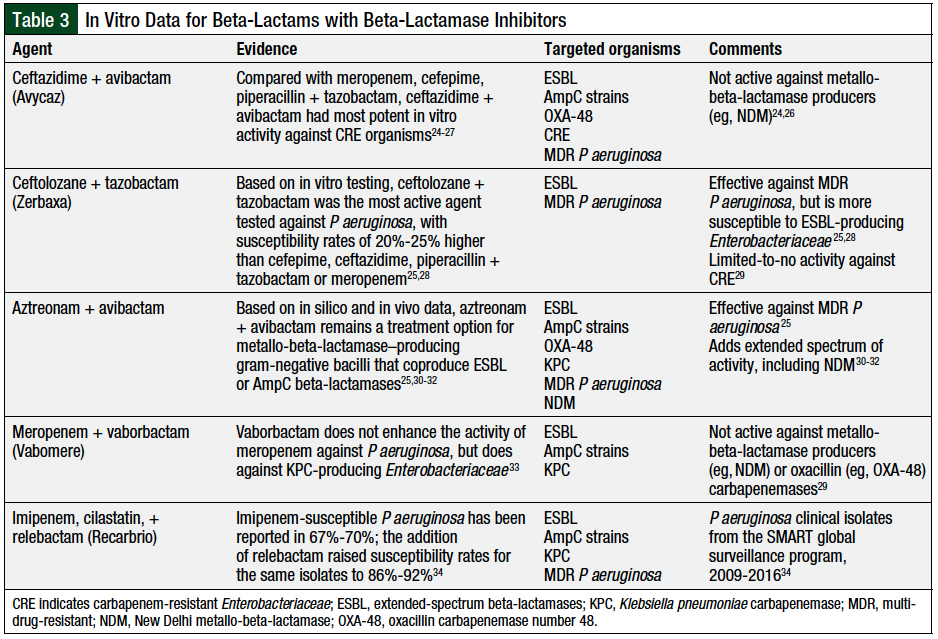
The current guidelines for empiric therapy for febrile neutropenia may not appropriately cover MDR gram-negative bacteria. Resistance could occur through multiple mechanisms, including the production of beta-lactamases, changes to porins that allow the passage of beta-lactams through the bacterial outer membrane, and efflux pumps that remove beta-lactams.24 To circumvent this resistance, new beta-lactams (and non–beta-lactams) combined with beta-lactamase inhibitors (BLBLIs) have been developed (Table 3).24-34
Combination treatments, such as ceftazidime plus avibactam, and ceftolozane plus tazobactam, may have a place in therapy after nonresponse to the currently recommended antimicrobials (cefepime, piperacillin plus tazobactam, carbapenems) and/or with concern for MDR organisms.25 However, the use of combination treatments is limited because of their high-cost burden, lack of clinical data in patients with neutropenia, and inherent resistance to treatment.25
One study’s preliminary data report suggested that ceftazidime plus avibactam may have a role as empiric therapy in patients with hematologic cancer and febrile neutropenia who had carbapenem-resistant K pneumoniae bloodstream infections.26 A total of 8 (57%) patients received empiric ceftazidime plus avibactam treatment during an episode of febrile neutropenia. All the carbapenem-resistant K pneumoniae isolates that were colonized were KPC producers and were resistant to colistin (minimum inhibitory concentrations [MICs] >64 ug/mL), whereas 5 carbapenem-resistant K pneumoniae isolates were resistant to gentamicin (MIC >16 ug/mL) and tigecycline (MIC >8 ug/mL). Monotherapy was dosed at 2.5 g every 8 hours in 6 patients, and 2 patients received combination therapy with the addition of tigecycline and gentamycin. The mean duration of treatment was 13.6 days, and all patients were alive at 14 days of evaluation.26
Beyond small case series and reports, these combination agents are not frequently used empirically in patients with febrile neutropenia. However, in vitro data on BLBLIs have shown the lowest level of resistance and most potent activity against many gram-negative isolates compared with standard-of-care antimicrobial agents.25,26
One study assessed 521 clinical isolates from patients with cancer, the majority (>90%) of which were bloodstream infections, for susceptibility to ceftazidime plus avibactam.27 Of the 51 MDR P aeruginosa isolates, 42 (82.4%) were susceptible to ceftazidime plus avibactam. In comparison, only 21.6% of these isolates were susceptible to meropenem, 35.3% were susceptible to piperacillin plus tazobactam, and 37.3% were susceptible to cefepime.27
In another study, a total of 1257 P aeruginosa isolates were examined, of which 61% were isolated from nonrespiratory sources (ie, blood, wounds, or body fluids).28 Susceptibility to ceftolozane plus tazobactam was >90% for all isolates and was considered overall to be the most active agent compared with guideline-recommended treatments.28 The in vitro data cited here suggest that these treatment combinations warrant further evaluation in the empiric treatment of patients with febrile neutropenia.
