The 5-year survival rate for patients with advanced or metastatic renal-cell carcinoma (RCC) has increased in the past 20 years, from 7.3% to 11.7%.1 This improvement can be attributed to advancements in the treatment of RCC, including the development of oral targeted agents, such as tyrosine kinase inhibitors (TKIs) and mammalian target of rapamycin (mTOR) inhibitors. As of September 2021, a total of 9 oral targeted agents have been approved by the US Food and Drug Administration (FDA) for the treatment of metastatic RCC, including axitinib, cabozantinib, erlotinib, everolimus, lenvatinib, pazopanib, sorafenib, sunitinib, and tivozanib.
Although oral targeted agents have had better tolerability, improved outcomes, and easier administration than cytokine-based therapies,2 the data are limited in patients with renal impairment or with end-stage renal disease (ESRD) who are undergoing dialysis. Many of the pivotal clinical trials that led to the approval of these oral targeted therapies in RCC excluded patients with renal impairment or ESRD who were undergoing dialysis, because of the potential for altered metabolism and the elimination of therapies in the context of dialysis.2 The available data are limited to small patient populations and/or do not include more recent oral targeted agents, such as cabozantinib.2-5
It is critical to determine the appropriate treatment regimens for patients with RCC and concurrent renal impairment, because the diagnosis of RCC may increase the risk for renal insufficiency.3 Gupta and colleagues report that 33% of patients with metastatic RCC have renal dysfunction.4 A retrospective cohort study that included nearly 11,000 patients with RCC showed that 25.4% of the patients had at least 1 renal adverse outcome, with 6% of the patients progressing to dialysis or requiring renal transplantation.6
This information poses a challenge when determining the appropriate treatment regimens, because many of the oral targeted agents (including axitinib, cabozantinib, lenvatinib, sorafenib, and sunitinib) that are used for the treatment of metastatic RCC are at least partially eliminated through the kidneys.7-11 Thus, there is concern that patients may have increased adverse events with these medications in the setting of renal dysfunction. Several studies, some of which have a small number of patients and include case series and reports, have shown that oral targeted agents are tolerated in patients with moderate-to-severe renal impairment or ESRD who are undergoing dialysis.2-5
A retrospective review by Czarnecka and colleagues demonstrated the safe and effective use of sunitinib, sorafenib, and pazopanib in 9 patients with RCC who were undergoing hemodialysis.3 However, Gupta and colleagues reported that patients with RCC and renal insufficiency who received sunitinib or bevacizumab had an increased incidence of hypertension, with higher rates of rash and dose interruptions with mTOR inhibitors, compared with patients with normal renal function.4
In addition, a study by Josephs and colleagues showed an increased risk for diarrhea, hand-foot skin reaction, and neutropenia in 10 dialysis-dependent patients compared with non–dialysis-dependent patients.5 Despite indicating a correlation between oral targeted agents adverse events and renal dysfunction, both studies concluded that patients with moderate-to-severe renal impairment or patients who were undergoing dialysis could safely receive oral targeted agents if they are closely monitored.4,5 To our knowledge, no similar data are available involving the more recent FDA-approved targeted therapies for RCC.
These limitations in the current literature warrant further clarification and investigation of the safety, tolerability, and appropriate monitoring of oral targeted agents in patients with RCC and renal dysfunction.
The purpose of our study was to assess the tolerability, safety, and efficacy of FDA-approved oral targeted agents for metastatic RCC in patients with moderate-to-severe renal impairment or with ESRD who are undergoing dialysis, to provide guidance for clinicians when managing patients with metastatic RCC.
Methods
This retrospective study reviewed the electronic health records (EHR) of patients with metastatic RCC and baseline renal impairment who received treatment with an oral targeted agent at a single-site academic medical center between June 2008 and April 2020.
