Dr Mancini is Oncology Pharmacist, St Luke’s Mountain States Tumor Institute; Dr Kramer is Oncology Pharmacist, St Luke’s Mountain States Tumor Institute; and Ms Powell is Pharmacy Technician and Billing Specialist, St Luke’s Health System Outpatient Pharmacy, Boise, ID.
Background: The dispensing and management of oral chemotherapies involves many challenges, with access to and the finances of oral agents being the biggest barriers to treatment. The oncology literature is focused on the clinical benefits of on-site dispensing and management programs; however, little to no data are available regarding the financial benefits to third-party payers.
Objective: To evaluate if on-site drug dispensing can reduce unnecessary dispensing of oral chemotherapies, which would help to reduce waste, lower drug costs, and ensure rapid start of therapy.
Methods: The St Luke’s Mountain States Tumor Institute oral chemotherapy office conducted a 6-month prospective evaluation from March 2011 to September 2011 of all patients receiving active oral chemotherapy. During this time frame, any cancer-related drug prescription that was returned for credit was evaluated for its start date in relation to the date of the visit to the oncologist. Prescriptions were evaluated if they were permanently discontinued as a result of disease progression, or if a dose change resulted in a new dosing form that could not be made with the current dosage units. The costs of the unused agents were then computed based on the average wholesale price (AWP) of the specific drug.
Results: During the 6-month period, a total of 39 prescriptions (for 37 patients) were returned for credit. The total amount saved based on the AWP for the 39 agents was $103,567.33. In addition, the amount saved in copayments was $13,850.34; of that, $9134.28 would have come from assistance funds and $2760.09 would have been covered by retroactive secondary insurance billing. After subtracting the patients with secondary insurance as well as the copay assistance funds, a total of 21 patients had out-of-pocket costs totaling $1955.97 worth of copayments, which averages $93 per patient.
Conclusion: On-site dispensing of oral chemotherapy agents can reduce prescription medication waste and therefore reduce overall costs for health insurance plans, patients, and assistance foundation funds. Tighter control of dispensing, by keeping medications under the pharmacist’s control until patients see their oncologist, can eliminate waste and unnecessary dispensing of rather expensive medications, which further serves as a financial incentive for on-site dispensing.
There are many challenges associated with the dispensing and management of oral chemotherapy agents. Complications related to the rapid rate of drug development, financial concerns, medication adherence, monitoring of drug side effects, and drug–food and drug–drug interactions all combine to create a vast network of complexity that goes beyond the management techniques used to treat patients with intravenous oncolytics.
Since 2007, 15 new oral oncolytics have been introduced to the US market, representing an average approval rate of 1 new drug every 4 months.1 This reflects an acceleration of new oral oncolytics hitting the market 12 times faster than in the past 50 years.
As cancer centers in the United States look for ways to address these challenges, they need to find a way to pay for the resources that are allocated to managing patients with cancer. Despite the use of a mail-order pharmacy, many aspects of the care of these patients still have to be addressed by the patient’s treatment center. The oncology literature is focused on the clinical benefits of on-site dispensing and management programs,2-4 but little to no data are available on the financial benefits of on-site dispensing to third-party payers. There are ways to ensure that resources can get paid for, provided that these clinics also have dispensing pharmacies.
One of the most significant barriers to the optimal management of oral oncolytics is the financial component of costs to the patient and to the health insurance plan. One aspect of this is the requirement of certain health insurance companies to use a specific mail-order pharmacy because the specific center’s pharmacy is not “a contract provider.” In some cases, this can be overcome as easily as having a discussion with the insurance company and getting on contract. However, some insurance companies only allow prescriptions to be filled through a single mail-order pharmacy, in which case neither the patient nor the provider has any choice in how the patient obtains the medication.
This is potentially problematic, because the direct lines of communication that exist between an internal pharmacy and the oncologist’s office do not exist with external pharmacies. In addition, patients will rarely have direct interactions with the healthcare team, specifically a pharmacist, if patients are required to use a mail-order pharmacy, and this may compromise optimal therapy for the patient.5
When patients are treated with oral chemotherapy agents, oncologists prefer to see their patients on the day of, or a few days before, the start of their next cycle. Patients are therefore responsible for ensuring that they have their medication with them that day. If they are required to use a mail-order pharmacy, often the patients have already called to request their refill to ensure that they have it on day 1 of their treatment cycle.
Once a prescription has left a pharmacy’s control, the pharmacy cannot legally reuse the medication, because a pharmacy’s proper storage conditions cannot be guaranteed. Because a pharmacy cannot reuse the medication, it cannot credit the drug cost, leading to charges for a medication that will never be used.
The goal of this article is to evaluate how on-site drug dispensing can provide a mechanism for reducing the unnecessary dispensing of oral oncolytics, which can lead to financial savings and ensure that there are no delays in the start of therapy.