To manage febrile neutropenia in patients with hematologic malignancies, the Spanish Society of Infectious Diseases and Clinical Microbiology and the Spanish Association of Hematology and Hemotherapy have compiled a consensus document advising on the role of BLBLIs.35 For extensively drug-resistant or pan–drug-resistant P aeruginosa infections and drug-resistant gram-negative pathogens, such as CRE, the use of ceftolozane plus tazobactam (recommendation C-II) or ceftazidime plus avibactam (recommendation C-I) may be considered.35
A retrospective study evaluated patients with hematologic cancer and neutropenia who had at least 1 episode of a bloodstream infection because of an extended-spectrum beta-lactamase–producing gram-negative bacilli.36 Patients had received carbapenems or BLBLIs for more than 24 hours as empirical (N = 174) or definitive (N = 251) antibiotic therapy. The primary outcome assessed 30-day mortality, and there was no difference between carbapenems and BLBLIs in the empirical or definitive therapy groups (13.4% vs 20.8%; P = .33; and 15.8% vs 5.8%; P = .99, respectively). However, because of the study’s small sample size and retrospective design, the data were not powered enough to detect a true difference in mortality between the groups.36
In the setting of carbapenem-sparing alternative therapies, BLBLIs have similar efficacy in the treatment of severely immunosuppressed patients with hematologic cancer, neutropenia, and bloodstream infections resulting from extended-spectrum beta-lactamase producing gram-negative bacilli.29 These strategies may also be used in the context of mild-to-moderate bloodstream infections from extended-spectrum beta-lactamases or sites where source control may be rapidly obtained to minimize the spread of CRE.29
However, there is very limited evidence on the use of these alternative antibacterial agents in this setting.29 To help guide clinical practice with these combination treatments, studies comparing these antimicrobials with guideline-recommended therapies would help direct clinical practice while considering patient characteristics and local resistance patterns.
The combination of aztreonam and avibactam has adequate in vitro activity against New Delhi MBL, even though the rate of hydrolysis of this enzyme is considered slow.30,31 The rationale postulated is that avibactam inactivates classes A, C, and D beta-lactamases, which restores the susceptibility of aztreonam.30 Potential combinations of ceftazidime and avibactam with aztreonam have had synergistic effects in 2 case reports, reducing MICs from >256 mg/L to between 0.125 mg/L and 2 mg/L. At the time the article by Davido and colleagues was published, aztreonam plus avibactam was in early development; however, their results show that this combination may be effective in patients with MBL infections.30
Most recently, the susceptibility of aztreonam plus avibactam was evaluated in 161 MBL-Enterobacteriaceae isolates, including K pneumoniae (45.4%) and E coli (32.9%).32 Susceptibility testing to aztreonam showed resistance to 81.4% of isolates. However, with the addition of avibactam to aztreonam, 96.9% of isolates were susceptible, with a MIC90 of ≤1 μg/mL. This study indicates the high potency of the combination of aztreonam and avibactam and the rationale for not using aztreonam as monotherapy because of its rapid inactivation by beta-lactamases.32
Another promising combination, meropenem plus vaborbactam, has been effective against KPC-producing Enterobacteriaceae.33 Although this combination treatment was tested against 4500 gram-negative isolates and resulted in the inhibition of 131 (98.5%) of 133 KPC-producing Enterobacteriaceae strains, the combination did not show any benefit against meropenem-resistant A baumannii or P aeruginosa, potentially as a result of differing mechanisms of carbapenem resistance in the study region.33
A recent novel beta-lactamase inhibitor, relebactam (in combination with imipenem and cilastatin), has shown activity against class C cephalosporinases, such as AmpC beta-lactamases, and class A carbapenemases, including KPC.37 In vitro studies have shown significant reductions in MICs when relebactam was added to imipenem in nonsusceptible strains of Enterobacteriaceae and in P aeruginosa.34 Clinical isolates of P aeruginosa were tested against imipenem, with the rates of susceptibility ranging from approximately 67% to 70%. When 4 μg/mL of relebactam was added, the susceptibility rates of imipenem increased to approximately between 86% and 92%.34
In a separate susceptibility report, imipenem plus relebactam increased susceptibility by 3-fold to carbapenem-resistant P aeruginosa isolates that do not express MBLs.38 This confirms the effectiveness and potency of this unique antimicrobial combination and how it could have a place in therapy for patients with neutropenia who have carbapenem-resistant P aeruginosa infections.