The study included patients aged ≥18 years with a baseline creatinine clearance (CrCl) <60 mL/min, or with ESRD who were undergoing dialysis, had histologically confirmed metastatic RCC, and received an oral targeted agent (ie, sunitinib, pazopanib, everolimus, axitinib, cabozantinib, or sorafenib). All patients had to have a documented assessment of any adverse events in this medical center’s EHR system. Patients who were enrolled in a clinical trial during the period in which they were receiving an oral molecularly targeted agent were excluded from the study.
CrCl was calculated using the Cockcroft-Gault formula. Renal impairment was defined as a CrCl of <60 mL/min according to the Kidney Disease: Improving Global Outcomes 2012 clinical practice guideline.12 Moderate renal dysfunction was defined as a CrCl of 30 mL/min to <60 mL/min, and severe renal dysfunction was defined as a CrCl of <30 mL/min.
Adverse events were graded according to the National Cancer Institute Common Terminology Criteria for Adverse Events version 5. The grading of adverse events was performed and assessed by the primary investigator, when provider assessment was unavailable. Treatment episode was defined as the time in which an individual patient received a specific oral targeted agent. The duration of therapy was defined as the time from the initiation of an oral molecularly targeted agent to treatment discontinuation for any reason.
Progression-free survival (PFS) was defined as the time from the initiation of an oral molecularly targeted agent to the time of disease progression or death from any cause. Overall survival (OS) was defined as the time from the initiation of an oral molecularly targeted agent to the time of death from any cause.
The co-primary end points of this study included the incidence and grade of adverse events while receiving an oral targeted agent. The secondary end points included the rates of dose adjustments and treatment interruptions and discontinuations of an oral targeted agent because of adverse events, as well as response to an oral molecularly targeted agent (defined using the Response Evaluation Criteria in Solid Tumours [RECIST] v1.1 criteria), PFS, and OS.
The patient characteristics included the median and range of continuous variables and the frequency and percentage of categorical variables. OS and PFS outcomes were analyzed using Kaplan-Meier estimates and curves.
Results
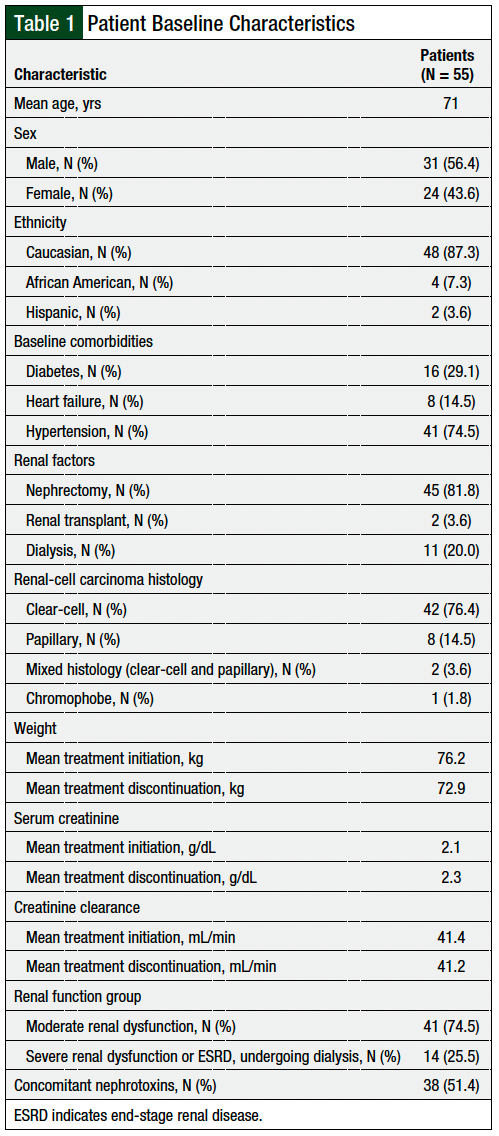
A total of 55 patients with metastatic RCC who were receiving a total of 74 oral molecularly targeted agents met the study inclusion criteria. The baseline patient characteristics are shown in Table 1. The patients’ median age was 71 years. A total of 38 (51.4%) patients received concomitant nephrotoxins. Overall, 11 (20%) patients were undergoing dialysis at the initiation of an oral targeted therapy. The patients’ weight decreased throughout treatment, with an average weight of 76.2 kg at treatment initiation and 72.9 kg at treatment discontinuation. The patients’ serum creatinine and CrCl levels remained relatively stable throughout the treatment with an oral targeted agent.
