Pancreatic cancer is relatively common, but only approximately 9% of pancreatic cancers are considered localized at diagnosis and survival outcomes are suboptimal, with a relative 5-year survival rate of approximately 40%.1,2 Surgical resection remains the only cure for pancreatic cancer, which is only possible for patients with localized disease and without significant vascular involvement.3,4
Pancreatic tumors that are considered to be borderline resectable may warrant neoadjuvant therapy to shrink the tumor for surgical intervention, with the goal of cure.5 Neoadjuvant therapy is also recommended by the National Comprehensive Cancer Network (NCCN) for patients with high-risk clinical and laboratory features to promote successful resection.5
The value of neoadjuvant therapy in this context is continuing to be studied, and the recommended regimens are based on limited evidence. The NCCN’s guidelines recommend consultation at a high-volume center with a multidisciplinary team that includes surgeons, diagnostic imaging, interventional endoscopy, medical and radiation oncologists, pathology, and palliative care.5
One frequently used regimen for the neoadjuvant treatment of pancreatic cancer is FOLFIRINOX, which combines the cytotoxic agents 5-fluorouracil, irinotecan, and oxaliplatin.5 According to a meta-analysis review of clinical trials examining the use of neoadjuvant FOLFIRINOX therapy for patients with pancreatic cancer, an estimated 68% of patients with borderline resectable disease will successfully undergo resection after 4 to 9 cycles of neoadjuvant FOLFIRINOX, with each cycle administered every 14 days.6
The use of chemotherapy in patients with cancer and renal impairment, especially in those with end-stage renal disease (ESRD), presents clinicians with multiple issues to consider.7 The clearance of medications depends heavily on nonrenal elimination and the ability of hemodialysis to clear serum concentrations of the drug.7 A careful review of the literature and an evaluation of each agent’s pharmacokinetics should be performed before the administration of chemotherapy in patients with ESRD.
Improper dose adjustments or administration of chemotherapy in relation to hemodialysis can lead to drug accumulation, increased drug exposure, and the downstream exacerbation of adverse events. Several adverse events are of particular concern with FOLFIRINOX, including oxaliplatin-induced peripheral neuropathy and cholinergic effects caused by irinotecan treatment that can lead to gastrointestinal (GI) disturbances, mainly diarrhea.8-12
In addition, myelosuppression associated with FOLFIRINOX treatment could theoretically be more profound, with longer exposure secondary to poor renal clearance.8-10 Although patients with renal impairment are rarely represented in clinical trials, standard clinical practice necessitates further guidance about dosing to advise on the best treatment options for this high-risk patient population.
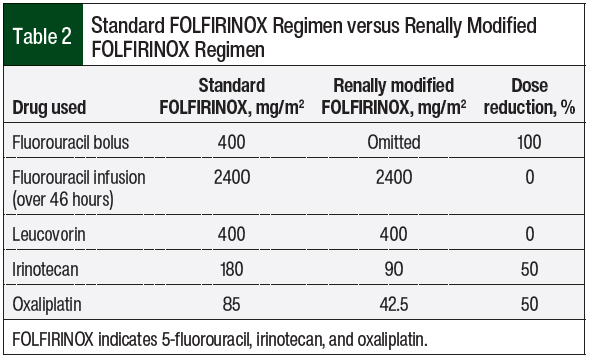
The collection of pharmacokinetic data on each agent is crucial for proper assessment of and adjustments for a multi-agent regimen in patients receiving hemodialysis. The dosing of FOLFIRINOX in a patient with normal organ function includes oxaliplatin 85 mg/m2 over 2 hours, leucovorin 400 mg/m2 over 2 hours, irinotecan 180 mg/m2 over 90 minutes, fluorouracil 400 mg/m2 intravenous (IV) bolus, and fluorouracil 2400 mg/m2 IV as a continuous infusion over 46 hours.6
With the FOLFIRINOX regimen, renal elimination clearance accounts for 54% of oxaliplatin, 20% of irinotecan, 3% of irinotecan’s metabolites, and negligible amounts of fluorouracil.10,11,13-16 As reported in multiple case reports, oxaliplatin was administered with a significant dose reduction of approximately 50%, and hemodialysis was performed within approximately 1 hour or immediately after oxaliplatin administration.12,17-22
Irinotecan has been tolerable in doses between 50 mg/m2 and 80 mg/m2 in several cases of patients with cancer who were receiving intermittent hemodialysis.13,23,24 In these cases, irinotecan was administered immediately after dialysis, and adverse events, such as diarrhea, were managed with supportive care.13,23,24
Fluorouracil is predominantly metabolized by the liver, with corresponding dose adjustment based on hepatic function, and it has been used safely without dose adjustments in patients who were receiving intermittent hemodialysis.14-16 In these cases, fluorouracil was administered after hemodialysis.14-16
The long administration time of fluorouracil via infusion pump may pose a concern during subsequent dialysis sessions, because fluorouracil is dialyzable, leading to the possibility of decreased exposure and a potential effect on the drug’s efficacy.16 Overall, there are significant clinical and logistic considerations when administering the FOLFIRINOX regimen to a patient with ESRD.