Based on these in vitro data, we would expect that imipenem plus relebactam would be effective against pathogens nonsusceptible to carbapenems. In the double-blind, randomized controlled phase 3 trial, RESTORE-IMI 1, imipenem plus relebactam showed an overall favorable response compared with colistin plus imipenem in nonsusceptible imipenem pathogens.39 The beta-lactamases that were identified in the study included AmpC (84%), extended-spectrum beta-lactamase (35%), KPC (16%), and OXA-48 (3%). The primary outcome was similar between the imipenem plus relebactam and colistin plus imipenem treatment arms (71% vs 70%, respectively; 90% CI, –27.5-21.4), which indicates the effectiveness of imipenem plus relebactam in overcoming resistance, particularly in extended-spectrum beta-lactamase and KPC producers. However, because of the small sample size of patients with CRE, further in vivo evidence is warranted.39
Novel agents such as eravacycline, a fluorocycline, and cefiderocol, a siderophore cephalosporin, were compared with ceftazidime plus avibactam in 343 carbapenem-resistant E coli isolates.40 The overall susceptibilities for each agent were 98% for eravacycline, 92% for cefiderocol, and 82% for ceftazidime plus avibactam. The addition of avibactam increased ceftazidime’s susceptibility by 71%, from 11% to 82%.40 These observed patterns of susceptibility show the potential for the global use of these agents in the treatment of carbapenem-resistant E coli strains.
Recently, in an open-label, randomized phase 3 study, CREDIBLE-CR, treatment with cefiderocol was compared with best-available therapy in 152 patients with carbapenem-resistant gram-negative pathogens.41 The resistant organisms included A baumannii (46%), K pneumoniae (33%), and P aeruginosa (19%). In patients with bloodstream infections or sepsis, clinical and microbiologic cure was equal in both treatment arms (43%), which indicates cefiderocol’s strong activity and potential for being a novel option for patients with resistant pathogens.41
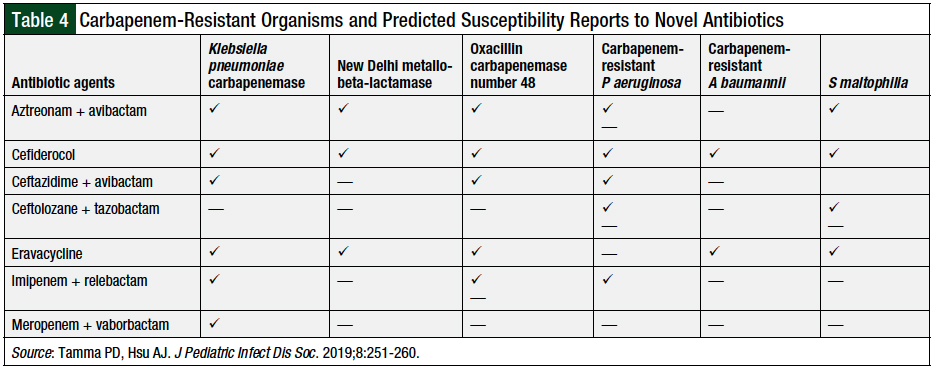
Table 4 illustrates the potential susceptibility of the novel antibiotics discussed in this review against carbapenem-resistant pathogens.42
Prophylaxis Options
It is important to consider supportive care measures beyond antimicrobials, such as appropriate respiratory care and hand hygiene, as well as vaccine administration. For high-risk patients with a prolonged or profound duration of neutropenia, prophylaxis with a fluoroquinolone may be initiated.2 Fluoroquinolones have demonstrated lower rates of bacteremia and a lower incidence of neutropenic fever.43
The fluoroquinolone agents that have been the most comprehensively evaluated are levofloxacin and ciprofloxacin. Although levofloxacin and ciprofloxacin have similar efficacy, levofloxacin may be preferred in situations with a heightened risk for viridans group streptococcal infections related to oral mucositis.2 No adjunct gram-positive agents are recommended.2
Levofloxacin 500 mg orally daily is the preferred prophylactic regimen for febrile neutropenia; however, if a patient is unable to tolerate oral medications, 500 mg IV daily can be substituted.3 In patients who have an allergy, intolerance, or contraindication to fluoroquinolones, cefpodoxime 200 mg twice daily can be a viable substitute.43 These agents were compared in a single-center, retrospective chart review in allogeneic stem-cell transplant recipients.43 Both agents had similar rates of neutropenic fever and antimicrobial nonresponse and comparable rates of infections, hospitalizations, and mortality in the first 100 days of treatment.43
