| This section provides a quick update of symptomatic conditions in oncology and their management. Readers are invited to submit brief updates following the guidelines provided at the end of the article. |
Symptom Overview
Hyperuricemia is a complication commonly associated with tumor lysis syndrome (TLS) in patients with hematologic cancers. It is characterized by an increased serum uric acid concentration driven by the purine catabolism pathway, which converts purine nucleic acids to hypoxanthine, to xanthine, and then to uric acid via the xanthine oxidase enzyme.1 In the context of TLS, hyperuricemia is defined as a uric acid level ≥8 mg/dL, based on Cairo and Bishop’s laboratory criteria.2 Accumulation can result in uric acid crystal precipitation in the renal tubules, leading to renal damage and potential renal failure.
Etiology
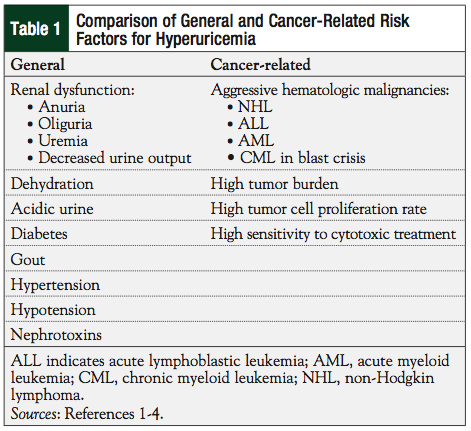
Hyperuricemia occurs most commonly in patients with aggressive hematologic malignancies that have ≥1 of the following characteristics: a high tumor burden; a rapid rate of proliferation; or are more sensitive to cytotoxic treatment.1,3 As an important component of TLS, hyperuricemia is most frequently seen in patients with high-grade, non-Hodgkin lymphomas, especially Burkitt lymphoma, and other aggressive hematologic disorders, including acute lymphoblastic leukemia and acute myeloid leukemia. In addition to cancer-related causes, which can result in spontaneous versus treatment-related TLS, the associated hyperuricemia can be exacerbated by underlying renal dysfunction, dehydration, or other comorbidities outlined in Table 1.1-4
Treatment Options
Treatment is focused on prophylaxes, and prevention of the hyperuricemic component of TLS.
Aggressive fluid hydration is essential to increase urine output and promote uric acid excretion. Intravenous (IV) fluid infusion rates should be sufficient to maintain urine output at >100 mL/hr (or 3 mL/kg/hour in children weighing <10 kg); up to 3 L/m2 is recommended for adult patients with high risk of TLS.3,4 Selection of fluids and initial rates should be guided by the cardiovascular status of the patient,3 and clinical assessment of patient-specific factors. Use of sodium bicarbonate for urine alkalinization is no longer recommended in light of studies showing that alkalinization may be ineffective in preventing uric acid nephropathy,3,5 contribute to acute kidney injury,3,6 and increase risk of precipitation of xanthine crystals in renal tubules when used in patients receiving allopurinol.1
Allopurinol is considered a mainstay for preventing hyperuricemia associated with TLS.3 Allopurinol works as a competitive xanthine oxidase inhibitor, effectively blocking the conversion of hypoxanthine and xanthine to uric acid.1,3 Allopurinol is available both orally and intravenously. Although the efficacy of the IV formulation is equivalent to that of the oral formulation, oral dosing is preferred in most cases for cost considerations. Use of IV allopurinol should be restricted to patients who are unable to tolerate oral medications.1 In adults, allopurinol is given as a load of 600 to 800 mg orally per day in divided doses starting 12 to 48 hours prior to initiating cytotoxic therapy,3 followed by 300 mg orally once daily throughout active treatment and until uric acid levels and all other TLS laboratory values have normalized.3 IV dosing of allopurinol in adults is 200 to 400 mg/m2 (maximum 600 mg daily) either once daily or in divided doses 2 to 3 times daily. Most of the evidence recommending renal dose adjustments for allopurinol originates from the chronic treatment of gout, where a dose reduction of 50% may be recommended in patients with renal insufficiency.1 However, it is unclear whether renal adjustment is required in the short-term treatment of acute TLS.7 Allopurinol primarily works to prevent further production of uric acid; however, it is unable to break down preexisting uric acid.3 When given concurrently with IV hydration, allopurinol prophylaxis is preferred for at least 1 to 2 days prior to initiation of chemotherapy to allow for excretion of existing uric acid loads.3 This pretherapy treatment may not be possible, depending on tumor kinetics (which may require urgent therapy for other clinical indications).