Case Report
In June 2020, a 65-year-old man presented to Fred Hutch Cancer Center in Seattle with new-onset severe pruritus and diarrhea associated with jaundice that started 5 days earlier. He had a notable history of hypertension and ESRD secondary to hypertension, which required hemodialysis 3 times weekly. A computed tomography (CT) showed biliary obstruction that was corrected with stenting, and a fine-needle aspirate confirmed the diagnosis of pancreatic ductal adenocarcinoma.
A tumor board interdisciplinary team of medical oncologists, surgeons, and pharmacists ultimately determined that the patient’s pancreatic cancer was borderline resectable. The decision was made to administer neoadjuvant FOLFIRINOX therapy every 2 weeks for 4 to 6 months, with the goal of decreasing the tumor size to allow for resection, with a curative intent.
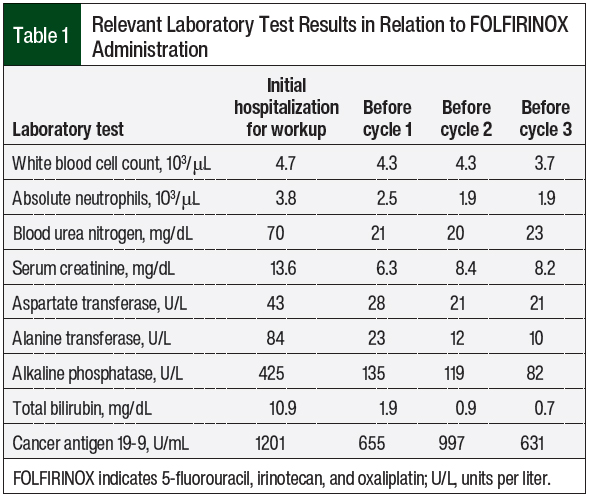
The patient’s renal status and dialysis schedule, however, posed clinical and logistic challenges for safe and effective treatment. The relevant laboratory findings on day 1 of his admission for workup and before cycle 1 of FOLFIRINOX included blood urea nitrogen of 21 mg/dL and serum creatinine of 6.3 mg/dL (Table 1).
No hepatic dose adjustments were made, because the patient’s liver transaminases and bilirubin normalized after stent placement. For his first cycle, renally adjusted FOLFIRINOX dosing was administered 24 hours before dialysis, and the fluorouracil pump was disconnected before traveling to dialysis. Oxaliplatin was administered intravenously at 42.5 mg/m2, representing a 50% dose reduction. Oxaliplatin was administered over 42.5 minutes (1 mg/m2/min) during cycle 1 to allow increased time for exposure to fluorouracil.25
Although various case reports suggest performing hemodialysis immediately after treatment with oxaliplatin,12,17-22,26 this was not the case in our patient because of his preference and a concern about his complex schedule and transportation. Irinotecan was administered at a dose of 90 mg/m2, representing a 50% dose reduction, over 55 minutes to allow for an earlier fluorouracil pump start.27 Fluorouracil was administered as a continuous infusion at a dose of 2400 mg/m2 over 46 hours, and dialysis was performed immediately after.