Conclusion
Antibiotic resistance in patients with febrile neutropenia is a growing concern where modification to initial empiric therapy needs to be considered early in the course of treatment. Increasing rates of resistance with standard therapies have been acknowledged internationally, with efforts to define best practices, such as appropriate de-escalation and duration of therapy, to help minimize the risk for further treatment resistance. In cases where treatment resistance has become more predominant and therapeutic options are limited, in vitro data may help guide healthcare providers in determining appropriate empiric strategies to combat resistant organisms.
Based on a patient’s clinical status, previous culture data, institutional antibiograms, and the prevalence of MDR organisms, new and promising antimicrobials may be more widely used as empiric therapies in the coming years.
Author Disclosure Statement
Dr Bubalo has received research support from Helsinn. Dr Kedzior and Dr Ham have no conflicts of interest to report.
References
- Taplitz RA, Kennedy EB, Bow EJ, et al. Outpatient management of fever and neutropenia in adults treated for malignancy: American Society of Clinical Oncology and Infectious Diseases Society of America Clinical Practice Guideline update. J Clin Oncol. 2018;36:1443-1453.
- Freifeld AG, Bow EJ, Sepkowitz KA, et al. Clinical practice guideline for the use of antimicrobial agents in neutropenic patients with cancer: 2010 update by the Infectious Diseases Society of America. Clin Infect Dis. 2011;52:e56-e93.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines): Prevention and Treatment of Cancer-Related Infections. Version 2.2020. June 5, 2020. www.nccn.org/professionals/physician_gls/pdf/infections.pdf. Accessed April 19, 2020.
- Rhodes A, Evans LE, Alhazzani W, et al. Surviving Sepsis Campaign: international guidelines for management of sepsis and septic shock: 2016. Crit Care Med. 2017;45:486-552.
- Siegel JD, Rhinehart E, Jackson M, et al; for the Centers for Disease Control and Prevention. Management of multidrug-resistant organisms in healthcare settings, 2006. Updated February 15, 2017. www.cdc.gov/infectioncontrol/pdf/guidelines/mdro-guidelines.pdf. Accessed April 20, 2020.
- Braga CC, Taplitz RA, Flowers CR. Clinical implications of febrile neutropenia guidelines in the cancer patient population. Crit Care Med. 2019;15:25-26.
- Zimmer AJ, Freifeld AG. Optimal management of neutropenic fever in patients with cancer. Crit Care Med. 2019;15:19-24.
- Legrand M, Max A, Peigne V, et al. Survival in neutropenic patients with severe sepsis or septic shock. Crit Care Med. 2012;40:43-49.
- Perdikouri EIA, Arvaniti K, Lathyris D, et al. Infections due to multidrug-resistant bacteria in oncological patients: insights from a five-year epidemiological and clinical analysis. Microorganisms. 2019;7:277.
- Multinational Association of Supportive Care in Cancer. Identifying patients at low risk for FN complications: development and validation of the MASCC Risk Index Score. www.mascc.org/mascc-fn-risk-index-score. Accessed April 20, 2020.
- Goodman LM, Estfan B, Montero A, et al. Improving the management of patients with low-risk neutropenic fever at the Cleveland Clinic Taussig Cancer Institute. Crit Care Med. 2017;13:e259-e265.
