Allogeneic bone marrow transplant is a therapy that has the potential to cure several hematologic malignancies.1 One component of successful allogeneic transplant is the graft-versus-leukemia effect of the donor lymphocytes, which is when the donor graft contributes to the antileukemic properties of an allogeneic transplant.2 Despite the lifesaving potential of allogeneic bone marrow transplant, patients can have clinical complications from that procedure, including graft-versus-host disease (GVHD), an immune-mediated disorder that remains a major cause of late, non–relapse-related mortality.1,3 Patients with active chronic GVHD are more likely to report poor general and mental health, as well as functional impairments, limitations of physical activity, and pain compared with people who have no history of chronic GVHD.4
GVHD occurs after the hematopoietic system of a nongenetically identical donor is transplanted to a recipient.5 The donor immune cells target healthy host tissues, causing inflammation and immune dysregulation. Before 2005 (when a new consensus statement was published5), the classification of GVHD was divided into 2 types: acute GVHD (occurring ≤100 days posttransplant) and chronic GVHD (occurring >100 days posttransplant). The diagnosis of acute versus chronic GVHD was distinctly separated by day 100. Acute GVHD presents in target organs of the skin, gastrointestinal tract, or liver.6 By contrast, chronic GVHD occurs >100 days posttransplant and presents in target organs and other locations.3,6
The majority of GVHD diagnoses are based on clinical physical evaluations and patient interviews.5 The qualitative assessments of GVHD symptoms, particularly chronic GVHD, were inadequate to quantifying and comparing responses.7
To standardize the definitions and classifications of GVHD, in 2005 and in 2014 the National Institutes of Health (NIH) Consensus Conference formulated recommendations for diagnostic criteria, severity scoring, and response assessments for clinical trials to focus more on an organ-based disease presentation model.8,9 In 2005, the NIH Consensus Conference redefined the classification of acute and chronic GVHD by eliminating the time restriction of 100 days and reclassifying it based on distinct clinical syndromes, regardless of the presentation time.8 These new recommendations are widely adopted to therapeutic clinical trials; however, they have been difficult to incorporate into observational and retrospective studies, because the measurement tools are not often used in day-to-day clinical care.5
Matched unrelated donor allogeneic transplant recipients have a higher risk for chronic GVHD compared with matched related donor transplant recipients. The incidence of chronic GVHD for a matched related donor allogeneic transplant is roughly 20%, which increases to approximately 40% with a matched unrelated transplant.10 Of note, studies have reported even higher rates of chronic GVHD in patients undergoing matched related donor allogeneic transplant—approximately 63% with peripheral blood and 52% with bone marrow, 3 years posttransplant.11
Lee and colleagues analyzed data from the International Bone Marrow Transplant Registry and the National Marrow Donor Program to validate a new chronic GVHD scoring system.12 They found a higher incidence of cumulative chronic GVHD in recipients of unrelated donors compared with sibling donor transplants (63% vs 42% at 1 year, respectively; P <.0001), as well as more severe manifestations.12
The incidence of chronic GVHD varies widely among studies. In a meta-analysis using data from 9 randomized clinical trials, the 3-year aggregate cumulative incidence of any-stage chronic GVHD was 68% for peripheral blood stem cells and 52% for bone marrow transplantation.13 In addition, the majority of matched allogeneic transplants for the treatment of leukemia are using peripheral stem cells as the stem-cell source.14
Studies have shown that stem cells from a peripheral source have been associated with faster hematologic recovery and lower risk for relapse compared with bone marrow stem cells; however, the incidences of severe acute and chronic GVHD are higher.13,15,16
Several methods are used to decrease the incidence of GVHD, including optimizing donor selection, using long-term immunosuppressive medications, and T-lymphocytes depletion.8,9,11,17,18 One method to prevent acute GVHD, a known risk factor for chronic GVHD, is to incorporate a GVHD prophylaxis regimen, given before or close to the time of stem-cell infusion.3,15,19 These regimens consist of a calcineurin inhibitor (tacrolimus or cyclosporine) with low-dose methotrexate or mycophenolate mofetil.3,16,18
Antithymocyte globulin (ATG) is an antibody that is added for unrelated donor allogeneic transplants.18-21 ATG is a preparation method made by in vivo depletion of peripheral T-lymphocytes, primarily through complement-dependent lysis or activation-associated apoptosis.18 The ATG antibodies are derived from horses (ie, ATG-horse) or from rabbits (ie, ATG-rabbit) through immunization of the animals with thymocytes and purifying the immunoglobulin (Ig)G fraction from the serum.18,22,23 Currently, 2 brand-name agents are available in the United States, 1 for ATG-horse (Atgam) and 1 for ATG-rabbit (Thymoglobulin).