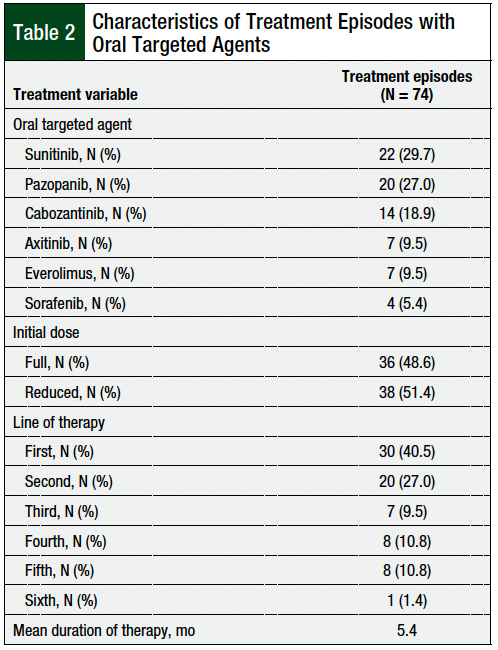
The treatment characteristics associated with oral targeted agents used in this study are shown in Table 2. The most frequently prescribed oral targeted agents were sunitinib (29.7%) and pazopanib (27%), followed by cabozantinib (18.9%), axitinib (9.5%), everolimus (9.5%), and sorafenib (5.4%). Most of the oral targeted agents in this study were used in the first- or second-line setting (range, 1-6). In 36 (48.6%) treatment episodes, the patients started treatment with an oral targeted agent at full dose; in the remaining 38 (51.4%) episodes, the patients started treatment with a reduced dose or an adjusted schedule. The mean duration of therapy was approximately 5.4 months.
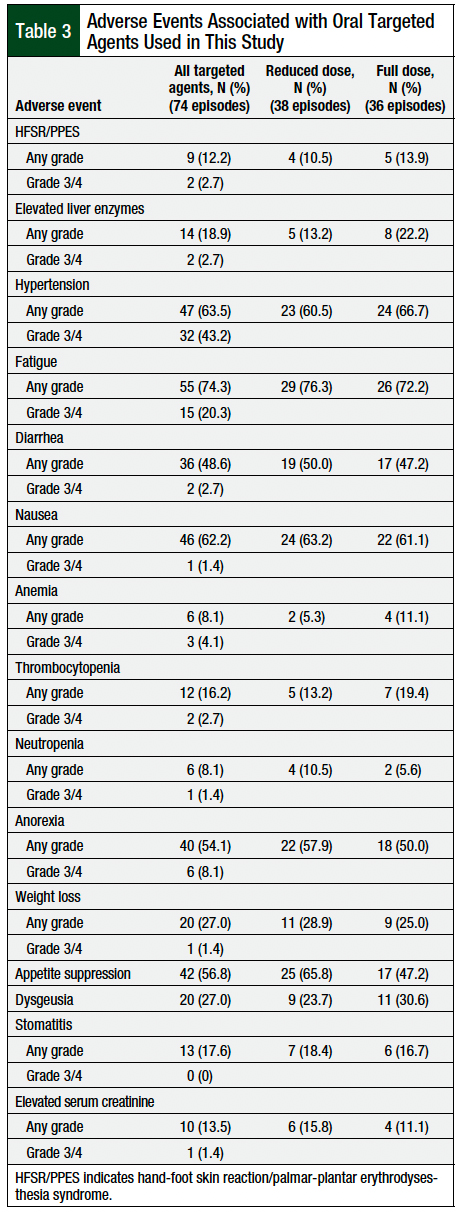
A total of 72.7% of the patients had a grade 1 or 2 adverse event, 67.3% of the patients had a grade 3 or 4 adverse event, and no grade 5 adverse events (ie, deaths) occurred. The incidence and severity of each adverse event that was reported with the 74 treatment cycles of oral targeted agents are shown in Table 3. The most frequent adverse events included fatigue (74.3%), hypertension (63.5%), nausea (62.2%), appetite suppression (56.8%), anorexia (54.1%), diarrhea (48.6%), weight loss (27%), and dysgeusia (27%).