Methods
The St Luke’s Mountain States Tumor Institute oral chemotherapy office conducted a 6-month prospective evaluation from March 2011 to September 2011 of all patients receiving active oral chemotherapy to investigate the potential cost-savings by tracking any prescription that was returned for credit. Within this program, prescriptions for oral oncolytics are sent to the central oral chemotherapy office, which processes the prescription and fills it in conjunction with the outpatient dispensing pharmacy.
Once prepared, the prescriptions are sent to 1 of 5 outpatient cancer centers, where the site pharmacist dispenses the medication to the patient after that patient has seen the oncologist. If a patient’s treatment is discontinued at that oncologist’s visit as a result of disease progression or drug toxicity, the prescription is returned to the central pharmacy for credit, because the medication remained under the pharmacist’s control.
During the 6-month time frame of this study, any prescription that was returned for credit was evaluated for the start date in relation to the date of the oncologist’s visit. If the patient was due to start the medication on the day of, or the day after, the oncologist’s visit, that prescription was documented, including the medication name, the dosage, and the number of tablets supplied in that fill, before being returned to stock.
In this analysis, prescriptions were evaluated if they were permanently discontinued as a result of disease progression or if a dose change resulted in a new dosage form that could not be made with the current dose. For example, a dose reduction for sunitinib from 50 mg to 37.5 mg would require replacing the prescription with new capsule sizes, and would therefore be included for analysis. An alternate example, such as reducing capecitabine from 1500 mg to 1000 mg twice daily, would not be included, because the patient could use the same tablet sizes in the prescription. These types of changes were not included in the analysis, because it would be assumed that the pharmacy would adjust the quantity of drugs to be dispensed for the subsequent cycle.
Finally, the price of each of the prescriptions was then computed using the average wholesale price (AWP). The AWP was chosen as a benchmark because most third-party payers, dispensing pharmacies, and clinics calculate what they pay or what they are reimbursed for in relation to the AWP and can calculate their own impact. In addition, the pharmacy records were reviewed to determine what the patient’s copayment responsibility would be if they had filled the medication. All patient charts were evaluated for documentation confirming the availability of secondary insurance or if the patients were receiving financial assistance to cover their co-payments.
Results
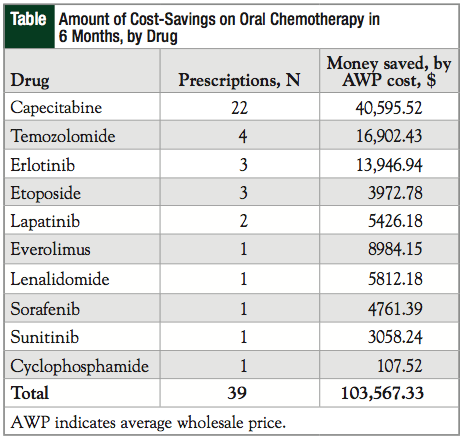
Between March 2011 and September 2011, a total of 37 patients had 39 prescriptions returned for credit, which met the criteria for inclusion in this analysis. Of these, 2 patients were receiving combined-modality treatment (1 with lapatinib and capecitabine and 1 with cyclophosphamide and etoposide). In addition, 4 patients were receiving multiple-dose strengths of the same drug to make their total daily dosage (3 patients receiving capecitabine and 1 patient receiving temozolomide). The most frequently returned medication was capecitabine.
As shown in the Table, the total amount that was saved based on the AWP for this 6-month period was $103,567.33.
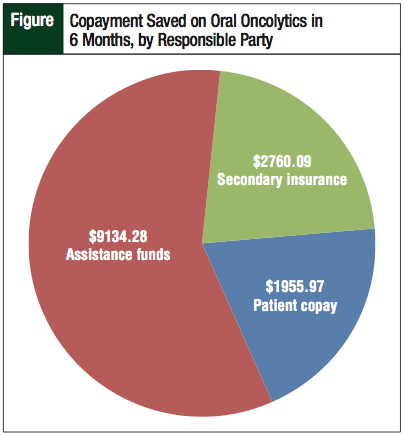
In addition, the amount saved by patients in copayments was $13,850.34, of which $9134.28 would have come from assistance funds and $2760.09 would have been covered by retroactive secondary insurance billing. After subtracting the patients with secondary insurance as well as copay assistance funds, 21 patients had out-of-pocket costs totaling $1955.97 worth of copayments, which averages $93 per patient (Figure).
Discussion
The analysis by St Luke’s Mountain States Tumor Institute oral chemotherapy program was able to show a potential extrapolated annual savings of more than $200,000 based on this prospective evaluation. By avoiding unnecessary dispensing, costs can be reduced for insurance plans that are paying a bulk of the cost, for patients paying out-of-pocket expenses (averaging approximately $100 per patient), and for copay assistance foundation funds, which can be used for other patients who are seeking financial assistance. By allowing more tightly controlled dispensing of chemotherapy prescriptions and ensuring that the prescription stays within the control of the pharmacy until the patient sees the oncologist, we are able to eliminate waste and the unnecessary dispensing of rather expensive medications.