ATG-rabbit has also been shown to induce generation of regulatory T-cells (ie, Tregs) in vitro and in vivo.24 This mechanism is not found in ATG-horse, and accumulating data show convincing evidence for the role of Tregs in preventing GVHD after allogeneic transplant.24-26 Because they are derived from animals, ATG agents can cause infusion-related reactions when administered to humans.22,23
To prevent potentially life-threatening infusion-related reactions, the administration of ATG-horse involves a test dose before administering the full dose.22 ATG-rabbit does not require a test dose.23 Premedications, such as an antihistamine, antipyretic, and steroid, are given, and if an infusion-related reaction occurs, it is managed by slowing the infusion and/or administering hypersensitivity rescue medications.23
Several studies have compared the incidence of GVHD in patients undergoing allogeneic unrelated donor transplant, regardless of whether they receive ATG-rabbit.27 In a retrospective study, Ratanatharathorn and colleagues compared the outcomes of 197 unrelated donor transplant recipients who received GVHD prophylaxis with tacrolimus plus mycophenolate or with tacrolimus plus mycophenolate and ATG-rabbit.19 Preparation regimens were assigned according to the underlying diagnosis. The cumulative incidence of grade 3 or 4 acute GVHD was higher in the tacrolimus plus mycophenolate cohort, at 27% (95% confidence interval [CI], 19%-35%; P = .02) compared with the tacrolimus plus mycophenolate/ATG-rabbit group, at 14% (95% CI, 4%-24%; P = .02). The cumulative incidence of chronic GVHD was lower with adding ATG-rabbit, at 43% (95% CI, 40%-72%; P <.001) versus 56% (95% CI, 46%-66%; P <.001). The patients who received ATG-rabbit also had a significantly lower global severity of chronic GVHD (P <.001).19
A retrospective study by Ravinet and colleagues also showed a significant lower incidence of grade 3 or 4 acute and chronic GVHD in patients with acute myeloid leukemia (AML) or with myelodysplastic syndrome (MDS) who received myeloablative conditioning followed by matched unrelated donor transplant from peripheral stem cells.28 Literature directly comparing the efficacy and safety between the 2 ATG agents is not currently available.
The primary objective of our study was to compare the efficacy of the 2 ATG agents by assessing the incidence of chronic GVHD after switching from ATG-horse to ATG-rabbit. Several reasons for changing agents include the potential for a decrease in the incidence of hypersensitivity reactions with ATG-rabbit; elimination of ATG-horse test dose; and a study supporting the efficacy of ATG-rabbit in hematopoietic stem-cell transplant (HSCT) recipients in the prevention of chronic GVHD.20 Our hypothesis was that ATG-rabbit was noninferior to ATG-horse in the prevention of chronic GVHD.
The secondary objectives were to describe potential confounding factors and complications of patients undergoing allogeneic HSCT. These include frequency of acute GVHD, cytomegalovirus (CMV) reactivation, hypersensitivity reactions, and infections, as well as the average length of hospital stay. In addition, we analyzed the costs of drugs and length of hospital stay to estimate the financial savings after switching from ATG-horse to ATG-rabbit.
Methods
This was a single-center retrospective noninferiority study conducted at Henry Ford Hospital in Detroit, MI. The Henry Ford Transplant Institute has an expanding bone marrow transplant program that at the time of this study in 2017 was performing 100 HSCTs annually, of which 20 to 30 were unrelated donor HSCTs.
Patients who received an unrelated donor allogeneic HSCT between January 2005 and December 2015 were screened for inclusion in the study. To be considered in the analysis, patients had to meet 3 criteria, including being adults aged ≥18 years; receiving an allogeneic unrelated donor HSCT (peripheral or bone marrow) for a malignant or nonmalignant disorder; and receiving at least 1 dose of ATG.
Patients who received ATG-horse were administered 10 mg/kg for 2 intravenous (IV) doses 3 days before transplant (ie, D –3) and 3 days after transplant (ie, D +3). Patients who received ATG-rabbit were administered a total dose of 4.5 mg/kg, given intravenously over 3 days (0.5 mg/kg on D –5; 1.5 mg/kg on D –3; and 2.5 mg/kg on D –1).
Outcome Measures
The primary outcome measure was the incidence of chronic GVHD, including limited and extensive GVHD. Chronic GVHD was defined as GVHD occurring >100 days after the stem-cell infusion date. Secondary end points included the incidence of acute GVHD, cumulative incidence of CMV reactivation at 6 months, average length of hospital stay, incidence of hypersensitivity reactions, and overall incidence of infection. Acute GVHD was defined as GVHD that occurred ≤100 days after transplant. CMV reactivation was defined as CMV DNA quantitative copies >500 copies/mL for a minimum of 2 readings, with quantitative CMV monitored via polymerase chain reaction assay twice weekly.
Length of hospital stay was defined as the number of days from the date of hospital admission to the date of discharge or death. Hypersensitivity reactions were defined as any documented reaction attributed to an ATG agent that met the Common Terminology Criteria for Adverse Events description for allergic reaction, anaphylaxis, or cytokine-release syndrome.29 The incidence of infection was defined by the addition of antibiotics for the treatment of suspected infection.