Febuxostat, a selective xanthine oxidase inhibitor, may be a suitable antihyperuricemic alternative to allopurinol.8 Although it is rare, hypersensitivity reactions are associated with allopurinol, and renally impaired patients may be at an increased risk.7 Febuxostat is associated with fewer hypersensitivity reactions, and does not require renal adjustment,8 so it may provide an alternative for patients who have known hypersensitivity to allopurinol. Febuxostat is currently indicated for the management of gout-associated hyperuricemia; however, recent studies suggest its potential usefulness in the context of TLS.9 Febuxostat doses of 40 to 60 mg daily successfully lowered uric acid levels in a single-institution study of Japanese patients with cancer managed for intermediate-risk TLS. Another single-institution, retrospective study of Japanese patients with cancer at risk for TLS showed no significant difference between 300 mg daily of allopurinol and 40 mg daily of febuxostat in lowering uric acid levels.10
Finally, rasburicase, a recombinant urate oxidase enzyme, promotes the conversion of uric acid to the inactive soluble metabolite allantoin.1 Although it is very effective in reducing uric acid levels, rasburicase is typically reserved—because of its high cost—for treatment of patients who have already developed hyperuricemia with TLS, or as prophylaxis for high-risk individuals.1 Rasburicase is considered the therapy of choice for hyperuricemia despite prophylactic allopurinol use. Recommended IV dosing for rasburicase is 0.1 to 0.2 mg/kg once daily with treatment duration ranging from 1 to 7 days1,3; however, there is growing evidence supporting the safe and effective use of single-dose and fixed-dose rasburicase as a potential cost-saving strategy. Most of the data for single-dose rasburicase are retrospective reviews based on single-institution experiences using fixed doses of rasburicase ranging from 1.5 to 7.5 mg,11-13 and 1 prospective study using a historical control group.14 Repeat doses may be given based on continued serum uric acid level monitoring.11,12
Rasburicase is relatively fast-acting, with a decrease in uric acid levels observed within 4 hours of administration.14 Rasburicase is contraindicated in patients with a known glucose-6-phosphate dehydrogenase deficiency because of an increased risk for hemolysis.15 Serious adverse reactions to rasburicase are rare, but include hypersensitivity reactions (eg, anaphylaxis), hemolysis, and methemoglobinemia. Of clinical importance, rasburicase causes continued ex vivo enzymatic degradation of uric acid in blood samples kept at room temperature, leading to falsely low uric acid measurements. Blood samples should be placed in chilled tubes with a heparin anticoagulant, immersed immediately in an ice water bath, and assayed within 4 hours of collection to ensure accurate results.15
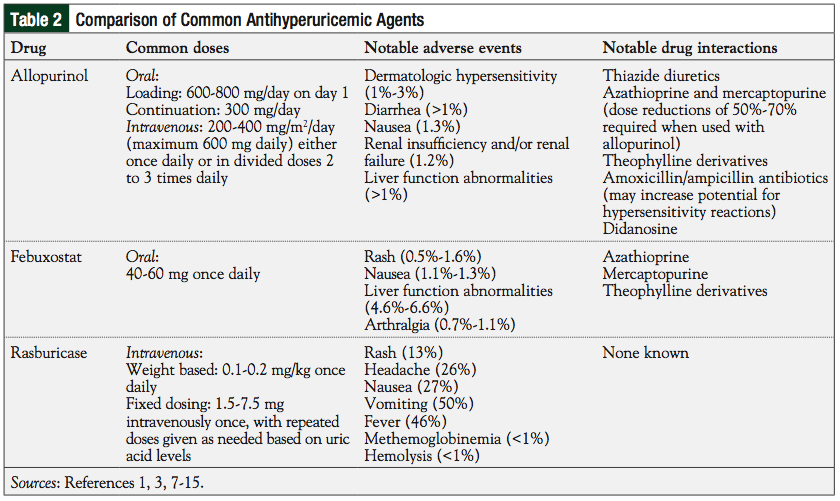
Allopurinol and rasburicase may be used concomitantly to optimize treatment of TLS, with allopurinol preventing formation of new uric acid, and rasburicase eliminating the existing uric acid load. For a comparison of common antihyperuricemic agents, see Table 2.1,3,7-15
In summation, patients with highly aggressive hematologic cancers are at an increased risk for hyperuricemia as part of their clinical course. The best form of treatment remains prevention of hyperuricemia with aggressive fluids and allopurinol. Rasburicase is an option for patients at high risk for hyperuricemia, or for patients with clinically significant hyperuricemia.