The most common grade ≥3 adverse events included hypertension (43.2%) and fatigue (20.3%). Of note, 28 (51%) patients who had hypertension after receiving an oral targeted agent had preexisting hypertension. The incidence of adverse events for patients who initiated treatment with a reduced dose of an oral targeted agent versus those who received a full dose of those drugs are shown in Table 3.
The incidence rates of adverse events were similar in patients who started treatment with a reduced or a full dose. The incidence and grade of adverse events were similar between the patients with moderate renal impairment and patients with severe or ESRD who had undergone dialysis (Appendix Table A).
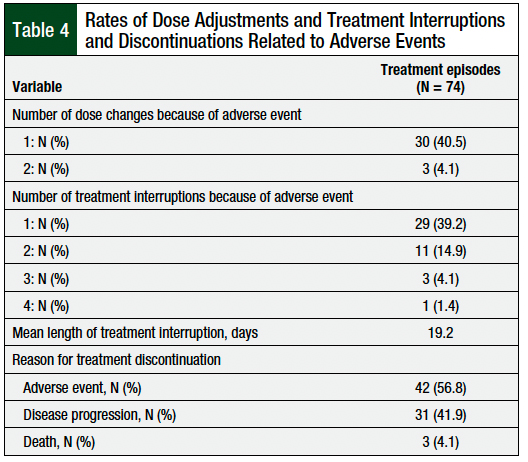
The rates of dose adjustments and treatment interruptions and discontinuations are shown in Table 4. The dose reduction because of an adverse event related to an oral targeted agent was required in 33 (44.6%) treatment episodes. Treatment interruptions were required at least once in 44 (59.6%) treatment episodes because of an adverse event.
Treatment discontinuations because of an adverse event occurred in 42 (56.8%) treatment episodes. The rates of treatment discontinuations because of an adverse event were 68.5% with pazopanib, 68.2% with sunitinib, and 46.2% with cabozantinib. An oral targeted agent was discontinued because of fatigue in 12 (22%) patients, nausea in 7 (13%) patients, anorexia in 7 (13%) patients, diarrhea in 6 (11%) patients, and elevated liver function tests in 5 (9%) patients (not shown).
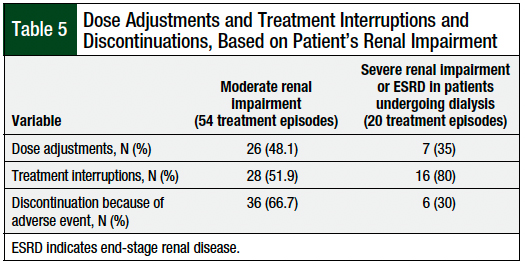
The moderate renal impairment group had higher rates of dose adjustments (48.1% vs 35%, respectively) and treatment discontinuation (66.7% vs 30%, respectively) as a result of an adverse event than the severe renal impairment or ESRD on dialysis group; however, the rate of treatment interruptions was higher in the severe impairment or ESRD on dialysis group than in the moderate renal impairment group (80% vs 51.9%, respectively; Table 5).