The cost analysis was based on group purchasing organization (GPO) and on wholesale acquisition cost (WAC) prices. As of June 2017, the ATG-rabbit GPO and WAC prices were $565.91 for a 25-mg vial of IV powder for solution. ATG-horse was supplied as five 5-mL (50 mg/mL concentration) ampules per package. GPO and WAC prices were $7812.40 per package. The cost analysis compared the price of treatment for 87 patients, which is the number of patients who received ATG-rabbit after the ATG switch.
Statistical Analyses
The study was designed to determine noninferiority of ATG-rabbit to ATG-horse. The following assumptions were made to calculate the sample size: one-sided alpha = 0.025, beta = 0.20, and noninferiority margin = 0.15. Our calculations showed that 122 patients would be needed to detect a power of 80% to exclude a difference of 15% in the primary end point of chronic GVHD for each arm.
The noninferiority margin was defined as the one-sided 97.5% CI for the difference of the primary end point of chronic GVHD between the 2 groups. Confounding factors included in the bivariate logistical regression were age, female donor/male recipient combination, and acute GVHD.
We performed all statistical analyses using IBM SPSS Statistics for Windows v.22.0 (IBM Corp, Armonk, NY). Nominal values were compared using Pearson’s chi-square or Fisher’s exact test. We compared continuous variables with the Mann–Whitney U test.
The study’s primary end point was analyzed using a binomial logistic regression model that considers the following compounding factors: older recipient age, history of acute GVHD, and combination of female donor and male recipient. These are all risk factors that have been determined in the previous studies as contributing to chronic GVHD.30,31
Results
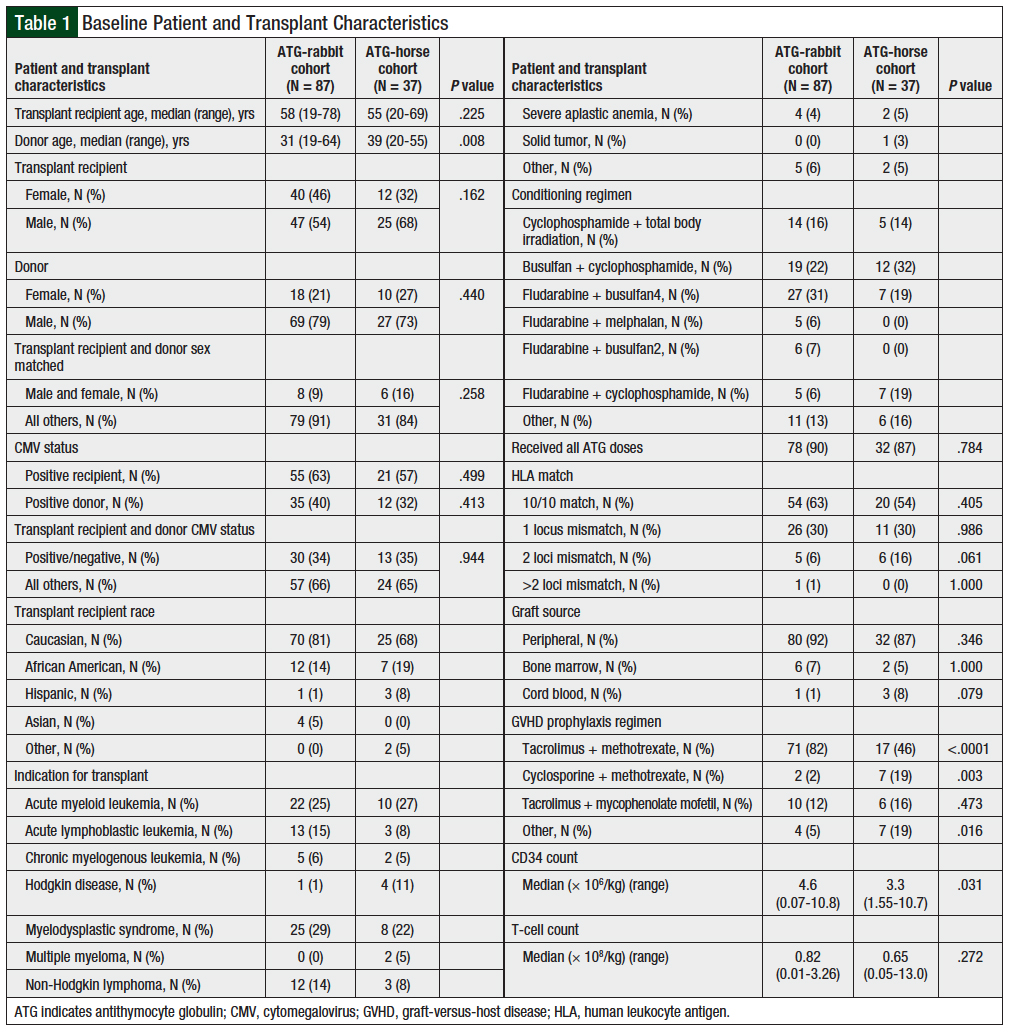
A total of 124 patients were included in the final analysis, comprising 37 patients in the ATG-horse group and 87 patients in the ATG-rabbit group. Patient characteristics are listed in Table 1. No major differences between groups were seen, except for the donor’s median age, which was not clinically significant. The combination of a male recipient and a female donor is an established risk factor for GVHD, but there was no difference between the incidence in recipients of ATG-horse versus ATG-rabbit (16% vs 9%; P = .258).