To evaluate the patient’s tolerance of fluorouracil and to facilitate his travel to hemodialysis, the fluorouracil infusion was administered for only 24 hours, and half of the dose was administered during cycle 1. Fluorouracil was increased to the full dose and infusion time during subsequent infusions. Fluorouracil bolus was omitted, based on our institutional practice.
Premedication antiemetic drugs included palonosetron, aprepitant, and dexamethasone. Prophylactic atropine was administered for the prevention of acute cholinergic symptoms.
The patient’s take-home prescription medications included loperamide, ondansetron, and prochlorperazine. No growth factor support was administered. Table 2 presents a comparison of renally modified FOLFIRINOX dosing and standard-dose FOLFIRINOX regimen.
After the first cycle of chemotherapy, the patient was hospitalized twice. The first hospitalization was 3 days after chemotherapy administration and was unrelated to his chemotherapy, malignancy, or comorbid conditions. The second hospitalization was 15 days after chemotherapy administration because of grade 3 nausea and vomiting, in accordance with the Common Terminology Criteria for Adverse Events version 5.0.28 Of note, the patient’s absolute neutrophil count nadir during the second hospitalization was 1.9 × 103/μL, without growth factor support.
Chemotherapy cycle 2 was delayed by 1 week because of the patient’s previous hospitalization and adverse events. In contrast to cycle 1, all agents were administered 48 hours before dialysis at standard rates to allow for the full administration of fluorouracil. Although oxaliplatin and irinotecan were maintained at the 50% dose reduction, oxaliplatin was infused over the standard 120 minutes, and irinotecan was infused over the standard 90 minutes. At the completion of fluorouracil treatment, the patient reported intermittent grade 2 nausea and grade 2 shortness of breath.
The patient was hospitalized on day 7 of cycle 2, with complaints of grade 3 shortness of breath lasting 3 days before admission, grade 3 diarrhea that started after the completion of fluorouracil administration, and abdominal pain. A cardiac workup showed elevated troponin without myocardial ischemia. The patient’s platelet and absolute neutrophil counts were within normal limits. His total bilirubin was elevated at 1.5 mg/dL, his aspartate transaminase was 1.2 times the upper limit of normal (ULN), and his alanine transaminase was 2.1 times the ULN.
A blood culture showed Escherichia coli bacteremia, which was treated with IV antibiotics. A new biliary stent was placed for concerns of biliary occlusion leading to the bacteremia. At the time of discharge, the patient’s pain was manageable and his diarrhea resolved.
Cycle 3 was administered on schedule, using the same infusion time and doses from cycle 2. On administration of the chemotherapy, the patient reported pain corresponding to his baseline pain. At the end of the fluorouracil infusion, the patient reported grade 3 nausea requiring IV fluids because of volume depletion secondary to poor oral fluid intake.
The patient was subsequently admitted to the hospital 15 days after chemotherapy (when he was due to receive treatment cycle 4) for complaints of grade 3 nausea and vomiting, diarrhea, and abdominal pain. The medical team was unsure of the patient’s adherence to his antidiarrheal and antiemetic medications at home. The team suspected that he was not scheduling his medications optimally and was not using the proper strength of his medications. During his hospital admission, the medical team optimized the patient’s antipain regimen and treated his diarrhea, vomiting, and nausea.
Additional treatment with the FOLFIRINOX regimen was discontinued based on the patient’s wishes because of intolerable adverse events. A follow-up CT showed stable disease with tumor encasement of the hepatic artery, which was determined to be unresectable. At a multidisciplinary tumor board the team decided to forego chemotherapy because of the lack of response to and intolerance of the regimen. The patient proceeded to radiation treatment, with a plan for surgical resection if radiation was successful. After radiation, further imaging showed disease progression and the patient was prescribed subsequent-line therapy with gemcitabine and nab-paclitaxel.