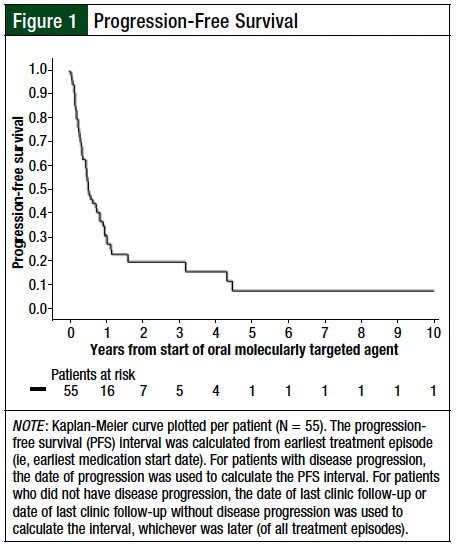
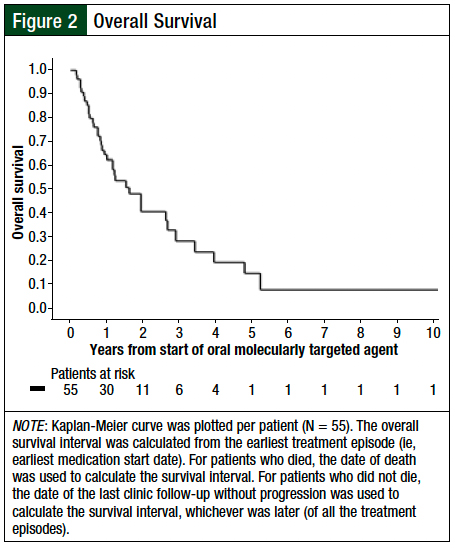
Treatment was discontinued because of disease progression in 31 (41.9%) treatment episodes and because of death in 3 (4.1%; Table 4). A total of 17 (30.9%) patients were still receiving treatment at the completion of the data collection. The best response per the RECIST criteria included a partial response in 19 (25.7%) treatment episodes, stable disease in 16 (21.6%) treatment episodes, and progressive disease in 7 (9.5%) treatment episodes (Appendix Table B). The median PFS was 6.7 months (Figure 1). At last follow-up, 38 (69.1%) patients had died, with a median OS of 18.4 months (Figure 2).
Discussion
Although the metabolism of oral molecularly targeted agents, including TKIs and mTOR inhibitors, occurs in the liver, many of these agents are excreted in urine. However, previous case reports have suggested that these medications are safe in patients with renal impairment or with ESRD undergoing dialysis, if monitored closely.2-5
The results of our study demonstrated a high incidence of adverse events in patients with metastatic RCC who were receiving an oral targeted agent and had renal impairment or ESRD and were undergoing dialysis. Because our study does not have a control cohort, comparing the incidence of adverse events with these targeted therapies in patients with impaired renal function versus patients with normal renal function (CrCl >60 mL/min) in previous studies13,14 can provide further insight into the impact of renal function on treatment tolerability.
In the CABOSUN clinical trial, Choueiri and colleagues reported an incidence rate of any-grade adverse events of 99% with cabozantinib and a rate of 99% with sunitinib,13 rates that are similar to our study, which showed an adverse event incidence rate of 100% with cabozantinib and 95% with sunitinib. Although Choueiri and colleagues reported an incidence of grade 3 or 4 adverse events of 67% with cabozantinib and 68% with sunitinib,13 our study demonstrated an incidence rate of 100% with cabozantinib and of 86% with sunitinib. The CABOSUN study reported grade 5 adverse events in 5% in the cabozantinib group and 7% in the sunitinib group13; by contrast, our study did not report any grade 5 adverse events in patients using those drugs.