Baseline CMV serology can also predict the likelihood of CMV reactivation in the recipient. The combination of CMV-positive recipient and CMV-negative donor status is a risk factor for CMV reactivation in the recipient. No difference was observed between ATG-rabbit and ATG-horse (34% vs 35%, respectively; P = .944). The majority of patients who underwent transplant were white. AML was the most common indication for transplant in both groups (ATG-horse, 27% vs ATG-rabbit, 25%), followed by MDS (22% vs 29%, respectively,) and acute lymphocytic leukemia (ALL; 8% vs 15%, respectively). Of the ATG-rabbit group, 90% received all ATG doses versus 87% in the ATG-horse group.
The patients in the 2 groups were fully matched, at 10/10 loci (63% ATG-rabbit vs 54% for ATG-horse; P = .405). The graft source was mainly peripheral blood (92% vs 87%, respectively; P = .346). The ATG-rabbit group more often than the ATG-horse used a GVHD prophylaxis regimen consisting of tacrolimus and methotrexate (82% vs 46%, respectively; P <.0001). By contrast, the ATG-horse group used more cyclosporine and methotrexate (19% vs 2%, respectively; P = .003). The ATG-rabbit group received more CD34+ cells, at a median of 4.6 × 106 cells/kg compared with 3.3 × 106 cells/kg for ATG-horse (P = .031).
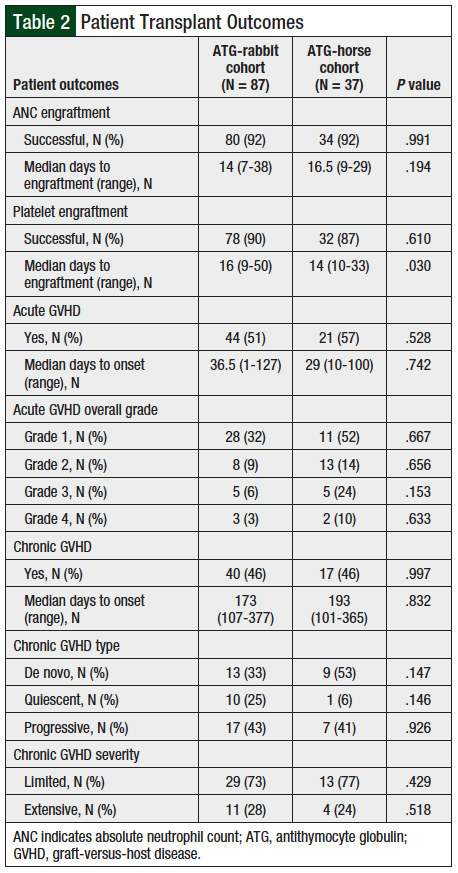
Transplant outcomes are listed in Table 2. Platelet engraftment was successful in 90% of cases in the ATG-rabbit group compared with 87% in the ATG-horse group (P = .610). The difference between median days to engraftment was significant, with ATG-horse having quicker engraftment (14 days vs 16.5 days with ATG-rabbit; P = .030). Acute GVHD was more common in the ATG-horse group (57%) compared with 51% with ATG-rabbit (P = .528). Comparison of acute GVHD severity grades 1 through 4 did not show significant differences.
The primary end point of chronic GVHD occurred in 40 (46%) patients in the ATG-rabbit group and 17 (46%) patients in the ATG-horse group (adjusted odds ratio, 0.983; 95% CI, 0.445-2.173). A 97.5% CI of –0.21 to 0.21 was calculated for the difference in population proportions. Confounding factors in the bivariate logistical regression included age, female donor/male recipient, and acute GVHD. The onset of chronic GVHD was a median of 173 days in the ATG-rabbit group and 193 days in the ATG-horse group (P = .832). No significant differences in chronic GVHD type and severity were observed between the 2 groups.