Discussion
Because our patient had multiple hospitalizations, modifications of the FOLFIRINOX regimen could have been further optimized with additional dose adjustments and supportive care measures for better therapy toleration.
The major adverse events with FOLFIRINOX regimen in our patient were nausea, vomiting, and diarrhea, which was likely largely attributable to irinotecan and was therefore empirically reduced to 90 mg/m2, a 50% reduction of the drug’s standard use.29
Vénat-Bouvet and colleagues presented 2 cases of patients with metastatic colorectal cancer who were undergoing hemodialysis and received 14-day cycles of the FOLFIRI (irinotecan, leucovorin, and 5-fluorouracil) regimen, with one patient receiving an empiric dose decrease of irinotecan 125 mg/m2 and the other patient receiving a standard dose of irinotecan 180 mg/m2; both doses led to hematologic adverse events, sepsis, and subsequent death.30
Other case reports have shown the safe use of weekly irinotecan doses between 50 and 80 mg/m2, in combination or as monotherapy, in patients undergoing hemodialysis.9,23,24,31
In our patient, irinotecan was dosed lower than in the cases described by Vénat-Bouvet and colleagues and higher than in other case reports,9,23,24,30,31 with the goal of maximizing the likelihood of a response, to allow for surgical resection. With further optimization of the chemotherapy doses, our patient’s adverse events might have been mitigated. His intolerable side effects may suggest that a lower dosing strategy is advisable in hemodialysis patients.
Previous case reports and our patient case suggest that irinotecan administered every 2 weeks may be initiated at a dose of 50 mg/m2, uptitrated based on tolerability and capped at 80 mg/m2. The final dosing decision should depend on a variety of patient-specific clinical factors. In our patient, irinotecan was likely the driver of treatment intolerance, notably diarrhea and emetogenicity.11,32
The safety and efficacy data regarding treatment with oxaliplatin are limited in patients with cancer who are dependent on hemodialysis.33 Watayo and colleagues reported the tolerability and pharmacokinetics of FOLFOX6 treatment regimen in a patient with rectal cancer who was receiving hemodialysis.17 The patient had grade 2 leukopenia, neutropenia, and thrombocytopenia during the fifth treatment cycle. No other intolerabilities were reported. He received a total of 11 treatment cycles and had no peripheral neuropathy.17
Wang and colleagues described a patient with colorectal cancer who required intermittent hemodialysis and received FOLFOX treatment every 3 weeks.18 That patient received oxaliplatin every 3 weeks at a starting dose of 50 mg/m2 before dialysis, which was escalated to the full dose of 85 mg/m2 using dose increases of 10 mg/m2 in cycles 2 and 3, without peripheral neuropathy.18
In these 2 cases, the patients underwent hemodialysis immediately after or 1 hour after oxaliplatin administration,17,18 because this would be the major route of clearance of oxaliplatin. Based on these 2 cases, oxaliplatin can be safely administered to patients who are undergoing intermittent hemodialysis; hemodialysis removes >80% of oxaliplatin.17,18 Thus, it is recommended that oxaliplatin be administered after a hemodialysis session or on the day the patient is not undergoing hemodialysis, to maximize efficacy.33
Our patient did not have hemodialysis immediately after or 1 hour after the oxaliplatin administration, because coordinating infusions at one institution and dialysis at another was not feasible, and the decision to forego immediate dialysis was driven mainly by the patient’s preferences.
The oncology team administered oxaliplatin treatment at 50% of the standard dosing, with dialysis occurring 24 hours after oxaliplatin administration during the first cycle, and 46 hours after administration on subsequent cycles. During the first cycle, we administered oxaliplatin at a rate of 1 mg/m2/min, because of the logistics with hemodialysis; this decision was based on a retrospective review of more than 600 patients that showed no increase in hypersensitivity in patients who received a faster chemotherapy infusion.25
Oxaliplatin might have confounded the causative agent of emetogenicity; however, the medical team believed that the symptoms were caused by the treatment with irinotecan. Treatment with oxaliplatin can be administered safely at a 50% dose reduction without the need for hemodialysis immediately after receiving therapy in the neoadjuvant setting.