- Averbuch D, Orasch C, Cordonnier C, et al; for ECIL4, a joint venture of EBMT, EORTC, ICHS, ESGICH/ESCMID and ELN. European guidelines for empirical antibacterial therapy for febrile neutropenic patients in the era of growing resistance: summary of the 2011 4th European Conference on Infections in Leukemia. Haematologica. 2013;98:1826-1835. Erratum in: Haematologica. 2014;99:400.
- Zhang Y, Zheng Y, Dong F, et al. Epidemiology of febrile neutropenia episodes with gram-negative bacteria infection in patients who have undergone chemotherapy for hematologic malignancies: a retrospective study of 10 years’ data from a single center. Infect Drug Resist. 2020;13:903-910.
- Kara Ali R, Surme S, Balkan II, et al. An eleven-year cohort of bloodstream infections in 552 febrile neutropenic patients: resistance profiles of Gram-negative bacteria as a predictor of mortality. Ann Hematol. 2020;99:1925-1932.
- Gustinetti G, Mikulska M. Bloodstream infections in neutropenic cancer patients: a practical update. Virulence. 2016;7:280-297.
- McCullough BJ, Wiggins LE, Richards A, et al. Aztreonam for febrile neutropenia in patients with beta-lactam allergy. Transpl Infect Dis. 2014;16:145-152.
- Aguilar-Guisado M, Espigado I, Martín-Peña A, et al. Optimisation of empirical antimicrobial therapy in patients with haematological malignancies and febrile neutropenia (How Long study): an open-label, randomised, controlled phase 4 trial. Lancet Haematol. 2017;4:e573-e583.
- Picard M, Robitaille G, Karam F, et al. Cross-reactivity to cephalosporins and carbapenems in penicillin-allergic patients: two systematic reviews and meta-analyses. J Allergy Clin Immunol Pract. 2019;7:2722-2738.e5.
- Tamma PD, Aitken SL, Bonomo RA, et al. Infectious Diseases Society of America guidance on the treatment of extended-spectrum ß-lactamase producing Enterobacterales (ESBL-E), carbapenem-resistant Enterobacterales (CRE), and Pseudomonas aeruginosa with difficult-to-treat resistance (DTR-P. aeruginosa). Clin Infect Dis. 2021;72:e169-e183.
- Codjoe FS, Donkor ES. Carbapenem resistance: a review. Med Sci (Basel). 2018;6:1.
- Girmenia C, Rossolini GM, Piciocchi A, et al. Infections by carbapenem-resistant Klebsiella pneumoniae in SCT recipients: a nationwide retrospective survey from Italy. Bone Marrow Transplant. 2015;50:282-288.
- Gedik H, Şimşek F, Kantürk A, et al. Bloodstream infections in patients with hematological malignancies: which is more fatal—cancer or resistant pathogens? Ther Clin Risk Manag. 2014;10:743-752.
- van Duin D, Arias CA, Komarow L, et al; for the Multi-Drug Resistant Organism Network investigators. Molecular and clinical epidemiology of carbapenem-resistant Enterobacterales in the USA (CRACKLE-2): a prospective cohort study. Lancet Infect Dis. 2020;20:731-741. Erratum in: Lancet Infect Dis. 2020;20:e116.
- Baker TM, Satlin MJ. The growing threat of multidrug-resistant Gram-negative infections in patients with hematologic malignancies. Leuk Lymphoma. 2016;57:2245-2258.
- Vossen MG, Milacek C, Thalhammer F. Empirical antimicrobial treatment in haemato-/oncological patients with neutropenic sepsis. ESMO Open. 2018;3:e000348.
- Micozzi A, Ansuinelli M, Minotti C, et al. Ceftazidime-avibactam as empiric therapy in febrile neutropenic high-risk haematological patients, HMpts, colonized with carbapenem-resistant Klebsiella pneumoniae (CRKP). Presented at the European Congress of Clinical Microbiology and Infectious Diseases; April 21-24, 2018; Madrid, Spain. Abstract P0681.
- Hachem R, Reitzel R, Rolston K, et al. Antimicrobial activities of ceftazidime-avibactam and comparator agents against clinical bacteria isolated from patients with cancer. Antimicrob Agents Chemother. 2017;61:e02106-16.