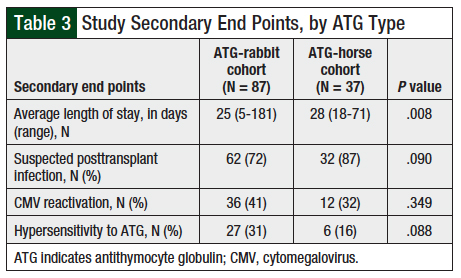
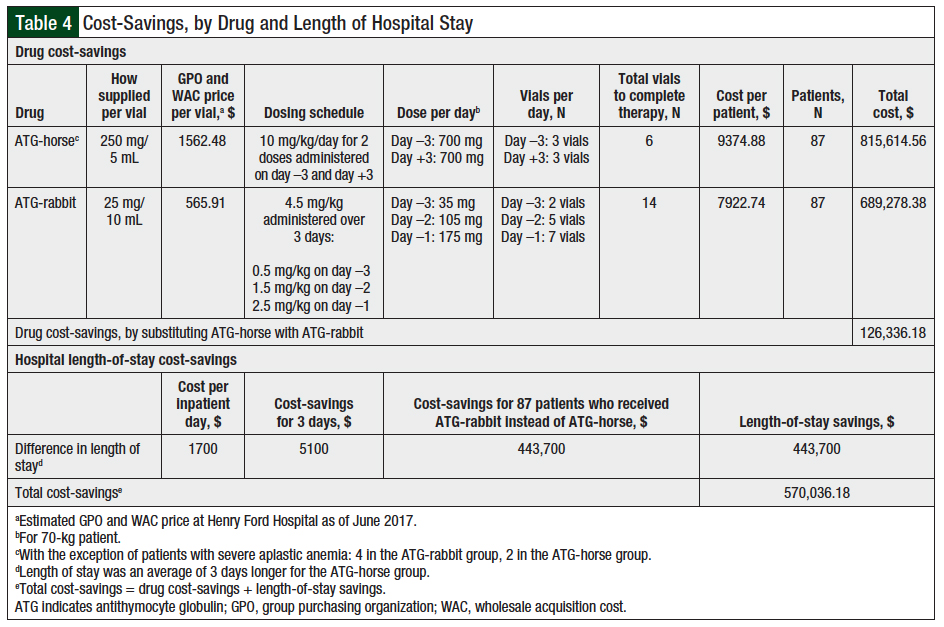
The results for the secondary end points are shown in Table 3. The 2 groups showed no differences in suspected posttransplant–related infection, CMV reactivation, and hypersensitivity reactions to ATG. However, in the ATG-rabbit group, the average length of hospital stay was shorter, at 25 days (range, 5-181 days) compared with 28 days in the ATG-horse group (range, 18-71 days; P = .008). Switching from ATG-horse to ATG-rabbit in 2011 resulted in substantial cost-savings, which are summarized in Table 4.
Between 2011 and 2015, 87 patients received an unrelated allogeneic bone marrow transplant at Henry Ford Hospital. The total cost using ATG-horse in 87 patients would be $815,614.56 compared with a total cost of $689,278.38 for ATG-rabbit in 87 patients, which equates to a $126,336.18 cost reduction. This is an estimation for a 70-kg patient, because both drugs are dosed based on weight. In addition, the estimated cost of 1 day of inpatient stay was $1700, and the cost avoidance of 3 fewer days of hospitalization for 87 patients was $443,700. The cumulative savings for 87 patients from 2011 to 2016 after switching between the 2 ATG agents is approximately $570,036.
Discussion
The study population was well-balanced between the 2 groups for baseline characteristics. The most common indications for transplant in the study population were AML, MDS, and ALL, which is reflective of indications for transplant worldwide.32 The majority of recipients were white, which is expected, because white patients in the United States have a higher likelihood than other ethnic groups of finding a well-matched patient donor and of undergoing the transplant process.17
GVHD prophylaxis regimens consist of a combination of immunosuppressive medications, including a calcineurin inhibitor (tacrolimus or cyclosporine) with methotrexate or mycophenolate mofetil for allogeneic transplants. ATG is added for unrelated donor transplants. As shown in Table 1, tacrolimus plus methotrexate was used more often (82%) in the ATG-rabbit group than in the ATG-horse group (46%; P <.0001). And cyclosporine plus methotrexate was more often used with ATG-horse (19%) compared with ATG-rabbit (2%; P = .003).
These significant differences reflect the changes in bone marrow transplant practice and a preferential use of tacrolimus over time. In the 1980s, cyclosporine was the only medication used to prevent GVHD.31 In later years, it was shown that adding low-dose methotrexate to cyclosporine reduces the incidence of acute and chronic GVHD.33
Yanada and colleagues compared tacrolimus plus methotrexate with cyclosporine plus methotrexate; they found that grade 2 to 4 acute GVHD in the unrelated donor HSCT population was higher with a cyclosporine-based regimen (57.8%) compared with a tacrolimus-based regimen (36.4%) at 100 days (P <.0001).34 Multivariate analysis confirmed a tacrolimus-based regimen reduced the risk for grade 2 to 4 acute GVHD. However, no significant difference was seen between the 2 groups for chronic GVHD (35% and 37.6%, respectively, at 3 years; P = .6618).34
Tacrolimus also offers the benefit of a favorable side-effects profile. It decreases the incidence of hirsutism and gingival hyperplasia that can be seen with cyclosporine.35 The decrease in acute GVHD incidence, which is a risk factor for chronic GVHD, and a better side-effects profile, show why tacrolimus plus methotrexate was more often used in conjunction with ATG-rabbit.