Fluorouracil is primarily metabolized hepatically, with renal elimination accounting for <10% of excretion.8 In our patient, the fluorouracil bolus was omitted to reduce the risks for severe myelosuppression, fatigue, and vomiting.34 Fluorouracil has been safely administered to patients undergoing hemodialysis without dose adjustments14-16; thus, we felt comfortable in administering fluorouracil at a standard dose in our patient.
Our patient had an acceptable recovery of all blood counts (Table 1) and had no hematologic adverse events. In addition, the patient did not have hand-foot syndrome, which is associated with continuous fluorouracil treatment.35
Diarrhea was reported by our patient on pump disconnecting, and hospitalizations secondary to adverse events might have resulted from poor antidiarrhea management at home. During the first cycle, only half of the fluorouracil dose was infused to allow for the monitoring of toleration to fluorouracil and to accommodate for the patient’s preference, because he had to travel to his dialysis session. Continuous-infusion fluorouracil can be administered at the full dose safely in a patient undergoing hemodialysis.
Our patient had frequent hospitalizations during the course of chemotherapy that could have been related to chemotherapy or to his other chronic medical conditions, such as pain or underlying malignancy, which ultimately led to the discontinuation of chemotherapy. With pain optimization, these admissions were likely secondary to his acute or chronic cancer pains.
The medical team extended the time between chemotherapy administration and undergoing dialysis to 46 hours to allow for longer exposure to the chemotherapy agents. Compared with the shortened treatment cycle, our patient reported more fatigue and nausea during subsequent treatment cycles, which was likely the result of being exposed to full-dose fluorouracil. Overall, renally modified FOLFIRINOX regimen was feasible in coordination with the dialysis sessions, and further modifications might have improved the tolerability.
The team used a multidisciplinary approach to formulate a chemotherapy plan that was safe, effective, and feasible. Predetermined dose reductions were based on literature review by the GI oncology pharmacy team. Our infusion center does not have a dialysis unit, and patients must travel to a third-party dialysis center.
In addition, the outside dialysis center would not dialyze a patient with an active continuous chemotherapy infusion, because of safety concerns. This posed a logistical obstacle to schedule the chemotherapy administration and continuous infusion pump disconnect to optimize exposure to these agents. The first cycle’s truncated chemotherapy administration was because of logistics and patient monitoring. Dialysis occurred 3 times weekly, and having a truncated exposure allowed the medical team to assess the patient’s tolerance before proceeding to a 48-hour exposure time to a modified FOLFIRINOX regimen.
Conclusion
Our case demonstrates how neoadjuvant treatment with renally modified FOLFIRINOX regimen for borderline resectable pancreatic cancer can be administered 48 hours before dialysis. The patient’s stable disease after receiving the renally modified FOLFIRINOX regimen and the subsequent nonresponse to radiation likely signify poor tumor biology.
This case also suggests areas for improvement in the management of adverse events. The GI adverse events associated with irinotecan could have been better managed with a greater dose reduction and optimization of home antidiarrheal medications, although this has the potential downside of a further reduction in efficacy. No hematologic adverse events were seen throughout our patient’s treatment, and his recurrent chronic pain further complicated the clinical picture. Optimization of the multi-agent chemotherapy plan was essential in the context of hemodialysis at an offsite dialysis center.
Finally, this case report highlights the multiple considerations needed for a patient undergoing hemodialysis. We recommend that irinotecan treatment be administered at 50 mg/m2 and maintaining the same doses for the other agents. Furthermore, oxaliplatin 42.5 mg/m2 (50% regimen dosing) could be safely administered, with no immediate hemodialysis. Fluorouracil can be used safely in a patient with ESRD, because it is predominantly metabolized hepatically. This chemotherapy treatment plan can be used to guide the dosing of FOLFIRINOX regimen in patients with cancer and ESRD who are undergoing hemodialysis.