The issue that a mail-order pharmacy may face is getting the prescription to the patient on time versus dispensing medication that may get discontinued when the patient sees his or her oncologist. This issue can be overcome by allowing an on-site pharmacy to dispense for the patients, because the direct interaction between the pharmacy and the oncologist allows the medication to be ready in time while not dispensing medication that will not be utilized.
One of the struggles that cancer centers face is putting the resources into processes that do not provide a revenue source to pay for those resources. This is essentially what happens when a cancer center is unable to fill medications for its patients.
By allowing on-site dispensing at centers that have proper management programs in place, these institutions can pay for the resources that are required to ensure that these patients are followed appropriately. Many centers face ongoing challenges with limited distribution models and insurance contracts that prevent them from dispensing drugs to their patients. In some cases, the health plan may force a patient to get his or her medication from a specific mail-order pharmacy, or may provide incentives to the patient for using that pharmacy by providing lower copayments. It can also be difficult to coordinate financial assistance for patients, because many pharmacies will not disclose copayment information with the clinic staff, such as social workers or financial advocates, leading to difficulty in ensuring that patients get their drugs at an affordable cost.
As has already been discussed in the medical literature, direct access to laboratories, full medication lists, and oncologist visits have established the clinical benefit of on-site dispensing and pharmacist involvement, yet we still struggle without financial data.2-4 The data that are provided in this article can help to provide leverage for cancer centers that are seeking to be a “contract pharmacy” with various payers and to show that these types of programs may be able to save them money.
Although the dollar amount shown in this analysis is spread over several health plans and may seem insignificant to a single payer, more cancer centers are seeking ways to incorporate the on-site dispensing of oral oncolytics. In the 12 months since this analysis, the workload of St Luke’s Mountain States Tumor Institute oral chemotherapy office has doubled. In addition, the field of oral oncolytics is constantly growing.
In the past 9 years (since 2004), 22 new oral cancer agents have been approved by the US Food and Drug Administration (FDA), representing an approval rate of 1 new cancer medication approximately every 5 months, based on FDA approvals.1 If we look at just the past 5 years, 15 new drugs have been approved, further increasing the average approval rate to 1 new drug every 4 months.1 This represents an acceleration of new oral oncolytics hitting the market at a rate 12 times faster than in the past 50 years. In addition, up to 35% of the cancer drugs in clinical trials are oral, which suggests that this issue will only grow in the future.6
Limitations
The main potential limitation to this evaluation was adequate documentation. Because it was the responsibility of the pharmacist working in the office that day to document the returns, it is possible that some of the tracking of returns may have been missed. It is possible that this dollar amount may be an understatement of the true potential savings.
Another potential area of savings that was not tracked is the capecitabine example that was stated before, where a dose might have been reduced, thereby leading to leftover tablets from a previous cycle. Adjusting the quantity of the subsequent fill under protocol may also save additional costs that were not calculated in this evaluation.
Conclusion
The unprecedented growth in oral chemotherapy agents means that as this field continues to grow, the potential for increases in cost-savings by allowing on-site dispensing is even bigger. Oral chemotherapy parity is a “hot topic,” and the present analysis can help provide leverage to those who are seeking it. Cancer centers are not asking to take over the market; they are simply asking for the chance to help their patients in the best way possible. One hopes that insurance companies will continue to recognize the clinical and financial benefits provided by these cancer centers.
Author Disclosure Statement
Dr Mancini is on the Speaker’s Bureau of Millennium Pharmaceuticals and is a Consultant to GlaxoSmithKline. Dr Kramer and Ms Powell reported no conflicts of interest.
References
1. US Food and Drug Administration. Drug approval reports by month. Report produced November 28, 2012. www.accessdata.fda.gov/scripts/cder/drugsatfda/index.cfm.
2. Mancini R, Wilson D. A pharmacist-managed oral chemotherapy program: an economic and clinical opportunity. Oncol Issues. January/February 2012:28-31.
3. Drenker K, Sondag A, Mancini R. Impact of a pharmacist-managed oral chemotherapy program on nonfulfillment rates. J Hematol Oncol Pharm. 2012;2:42-45.
4. Mancini R, Kaster LM, Vu B, et al. Implementation of a pharmacist-managed interdisciplinary oral chemotherapy program in a community cancer center.
J Hematol Oncol Pharm. 2011;1:23-30.
5. Jabbour EJ, Kantarjian H, Eliasson L, et al. Patient adherence to tyrosine kinase inhibitor therapy in chronic myeloid leukemia. Am J Hematol. 2012;87:687-691.
6. DeCardenas R, Helfrich JS. Oral therapies and safety issues for oncology practices. Oncol Issues. March/April 2010:40-42.