The results show that incidence of acute and chronic GVHD was similar between the ATG-horse and ATG-rabbit groups. Acute GVHD occurred in 50.6% and 56.8% (P = .528), respectively, with no significant differences in overall acute GVHD grades 1 to 4. Chronic GVHD occurred at 46% in both groups (P = .997). The median onset to chronic GVHD was 173 days (range, 107-377) in the ATG-rabbit group and 193 days (range, 101-365) in the ATG-horse group (P = .932). The type (de novo, quiescent, progressive) and severity (limited, extensive) were not significantly different between the ATG agents.
Our hypothesis was that ATG-rabbit is noninferior to ATG-horse in the context of chronic GVHD. We calculated a 97.5% CI of –0.21 to 0.21 for the difference in population proportions. Because this difference exceeds the prespecified noninferiority margin of 0.15, we were not able to reach the conclusion of noninferiority.
This study was not designed to show equality or inferiority; therefore, these other conclusions cannot be extrapolated from our findings. Nonetheless, previous studies, such as that of Walker and colleagues, showed that adding ATG-rabbit to a calcineurin inhibitor and methotrexate plus mycophenolate mofetil decreases the incidence of acute and of chronic GVHD.21 Other studies have shown the benefit of using ATG-rabbit for GVHD prevention.19,28,36 Therefore, the plan of Henry Ford Hospital is to continue using ATG-rabbit for bone marrow transplant, despite the lack of evidence for noninferiority of ATG-rabbit to ATG-horse in preventing chronic GVHD.
The time to engraftment was longer for platelets in the ATG-rabbit group, with a median of 16 days (range, 9-50) compared with a median of 14 days with ATG-horse (P = .030). Despite this, the overall average length of stay was shorter in the ATG-rabbit group, at 25 days (range, 5-181) compared with 28 days (range, 18-71; P = .008). From 2011 to 2016, the drug-related cost-savings seen by switching from ATG-horse to ATG-rabbit was $126,336.18. The decrease in hospital length of stay by 3 days saved a total of $443,700.
The overall 6-year cost-savings was $570,036.18 (roughly $95,000/year), or $6552.14 per patient. Several studies examining allogeneic transplant costs are from a single institution.37,38 As reported by Saito and colleagues, the median total costs from admission to 100 days posttransplant for an allogeneic transplant with related or unrelated donors was $102,575, at the Dana-Farber Cancer Institute/Brigham and Women’s Hospital, between the years 2000 and 2004.37 The median total cost from admission to 1 year posttransplant was $128,800.37
A more recent review of a single longitudinal administrative claims database by Majhail and colleagues reported a median cost of $203,026 for matched related and unrelated donor transplants from hospitalization through the first 100 days posttransplant.39
Published values may be an underestimation of the overall costs, because the estimated costs may not include the cost of resources to find a donor, mobilization of stem cells, the costs of long-term care, or the management of chronic GVHD and its complications.37,38 Factors that play into the variability of cost include stem-cell source and conditioning regimen intensity.38 The costs within the first 100 days posttransplant are mainly associated with the length of initial hospital stay.40 The decrease in the cost of an ATG and the length of inpatient stay decrease the burden of an already expensive process for allogeneic HSCT.
Limitations
This study includes a few notable limitations. First, the length of hospital stay of each patient is dependent on a multitude of factors, and the decrease in the length of hospital stay cannot be fully attributed to the change in the ATG agent alone. For example, improvements in antimicrobial prophylaxis, conditioning regimens, and provider practices over the past 10 years are key elements that can decrease a patient’s length of inpatient stay.
In addition, the Henry Ford Hospital in Detroit has several ongoing systemwide initiatives, including decreasing the inpatient length of stay, which might have contributed to the decrease in hospital stay seen in this study rather than the switching of ATG agents.
Furthermore, patient adherence to immunosuppressive medications after hospital discharge is important for preventing acute and chronic GVHD. The measurement of medication adherence through common methods, such as pill counting, however, was not possible, because this was a retrospective review. Another option would be to assess tacrolimus and cyclosporine levels, but we decided that the added benefit of evaluating lab values would decrease the applicability to real-life compliance.
Finally, patients might have received care outside of this single-center care after the transplant. As bone marrow transplant recipients, our patients are strongly encouraged to seek most, if not all, of their care at Henry Ford Hospital. In emergent cases that warrant immediate medical attention, however, it is possible that patients sought care elsewhere.
Conclusion
Based on our results, we were unable to conclude the noninferiority of ATG-rabbit to ATG-horse in preventing chronic GVHD. Nevertheless, previous studies have shown that adding ATG-rabbit to GVHD prophylaxis regimens helps to decrease the incidence of GVHD. With the 2 ATG formulations available to date, the elimination of the test dose during ATG-rabbit administration reduces extra steps for coordination and time. With a minimum of 3-day decrease in length of hospital stay, the overall cost-savings demonstrated in this study are notable. The operational and financial benefits shown here justify the continuing use of ATG-rabbit for patients undergoing allogeneic unrelated donor HSCT.