Author Disclosure Statement
Dr Cohen is on the Advisory Board of Pfizer; Dr Lee, Dr Jao, Dr Jeong, Dr Nakagawa, and Dr Segal have no conflicts of interest to report.
References
- Saad AM, Turk T, Al-Husseini MJ, Abdel-Rahman O. Trends in pancreatic adenocarcinoma incidence and mortality in the United States in the last four decades; a SEER-based study. BMC Cancer. 2018;18:688. doi: 10.1186/s12885-018-4610-4.
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70:7-30.
- McGuigan A, Kelly P, Turkington RC, et al. Pancreatic cancer: a review of clinical diagnosis, epidemiology, treatment and outcomes. World J Gastroenterol. 2018;24:4846-4861.
- Grossberg AJ, Chu LC, Deig CR, et al. Multidisciplinary standards of care and recent progress in pancreatic ductal adenocarcinoma. CA Cancer J Clin. 2020;70:375-403.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines): Pancreatic Adenocarcinoma. Version 1.2022. February 24, 2022. www.nccn.org/professionals/physician_gls/pdf/pancreatic.pdf. Accessed November 28, 2022.
- Conroy T, Hammel P, Hebbar M, et al; for the Canadian Cancer Trials Group and the Unicancer-GI–PRODIGE Group. FOLFIRINOX or gemcitabine as adjuvant therapy for pancreatic cancer. N Engl J Med. 2018;379:2395-2406.
- Launay-Vacher V. Epidemiology of chronic kidney disease in cancer patients: lessons from the IRMA study group. Semin Nephrol. 2010;30:548-556.
- Iyer L, Ratain MJ. 5-fluorouracil pharmacokinetics: causes for variability and strategies for modulation in cancer chemotherapy. Cancer Invest. 1999;17:494-506.
- Czock D, Rasche FM, Boesler B, et al. Irinotecan in cancer patients with end-stage renal failure. Ann Pharmacother. 2009;43:363-369.
- Oxaliplatin injection, for intravenous use [prescribing information]. Teva Pharmaceuticals; January 2020. https://dailymed.nlm.nih.gov/dailymed/fda/fdaDrugXsl.cfm?setid=9e51cc79-620c-48d7-b267-78e43c1ef6e4&type=display. Accessed June 18, 2021.
- Camptosar (irinotecan hydrochloride) injection, for intravenous use [prescribing information]. Pfizer; February 2022. https://labeling.pfizer.com/ShowLabeling.aspx?id=533. Accessed November 28, 2022.
- Katsumata K, Sumi T, Wada T, et al. Oxaliplatin for metastatic colon cancer in a patient with renal failure. Clin Med Oncol. 2008;2:97-101.
- Ashizawa T, Iwahori T, Yokoyama T, et al. Irinotecan hydrochloride (CPT-11) in dialysis patients with gastrointestinal cancer. Acta Med Okayama. 2010;64:19-26.
- Tanriverdi O, Ogunc H. A case report of three patients with metastatic gastric cancer on hemodialysis who were treated with cisplatin–fluorouracil regimen. J Oncol Pharm Pract. 2016;22:345-349.
- Rengelshausen J, Hull WE, Schwenger V, et al. Pharmacokinetics of 5-fluorouracil and its catabolites determined by 19F nuclear magnetic resonance spectroscopy for a patient on chronic hemodialysis. Am J Kidney Dis. 2002;39:E10. doi: 10.1053/ajkd.2002.30584.
- Gusella M, Rebeschini M, Cartei G, et al. Effect of hemodialysis on the metabolic clearance of 5-fluorouracil in a patient with end-stage renal failure. Ther Drug Monit. 2005;27:816-818.
- Watayo Y, Kuramochi H, Hayashi K, et al. Drug monitoring during FOLFOX6 therapy in a rectal cancer patient on chronic hemodialysis. Jpn J Clin Oncol. 2010;40:360-364.