- Goodlet KJ, Nicolau DP, Nailor MD. In vitro comparison of ceftolozane-tazobactam to traditional beta-lactams and ceftolozane-tazobactam as an alternative to combination antimicrobial therapy for Pseudomonas aeruginosa. Antimicrob Agents Chemother. 2017;61:e01350-17.
- Tamma PD, Villegas MV. Use of ß-lactam/ß-lactamase inhibitors for extended-spectrum-ß-lactamase infections: defining the right patient population. Antimicrob Agents Chemother. 2017;61:e01094-17.
- Davido B, Fellous L, Lawrence C, et al. Ceftazidime-avibactam and aztreonam, an interesting strategy to overcome ß-lactam resistance conferred by metallo-ß-lactamases in Enterobacteriaceae and Pseudomonas aeruginosa. Antimicrob Agents Chemother. 2017;61:e01008-17.
- Lohans CT, Brem J, Schofield CJ. New Delhi metallo-ß-lactamase 1 catalyzes avibactam and aztreonam hydrolysis. Antimicrob Agents Chemother. 2017;61:e01224-17.
- Zhang B, Zhu Z, Jia W, et al. In vitro activity of aztreonam–avibactam against metallo-ß-lactamase-producing Enterobacteriaceae—a multicenter study in China. Int J Infect Dis. 2020;97:11-18.
- Lapuebla A, Abdallah M, Olafisoye O, et al. Activity of meropenem combined with RPX7009, a novel ß-lactamase inhibitor, against Gram-negative clinical isolates in New York City. Antimicrob Agents Chemother. 2015;59:4856-4860.
- Young K, Painter RE, Raghoobar SL, et al. In vitro studies evaluating the activity of imipenem in combination with relebactam against Pseudomonas aeruginosa. BMC Microbiol. 2019;19:150.
- Gudiol C, Aguilar-Guisado M, Azanza JR, et al. Executive summary of the consensus document of the Spanish Society of Infectious Diseases and Clinical Microbiology (SEIMC), the Spanish Network for Research in Infectious Diseases (REIPI) and the Spanish Society of Haematology and Haemotherapy (SEHH) on the management of febrile neutropenia in patients with hematological malignancies. Enferm Infecc Microbiol Clin. 2020;38:174-181.
- Gudiol C, Royo-Cebrecos C, Abdala E, et al; for the BICAR study group. Efficacy of ß-lactam/ß-lactamase inhibitor combinations for the treatment of bloodstream infection due to extended-spectrum-ß-lactamase-producing Enterobacteriaceae in hematological patients with neutropenia. Antimicrob Agents Chemother. 2017;61:e00164-17.
- Recarbrio (imipenem, cilastatin, and relebactam) for injection, for intravenous use [prescribing information]. Merck; June 2020.
- Barnes MD, Bethel CR, Alsop J, et al. Inactivation of the Pseudomonas-derived cephalosporinase-3 (PDC-3) by relebactam. Antimicrob Agents Chemother. 2018;62:e02406-17.
- Motsch J, Murta de Oliveira C, Stus V, et al. RESTORE-IMI 1: a multicenter, randomized, double-blind trial comparing efficacy and safety of imipenem/relebactam vs colistin plus imipenem in patients with imipenem-nonsusceptible bacterial infections. Clin Infect Dis. 2020;70:1799-1808.
- Johnston BD, Thuras P, Porter SB, et al. Activity of cefiderocol, ceftazidime-avibactam, and eravacycline against carbapenem-resistant Escherichia coli isolates from the United States and international sites in relation to clonal background, resistance genes, coresistance, and region. Antimicrob Agents Chemother. 2020;64:e00797-20.
- Bassetti M, Echols R, Matsunaga Y, et al. Efficacy and safety of cefiderocol or best available therapy for the treatment of serious infections caused by carbapenem-resistant Gram-negative bacteria (CREDIBLE-CR): a randomised, open-label, multicentre, pathogen-focused, descriptive, phase 3 trial. Lancet Infect Dis. 2021;21:226-240.
- Tamma PD, Hsu AJ. Defining the role of novel ß-lactam agents that target carbapenem-resistant Gram-negative organisms. J Pediatric Infect Dis Soc. 2019;8:251-260.
- Doan VP, Yeh JC, Gulbis AM, et al. Levofloxacin versus cefpodoxime for antibacterial prophylaxis in allogeneic stem cell transplantation. Biol Blood Marrow Transplant. 2019;25:1637-1641.