Author Disclosure Statement
Dr Lu, Dr Mikulandric, Dr Grycki, Dr Vogel, Dr Farhan, Dr Neme, Dr Peres, and Dr Janakiraman have no conflicts of interest to report .
References
- Socié G, Stone JV, Wingard JR, et al; for the Late Effects Working Committee of the International Bone Marrow Transplant Registry. Long-term survival and late deaths after allogeneic bone marrow transplantation. N Engl J Med. 1999;341:14-21.
- Porter DL, Antin JH. The graft-versus-leukemia effects of allogeneic cell therapy. Annu Rev Med. 1999;50:369-386.
- Lee SJ, Vogelsang G, Flowers MED. Chronic graft-versus-host disease. Biol Blood Marrow Transplant. 2003;9:215-233.
- Fraser CJ, Bhatia S, Ness K, et al. Impact of chronic graft-versus-host disease on the health status of hematopoietic cell transplantation survivors: a report from the Bone Marrow Transplant Survivor Study. Blood. 2006;108:2867-2873.
- Lee SJ. Classification systems for chronic graft-versus-host disease. Blood. 2017;129:30-37.
- Przepiorka D, Weisdorf D, Martin P, et al. 1994 Consensus Conference on Acute GVHD Grading. Bone Marrow Transplant. 1995;15:825-828.
- Shlomchik WD, Lee SJ, Couriel D, et al. Transplant’s greatest challenges: advances in chronic graft-versus-host disease. Biol Blood Marrow Transplant. 2007;13:2-10.
- Filipovich AH, Weisdorf D, Pavletic S, et al. National Institutes of Health Consensus Development Project on Criteria for Clinical Trials in Chronic Graft-Versus-Host Disease: I. Diagnosis and Staging Working Group Report. Biol Blood Marrow Transplant. 2005;11:945-956.
- Shulman HM, Cardona DM, Greenson JK, et al. NIH Consensus Development Project on Criteria for Clinical Trials in Chronic Graft-Versus-Host Disease: II. The 2014 Pathology Working Group Report. Biol Blood Marrow Transplant. 2015;21:589-603.
- Sanders JE. Chronic graft-versus-host disease and late effects after hematopoietic stem cell transplantation. Int J Hematol. 2002;76(suppl 2):15-28.
- Flowers MED, Parker PM, Johnston LJ, et al. Comparison of chronic graft-versus-host disease after transplantation of peripheral blood stem cells versus bone marrow in allogeneic recipients: long-term follow-up of a randomized trial. Blood. 2002;100:415-419.
- Lee SJ, Klein JP, Barrett AJ, et al. Severity of chronic graft-versus-host disease: association with treatment-related mortality and relapse. Blood. 2002;100:406-414.
- Stem Cell Trialists’ Collaborative Group. Allogeneic peripheral blood stem-cell compared with bone marrow transplantation in the management of hematologic malignancies: an individual patient data meta-analysis of nine randomized trials. J Clin Oncol. 2005;23:5074-5087.
- Passweg JR, Baldomero H, Bader P, et al; for the European Society for Blood and Marrow Transplantation. Hematopoietic SCT in Europe 2013: recent trends in the use of alternative donors showing more haploidentical donors but fewer cord blood transplants. Bone Marrow Transplant. 2015;50:476-482.
- Anasetti C, Logan BR, Lee SJ, et al; for the Blood and Marrow Transplant Clinical Trials Network. Peripheral-blood stem cells versus bone marrow from unrelated donors. N Engl J Med. 2012;367:1487-1496.
- Savani BN, Labopin M, Blaise D, et al. Peripheral blood stem cell graft compared to bone marrow after reduced intensity conditioning regimens for acute leukemia: a report from the ALWP of the EBMT. Haematologica. 2016;101:256-262.
- Dehn J, Arora M, Spellman S, et al. Unrelated donor hematopoietic cell transplantation: factors associated with a better HLA match. Biol Blood Marrow Transplant. 2008;14:1334-1340.
- Mohty M. Mechanisms of action of antithymocyte globulin: T-cell depletion and beyond. Leukemia. 2007;21:1387-1394.
- Ratanatharathorn V, Deol A, Ayash L, et al. Low-dose antithymocyte globulin enhanced the efficacy of tacrolimus and mycophenolate for GVHD prophylaxis in recipients of unrelated SCT. Bone Marrow Transplant. 2015;50:106-112.
- Kröger N, Solano C, Wolschke C, et al. Antilymphocyte globulin for prevention of chronic graft-versus-host disease. N Engl J Med. 2016;374:43-53.