- Wang D, Li X, Xu L, et al. Dose-escalation of oxaliplatin in hemodialysis patient treated with FOLFOX therapy: a case report. Medicine (Baltimore). 2019;98:e17462. doi: 10.1097/MD.0000000000017462.
- Sasaki K, Zhou Q, Matsumoto Y, et al. Treatment of gastric and gastroesophageal cancer patients with hemodialysis by CapeOX. Intern Med. 2019;58:2791-2795.
- Funasaka C, Kanemasa Y, Shimoyama T, et al. Modified FOLFOX-6 plus bevacizumab chemotherapy for metastatic colorectal cancer in patients receiving hemodialysis: a report of three cases and review of the literature. Case Rep Oncol. 2019;12:657-665.
- Maruta M, Miyoshi T, Matsuo N, et al. Clinical pharmacokinetics of oxaliplatin in a hemodialysis patient with advanced gastric cancer. J Chemother. 2021;33:51-55.
- Horimatsu T, Miyamoto S, Morita S, et al. Pharmacokinetics of oxaliplatin in a hemodialytic patient treated with modified FOLFOX-6 plus bevacizumab therapy. Cancer Chemother Pharmacol. 2011;68:263-266.
- Budakoglu B, Abali H, Uncu D, et al. Good tolerance of weekly irinotecan in a patient with metastatic colorectal cancer on chronic hemodialysis. J Chemother. 2005;17:452-453.
- Verwimp J, Geurs F, Ponette S, et al. Complete response of a metastatic gastroesophageal adenocarcinoma on irinotecan-based chemotherapy in a dialysis patient. Int J Nephrol Renovasc Dis. 2010;3:61-64.
- Cercek A, Park V, Yaeger R, et al. Faster FOLFOX: oxaliplatin can be safely infused at a rate of 1 mg/m2/min. J Oncol Pract. 2016;12:e548-e553.
- Kobayashi M, Endo S, Hamano Y, et al. Successful treatment with modified FOLFOX6 and panitumumab in a cecal cancer patient undergoing hemodialysis. Intern Med. 2016;55:127-130.
- Singh A, Patel K, Chou L, et al. Factors affecting the development of irinotecan-associated acute cholinergic syndrome. J Clin Oncol. 2018;36(15 suppl):Abstract e14515.
- Department of Health & Human Services. Common Terminology Criteria for Adverse Events (CTCAE). Version 5.0. November 27, 2017. https://ctep.cancer.gov/protocoldevelopment/electronic_applications/docs/CTCAE_v5_Quick_Reference_8.5x11.pdf. Accessed October 20, 2020.
- Suker M, Beumer BR, Sadot E, et al. FOLFIRINOX for locally advanced pancreatic cancer: a systematic review and patient-level meta-analysis. Lancet Oncol. 2016;17:801-810.
- Vénat-Bouvet L, Saint-Marcoux F, Lagarde C, et al. Irinotecan-based chemotherapy in a metastatic colorectal cancer patient under haemodialysis for chronic renal dysfunction: two cases considered. Anticancer Drugs. 2007;18:977-980.
- Stemmler J, Weise A, Hacker U, et al. Weekly irinotecan in a patient with metastatic colorectal cancer on hemodialysis due to chronic renal failure. Onkologie. 2002;25:60-63.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines): Antiemesis. Version 2.2022. March 23, 2022. www.nccn.org/professionals/physician_gls/pdf/antiemesis.pdf. Accessed November 28, 2022.
- Janus N, Thariat J, Boulanger H, et al. Proposal for dosage adjustment and timing of chemotherapy in hemodialyzed patients. Ann Oncol. 2010;21:1395-1403.
- Mahaseth H, Brutcher E, Kauh J, et al. Modified FOLFIRINOX regimen with improved safety and maintained efficacy in pancreatic adenocarcinoma. Pancreas. 2013;42:1311-1315.
- Saif MW. Capecitabine and hand–foot syndrome. Expert Opin Drug Saf. 2011;10:159-169.