The most common adverse events in the study by Choueiri and colleagues were also very similar to those in our study, including fatigue, hypertension, diarrhea, and anorexia.13 Of note, Choueiri and colleagues reported grade 3 or 4 hypertension in 28% of patients receiving cabozantinib and 22% of patients receiving sunitinib; the incidence rate in our study was 50% with cabozantinib and 36% with sunitinib (Appendix Table C). Grade 3 or 4 fatigue was also higher in our study, at 29% with cabozantinib and 18% with sunitinib versus 6% with cabozantinib and 15% with sunitinib in the CABOSUN trial.13
In addition, Sternberg and colleagues demonstrated significant adverse events in patients with normal renal function who received pazopanib for the treatment of locally advanced or metastatic RCC in a randomized phase 3 clinical trial. A total of 40% had hypertension, 52% had diarrhea, and 26% had nausea.14 In our study, 60% of patients who received pazopanib had hypertension, 45% had diarrhea, and 65% had nausea. Overall, our study demonstrated incidences of any-grade or grade 1 or 2 adverse events that were similar to, and higher incidences of grade 3 or 4 adverse events than in previous studies of patients with normal renal function.13,14
The significant adverse events in patients with RCC who are receiving TKIs often lead to treatment interruptions and discontinuations. Although the incidence of treatment interruptions is not well-documented in the literature,2-5 59% of patients in our study had treatment interruptions. Treatment discontinuation resulting from adverse events occurred at a much higher rate in our study (57%) than in the CABOSUN study (20%),13 the study by Sternberg and colleagues (14%),14 and the study by Shetty and colleagues (16%).2
Regarding efficacy, the median PFS of patients receiving pazopanib was 9.2 months in the Sternberg and colleagues study,14 and 8.2 months for cabozantinib and 5.6 months for sunitinib in the study by Choueiri and colleagues.13 The median PFS in our study was 5.9 months with pazopanib, 5 months with cabozantinib, and 12.6 months with sunitinib.
An interim analysis by Sternberg and colleagues revealed a median OS of 61%14 compared with 62.1% in our study across all oral molecularly targeted agents. This shows similar OS outcomes and an increased median PFS in patients with renal impairment who received pazopanib or cabozantinib compared with previous studies in patients with normal renal function.13,14
Although previous studies in patients with metastatic RCC and renal impairment included a variety of TKIs, they did not include more recent agents, such as cabozantinib, in the setting of metastatic RCC. Our study evaluated cabozantinib in patients with mild-to-moderate renal impairment, and in patients undergoing dialysis, which represented 18.9% of the patients in our study.
Our study demonstrated a high incidence of adverse events, particularly grades 3 and 4, for patients with renal impairment receiving cabozantinib. None of these patients had grade 5 adverse events, which highlights the importance of proceeding with caution and monitoring closely for adverse events when prescribing cabozantinib to patients with renal impairment.
Finally, we did not find significant differences in adverse events between patients who received the full dose and those who received a reduced dose of oral targeted agents at treatment initiation. However, many of the patients were escalated or titrated to a higher or full dose, making it difficult to determine if there were any differences in tolerance at the lower doses.
Providers must exercise caution when prescribing oral targeted agents in patients with metastatic RCC and renal impairment or ESRD who are undergoing dialysis. The incidence of adverse events remains high with these agents, with a potential for an increased incidence of grade 3 and 4 adverse events, as well as an increased risk for treatment discontinuation. This increased risk of severe adverse events may point to the growing exposure to the agents; however, additional studies are warranted to further define differences in the safety and tolerability of these agents in patients with normal versus impaired renal function.
Limitations
This study had only 1 independent reviewer for all adverse events and for determining disease progression.
Furthermore, this was a retrospective study with a small patient population.
In addition, the number of patients who received each specific oral molecularly targeted agent differed, which rendered direct comparisons between these agents challenging.
Moreover, this study had no direct control cohort. Further analysis with a control group may aid in detecting differences in clinical outcomes in terms of safety and efficacy of oral molecularly targeted agents in patients with metastatic RCC and renal impairment.
Finally, proteinuria was not regularly monitored in these patients but is a known adverse event of some of these oral targeted agents, which limits the assessment of the safety of these agents in this patient population.
Conclusion
The incidence of adverse events in patients with metastatic RCC receiving an oral targeted agent remains prominent in those with renal impairment. The incidence of grade 3 or 4 adverse events and treatment discontinuations because of adverse events were higher in our study than in previous studies involving patients with normal renal function. The OS outcomes in our study were similar to results of landmark clinical trials, despite multiple dose reductions and treatment interruptions, which nevertheless led to changes in the median PFS in these patients. Our results provide new information about the use of cabozantinib in patients with RCC and renal impairment, demonstrating decreased safety and efficacy in this population.