- Walker I, Panzarella T, Couban S, et al; for the Canadian Blood and Marrow Transplant Group. Pretreatment with anti-thymocyte globulin versus no anti-thymocyte globulin in patients with haematological malignancies undergoing haemopoietic cell transplantation from unrelated donors: a randomised, controlled, open-label, phase 3, multicentre trial. Lancet Oncol. 2016;17:164-173. Erratum in: Lancet Oncol. 2016;17:164-173.
- Atgam (lymphocyte immune globulin, anti-thymocyte globulin [equine]), sterile solution for intravenous use only [prescribing information]. New York, NY: Pfizer; May 2018.
- Thymoglobulin (anti-thymocyte globulin [rabbit]) for injection, for intravenous use [prescribing information]. Cambridge, MA: Genzyme Corporation; April 2020.
- Feng X, Kajigaya S, Solomou EE, et al. Rabbit ATG but not horse ATG promotes expansion of functional CD4+CD25highFOXP3+ regulatory T cells in vitro. Blood. 2008;111:3675-3683.
- Shimony O, Nagler A, Gellman YN, et al. Anti-T lymphocyte globulin (ATG) induces generation of regulatory T cells, at least part of them express activated CD44. J Clin Immunol. 2012;32:173-188.
- Ehx G, Hannon M, Beguin Y, et al. Validation of a multicolor staining to monitor phosphoSTAT5 levels in regulatory T-cell subsets. Oncotarget. 2015;6:43255-43266.
- Baron F, Mohty M, Blaise D, et al. Anti-thymocyte globulin as graft-versus-host disease prevention in the setting of allogeneic peripheral blood stem cell transplantation: a review from the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation. Haematologica. 2017;102:224-234.
- Ravinet A, Cabrespine A, Socié G, et al. Impact of thymoglobulin by stem cell source (peripheral blood stem cell or bone marrow) after myeloablative stem cell transplantation from HLA 10/10-matched unrelated donors: a report from the Société Française de Greffe de Moelle et de Thérapie Cellulaire. Transplantation. 2016;100:1732-1739.
- National Cancer Institute. Common Terminology Criteria for Adverse Events (CTCAE). Version 4.03. June 14, 2010. www.eortc.be/services/doc/ctc/CTCAE_4.03_2010-06-14_QuickReference_5x7.pdf.
- Carlens S, Ringdén O, Remberger M, et al. Risk factors for chronic graft-versus-host disease after bone marrow transplantation: a retrospective single centre analysis. Bone Marrow Transplant. 1998;22:755-761.
- Flowers MED, Inamoto Y, Carpenter PA, et al. Comparative analysis of risk factors for acute graft-versus-host disease and for chronic graft-versus-host disease according to National Institutes of Health consensus criteria. Blood. 2011;117:3214-3219.
- D’Souza A, Fretham C, Lee SJ, et al. Current use of and trends in hematopoietic cell transplantation in the United States. Biol Blood Marrow Transplant. 2020 May 11:S1083-8791(20)30225-1, doi: 10.1016/j.bbmt.2020.04.013, PMID 3243804.
- Ringdén O, Horowitz MM, Sondel P, et al. Methotrexate, cyclosporine, or both to prevent graft-versus-host disease after HLA-identical sibling bone marrow transplants for early leukemia? Blood. 1993;81:1094-1101.
- Yanada M, Emi N, Naoe T, et al. Tacrolimus instead of cyclosporine used for prophylaxis against graft-versus-host disease improves outcome after hematopoietic stem cell transplantation from unrelated donors, but not from HLA-identical sibling donors: a nationwide survey conducted in Japan. Bone Marrow Transplant. 2004;34:331-337.
- Scott LJ, McKeague K, Keam SJ, et al. Tacrolimus: a further update of its use in the management of organ transplantation. Drugs. 2003;63:1247-1297.
- Schattenberg A, van der Meer A, Preijers F, et al. Addition of ATG to the conditioning regimen is a major determinant for outcome after transplantation with partially lymphocyte-depleted grafts from voluntary unrelated donors. Bone Marrow Transplant. 2004;33:1115-1121.
- Saito AM, Cutler C, Zahrieh D, et al. Costs of allogeneic hematopoietic cell transplantation with high-dose regimens. Biol Blood Marrow Transplant. 2008;14:197-207.
- Majhail NS, Mothukuri JM, Brunstein CG, Weisdorf DJ. Costs of hematopoietic cell transplantation: comparison of umbilical cord blood and matched related donor transplantation and the impact of posttransplant complications. Biol Blood Marrow Transplant. 2009;15:564-573.
- Majhail NS, Mau LW, Denzen EM, Arneson TJ. Costs of autologous and allogeneic hematopoietic cell transplantation in the United States: a study using a large National Private Claims Database. Bone Marrow Transplant. 2013;48:294-300.
- Preussler JM, Denzen EM, Majhail NS. Costs and cost-effectiveness of hematopoietic cell transplantation. Biol Blood Marrow Transplant. 2012;18:1620-1628.