Dr Diaz is Oncology Clinical Pharmacy Specialist, Oregon Health and Science University Hospital, OHSU Hospital and Clinics, Portland; and Dr Bubalo is Assistant Professor of Medicine, Division of Hematology and Medical Oncology, Oncology Clinical Pharmacy Specialist, Oregon Health and Science University Hospital, OHSU Hospital and Clinics, Portland, OR.
References
1. Coiffier B, Altman A, Pui CH, et al. Guidelines for the management of pediatric and adult tumor lysis syndrome: an evidence-based review. J Clin Oncol. 2008;26: 2767-2778.
2. Cairo MS, Bishop M. Tumour lysis syndrome: new therapeutic strategies and classification. Br J Haematol. 2004;127:3-11.
3. Mughal TI, Ejaz AA, Foringer JR, et al. An integrated clinical approach for the identification, prevention, and treatment of tumor lysis syndrome. Cancer Treat Rev. 2010;36:164-176.
4. Tosi P, Barosi G, Lazzaro C, et al. Consensus conference on the management of tumor lysis syndrome. Haematologica. 2008;93:1877-1885.
5. Conger JD, Falk SA. Intrarenal dynamics in the pathogenesis and prevention of acute urate nephropathy. J Clin Invest. 1977;59:786-793.
6. Ten Harkel AD, Kist-Van Holthe JE, Van Weel M, et al. Alkalinization and the tumor lysis syndrome. Med Pediatr Oncol. 1998;31:27-28.
7. Allopurinol tablet [package insert]. Huntsville, AL: Qualitest Pharmaceuticals; 2012.
8. Uloric (febuxostat) tablet [package insert]. Deerfield, IL: Takeda Pharmaceuticals America, Inc; 2013.
9. Takai M, Yamauchi T, Ookura M, et al. Febuxostat for management of tumor lysis syndrome including its effects on levels of purine metabolites in patients with hematological malignancies - a single institution’s, pharmacokinetic and pilot prospective study. Anticancer Res. 2014;34:7287-7296.
10. Maie K, Yokoyama Y, Kurita N, et al. Hypouricemic effect and safety of febuxostat used for prevention of tumor lysis syndrome. Springerplus. 2014;3:501.
11. Clemmons AB, Ensley E, Hoge S, et al. Fixed-dose rasburicase in overweight and obese patients versus normal-weight patients. Ann Pharmacother. 2014;48:1152-1158.
12. Herrington JD, Dinh BC. Fixed, low-dose rasburicase for the treatment or prevention of hyperuricemia in adult oncology patients. J Oncol Pharm Pract. 2015;21: 111-117.
13. McBride A, Lathon SC, Boehmer L, et al. Comparative evaluation of single fixed dosing and weight-based dosing of rasburicase for tumor lysis syndrome. Pharmacotherapy. 2013;33:295-303.
14. Reeves DJ, Bestul DJ. Evaluation of a single fixed dose of rasburicase 7.5 mg for the treatment of hyperuricemia in adults with cancer. Pharmacotherapy. 2008;28: 685-690.
15. Elitek (rasburicase) powder for solution, for intravenous infusion [package insert]. Bridgewater, NJ: sanofi-aventis U.S. LLC; 2011.
Submit Your Symptom Management Update
Readers are invited to submit brief updates with practice insights on the care of a specific symptom or a cluster of symptoms associated with a condition that is often seen in patients with cancer. The updates will be presented in the form of a “How I Treat” type of article.
The goal of this section is to present a quick background to enhance providers’ understanding of the symptoms associated with a specific condition and their characteristic presentation(s) and etiology. The emphasis should be on a concise description of available treatments and current course of therapy.
How to Submit
Submit a Word file of your article at www.JHOPonline.com.