These results raise questions about the safety of oral targeted agents in patients with metastatic RCC and renal impairment, but these drugs may still be considered for this patient population if increased monitoring is implemented. Our findings highlight the safety concerns of using these medications in patients with metastatic RCC and renal impairment, warranting additional investigation to provide guidance on specific dosing and sequencing of oral targeted agents in this vulnerable patient population.
Acknowledgments
We would like to acknowledge our statisticians, Ruta Brazauskas, PhD, and Bi Qing Teng, as well as Felicia Zook, PharmD, BCOP; Kristina Teso, PharmD, BCPS, BCOP; and Carolyn Oxencis, PharmD, BCOP.
Author Disclosure Statement
Dr McKernan, Dr Schmidt, and Dr Rhoades have no conflicts of interest to report.
References
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines): Kidney Cancer. Version 1.2022. July 1, 2021. www.nccn.org/professionals/physician_gls/pdf/kidney.pdf. Accessed September 23, 2021.
- Shetty AV, Matrana MR, Atkinson BJ, et al. Outcomes of patients with metastatic renal cell carcinoma and end-stage renal disease receiving dialysis and targeted therapies: a single institution experience. Clin Genitourin Cancer. 2014;12:348-353.
- Czarnecka AM, Kawecki M, Lian F, et al. Feasibility, efficacy and safety of tyrosine kinase inhibitor treatment in hemodialyzed patients with renal cell cancer: 10 years of experience. Future Oncol. 2015;11:2267-2282.
- Gupta S, Parsa V, Heilbrun LK, et al. Safety and efficacy of molecularly targeted agents in patients with metastatic kidney cancer with renal dysfunction. Anticancer Drugs. 2011;22:794-800.
- Josephs D, Hutson TE, Cowey CL, et al. Efficacy and toxicity of sunitinib in patients with metastatic renal cell carcinoma with severe renal impairment or on haemodialysis. BJU Int. 2011;108:1279-1283.
- Miller DC, Schonlau M, Litwin MS, et al. Renal and cardiovascular morbidity after partial or radical nephrectomy. Cancer. 2008;112:511-520.
- Inlyta (axitinib) tablets, for oral administration [prescribing information]. Pfizer; June 2020. http://labeling.pfizer.com/ShowLabeling.aspx?id=759. Accessed September 23, 2021.
- Cabometyx (cabozantinib) tablets, for oral use [prescribing information]. Exelixis; September 2021. www.cabometyxhcp.com/sites/default/files/2021-03/prescribing-information.pdf. Accessed September 23, 2021.
- Lenvima (lenvatinib) capsules, for oral use [prescribing information]. Eisai; August 2021. www.lenvima.com/-/media/Project/EISAI/Lenvima/PDF/prescribing-information.pdf. Accessed September 23, 2021.
- Nexavar (sorafenib) tablets, for oral use [prescribing information]. Bayer HealthCare Pharmaceuticals; July 2020. http://labeling.bayerhealthcare.com/html/products/pi/Nexavar_PI.pdf. Accessed September 23, 2021.
- Sutent (sunitinib malate) capsules, for oral use [prescribing information]. Pfizer; September 2021. http://labeling.pfizer.com/showlabeling.aspx?id=607. Accessed September 23, 2021.
- Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int Suppl. 2013;3:1-150.
- Choueiri TK, Halabi S, Sanford BL, et al. Cabozantinib versus sunitinib as initial targeted therapy for patients with metastatic renal cell carcinoma of poor or intermediate risk: the Alliance A031203 CABOSUN trial. J Clin Oncol. 2017;35:591-597. Errata in: J Clin Oncol. 2017;35:3736; J Clin Oncol. 2018;36:521.
- Sternberg CN, Davis ID, Mardiak J, et al. Pazopanib in locally advanced or metastatic renal cell carcinoma: results of a randomized phase III trial. J Clin Oncol. 2010;28:1061-1068.